## Clinical Assessment This patient has a **positive FAST examination** (free fluid in left paracolic gutter and pelvis) indicating intra-abdominal bleeding, but remains **haemodynamically stable** (BP 110/70, HR 102). This is the key distinction that guides management. ## FAST Interpretation **Key Point:** A positive FAST in a stable patient does NOT mandate immediate laparotomy. FAST detects free fluid (blood, urine, bile) but does not identify the source or quantify bleeding. ## Management Algorithm for Blunt Abdominal Trauma ```mermaid flowchart TD A[Blunt abdominal trauma + FAST positive]:::outcome --> B{Haemodynamically stable?}:::decision B -->|No - Shock/unstable| C[Immediate exploratory laparotomy]:::urgent B -->|Yes - Stable vitals| D[CT abdomen/pelvis with contrast]:::action D --> E{CT shows solid organ injury?}:::decision E -->|Yes| F[ICU admission + close monitoring]:::action E -->|No| G[Discharge if other injuries excluded]:::action F --> H{Deterioration or peritonitis?}:::decision H -->|Yes| I[Delayed laparotomy]:::urgent H -->|No| J[Conservative management]:::action ``` ## Why CT is Superior to DPL | Feature | FAST | CT | DPL | |---------|------|----|---------| | **Sensitivity for free fluid** | 73–97% | 95–100% | 90–97% | | **Identifies solid organ injury** | No | Yes (grade, location) | No | | **Quantifies bleeding** | No | Yes (volume estimate) | Semi-quantitative | | **Non-invasive** | Yes | Yes | No (invasive) | | **Repeat exams** | Easy | Easy | Single use | **High-Yield:** In a **stable patient with positive FAST**, CT is the gold standard because it: 1. Confirms the source of bleeding (spleen, liver, kidney, mesentery) 2. Grades solid organ injury (helps predict need for intervention) 3. Allows selective non-operative management (NOM) of Grade I–III injuries 4. Detects hollow viscus injury (pancreatic, bowel trauma) ## Indications for Immediate Laparotomy **Key Point:** Laparotomy is indicated when: - **Haemodynamic instability** (SBP < 90 mmHg, ongoing shock despite resuscitation) - **Peritoneal signs** (guarding, rigidity, rebound tenderness) - **Evisceration** or penetrating trauma with peritoneal violation - **Positive FAST + unstable** (no time for CT) This patient has none of these — he is compensating well. ## Non-Operative Management (NOM) in Blunt Abdominal Trauma **Clinical Pearl:** Modern trauma practice favours **selective NOM** for stable patients with blunt solid organ injury (spleen, liver, kidney injuries Grade I–III). Success rates exceed 90% if: - Patient remains haemodynamically stable - No peritonitis develops - ICU/high-dependency unit (HDU) monitoring available - Surgeon immediately available if deterioration occurs **Mnemonic: STABLE NOM** — **S**table vitals, **T**rusted imaging (CT), **A**bdominal exam serial, **B**lood available, **L**evel-1 facility, **E**xperienced team. ## Why Other Options Are Incorrect **Immediate laparotomy (Option A):** Reserved for haemodynamically unstable patients or those with peritonitis. This patient is compensating; premature surgery increases morbidity (adhesions, infection) without benefit. **DPL (Option D):** Largely obsolete. DPL is invasive, non-specific (cannot identify source), and inferior to CT. It may be used only if CT is unavailable and clinical suspicion is very high. [cite:ATLS 10th Edition Ch 5; Sabiston Textbook of Surgery 21e Ch 19] 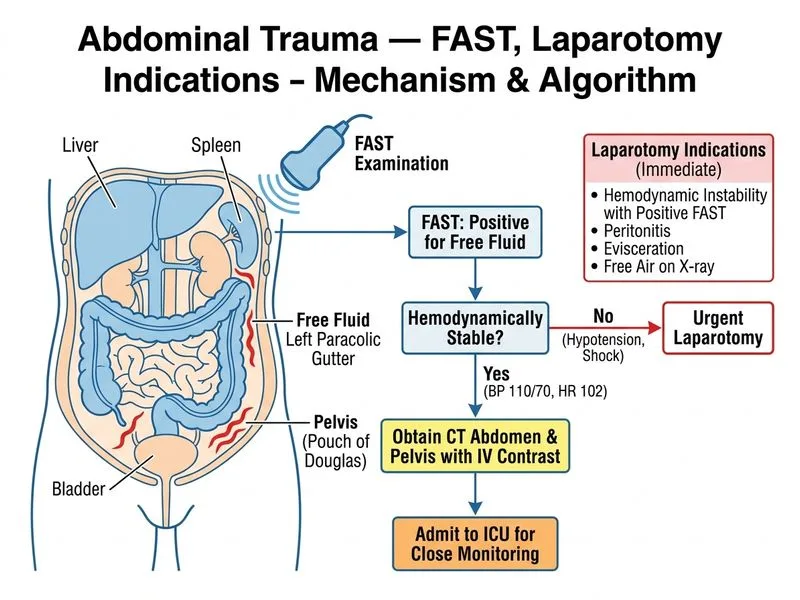
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.