## Discriminating Feature: Haemodynamic Stability and Peritoneal Signs ### Rationale for Correct Answer **Key Point:** The single most important discriminator between operative and non-operative management in blunt abdominal trauma is **haemodynamic stability** combined with **absence of peritoneal signs** (guarding, rigidity, rebound tenderness). **High-Yield:** Modern trauma management follows the **Selective Non-Operative Management (SNOM)** protocol for haemodynamically stable patients with solid organ injuries, regardless of FAST positivity or CT grade. ### Why Each Finding Matters | Finding | Role in Decision-Making | Operative Threshold | |---------|------------------------|---------------------| | Free fluid on FAST | Indicates bleeding but NOT an absolute indication for surgery in stable patients | Unstable patient + free fluid = laparotomy | | Haemodynamic stability + no peritoneal signs | Permits observation, serial exams, ICU monitoring | **BEST discriminator** — allows SNOM | | CT grade (I–V) | Prognostic; guides ICU level but does NOT mandate surgery if stable | Grade III–V stable = SNOM candidate | | Volume of free fluid | Correlates with bleeding severity but is imprecise; not a threshold value | Subjective; used with clinical signs | ### Clinical Algorithm ```mermaid flowchart TD A[Blunt abdominal trauma]:::outcome --> B{Haemodynamically stable?}:::decision B -->|No| C[Resuscitate + FAST]:::action C --> D{Free fluid + unstable?}:::decision D -->|Yes| E[Immediate laparotomy]:::urgent D -->|No| F[Resuscitate further]:::action B -->|Yes| G{Peritoneal signs?}:::decision G -->|Yes| H[Laparotomy]:::urgent G -->|No| I[FAST + CT imaging]:::action I --> J[SNOM protocol]:::action J --> K[Serial exams, ICU, transfusion threshold]:::action ``` ### SNOM Criteria (Stable Patient) 1. **Haemodynamic stability** — SBP > 90 mmHg, HR < 120 bpm, no ongoing shock 2. **No peritoneal signs** — no guarding, rigidity, or rebound 3. **Reliable examination** — alert, cooperative, no distracting injuries 4. **ICU/high-dependency bed** — for continuous monitoring 5. **Transfusion threshold** — typically 2–4 units before escalation to surgery **Clinical Pearl:** A patient with Grade III–V splenic laceration and free fluid can be managed non-operatively if haemodynamically stable and without peritoneal signs. This approach preserves splenic function and avoids unnecessary laparotomy. **Warning:** Haemodynamic instability (SBP < 90 mmHg, persistent tachycardia despite resuscitation, or peritoneal signs) overrides all other findings and mandates immediate laparotomy. [cite:ATLS 10e Ch 5, Harrison 21e Ch 297] 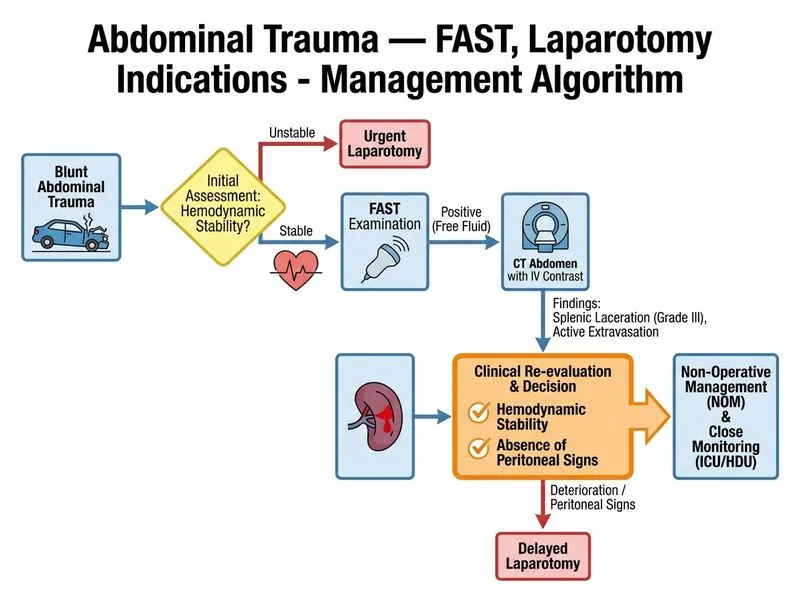
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.