## Splenic Injury Grading and Non-Operative Management **Key Point:** The AAST Organ Injury Scale is the standardized, evidence-based grading system used globally to classify splenic injuries and guide non-operative management protocols. ### AAST Splenic Injury Grading | Grade | Injury Type | Management Approach | | --- | --- | --- | | I | Haematoma < 10% surface area; Laceration < 1 cm depth | Observation, ICU/HDU monitoring | | II | Haematoma 10–50% surface area; Laceration 1–3 cm depth | Observation, ICU/HDU monitoring | | III | Haematoma > 50% surface area; Laceration > 3 cm depth | Observation ± angiographic embolization | | IV | Laceration involving hilar vessels; Devascularization > 25% | Observation ± angiographic embolization; Consider splenectomy | | V | Complete splenic devascularization; Shattered spleen | Splenectomy (usually mandatory) | **High-Yield:** Grades I–III are successfully managed non-operatively in haemodynamically stable patients with ICU/HDU monitoring and serial clinical examination. Angiographic embolization is increasingly used for Grade III–IV injuries to avoid splenectomy. **Clinical Pearl:** The success of non-operative splenic management depends on: - Haemodynamic stability - Absence of peritoneal signs - Availability of ICU/HDU monitoring - Access to interventional radiology for embolization - Willingness to perform emergency splenectomy if deterioration occurs **Mnemonic:** AAST = **A**merican **A**ssociation for the **S**urgery of **T**rauma — the gold standard for organ injury classification in trauma. [cite:ATLS 10e; American College of Surgeons] 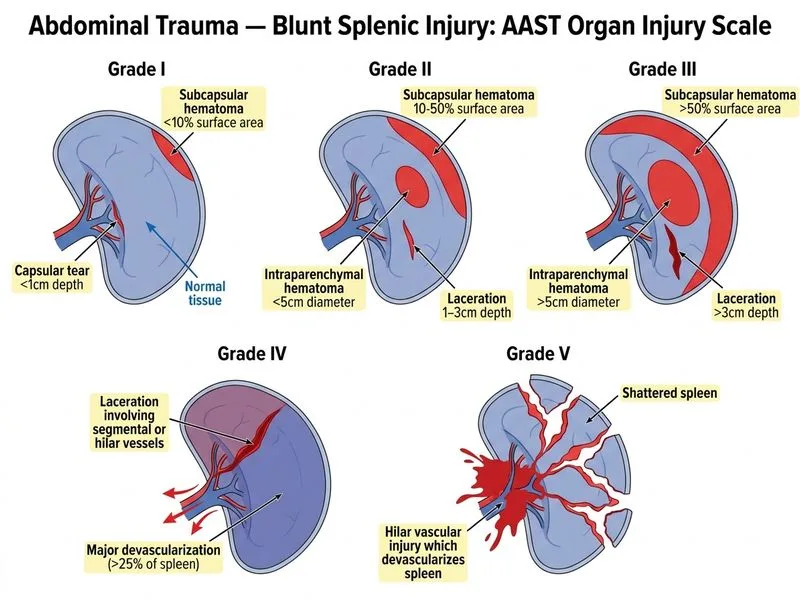
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.