## Management of Blunt Splenic Injury — Grade III with Active Extravasation ### Current Evidence for Splenic Artery Embolization (SAE) **Key Point:** In a haemodynamically stable patient with a Grade III splenic laceration and **active contrast extravasation ("blush")** on CT, splenic artery embolization (SAE) is the preferred intervention. Active extravasation indicates ongoing arterial bleeding and is a well-established indication for angioembolization in stable patients, allowing splenic preservation while controlling haemorrhage. **High-Yield:** The Eastern Association for the Surgery of Trauma (EAST) and the World Society of Emergency Surgery (WSES) guidelines recommend angioembolization as the primary intervention for haemodynamically stable patients with splenic injuries showing active extravasation on CT, regardless of grade. SAE reduces the failure rate of non-operative management (NOM) from ~20–30% to <10% in this subset. ### Management Algorithm for Blunt Splenic Injury ```mermaid flowchart TD A[Blunt splenic injury on CT]:::outcome --> B{Haemodynamically stable?}:::decision B -->|No, refractory shock| C[Immediate Splenectomy / OR]:::action B -->|Yes, stable| D{Active extravasation on CT?}:::decision D -->|No| E[NOM: ICU observation, serial exam, cross-matched blood]:::action D -->|Yes| F[Urgent CT Angiography + Splenic Artery Embolization]:::action F --> G{Post-SAE monitoring}:::decision G -->|Stable| H[ICU observation, serial exam]:::outcome G -->|Deterioration| I[Operative intervention / Splenectomy]:::urgent ``` ### Criteria Guiding the Choice Between Pure Observation vs. SAE | Feature | Pure NOM (Observation) | SAE Indicated | | --- | --- | --- | | **Haemodynamic status** | Stable | Stable | | **CT finding** | No active extravasation | **Active extravasation ("blush")** | | **Injury grade** | Grade I–II (selected III) | Grade III–V with blush | | **Goal** | Expectant monitoring | Haemorrhage control + splenic preservation | | **Failure rate without SAE** | Low (~5%) | High (~25–30%) | **Clinical Pearl:** The presence of a **contrast blush (active extravasation)** on CT is the critical differentiator. Without a blush, Grade III injuries can be managed with observation alone. With a blush, SAE is the standard of care in haemodynamically stable patients — it controls bleeding, preserves the spleen, and dramatically reduces NOM failure rates (WSES Guidelines 2017; Coccolini et al., *World J Emerg Surg* 2017). ### Why Option D (SAE) is Correct This patient has: - Haemodynamic stability (BP 110/70, HR 88) — rules out immediate splenectomy - Grade III laceration **with active extravasation** — this is the key finding that mandates intervention beyond simple observation - No indication for diagnostic laparoscopy (CT has already characterised the injury) The correct next step is **urgent CT angiography with splenic artery embolization**, which: 1. Confirms the bleeding vessel anatomy 2. Allows selective or proximal embolization to arrest haemorrhage 3. Preserves splenic immunological function 4. Avoids the morbidity of splenectomy in a young patient ### Why the Other Options Are Incorrect - **Option A (Diagnostic laparoscopy + splenectomy):** Laparoscopy is not indicated when CT has already characterised the injury; splenectomy is not the first choice in a stable patient. - **Option B (Observation alone):** Appropriate for stable patients *without* active extravasation. The presence of a contrast blush mandates intervention — pure observation carries an unacceptably high failure rate (~25–30%) in this setting. - **Option C (Immediate splenectomy):** Reserved for haemodynamically unstable patients who do not respond to resuscitation. This patient is stable. **Reference:** Coccolini F et al. Splenic trauma: WSES classification and guidelines for adult and pediatric patients. *World J Emerg Surg.* 2017;12:40. Also: EAST Practice Management Guidelines for Blunt Splenic Injury. 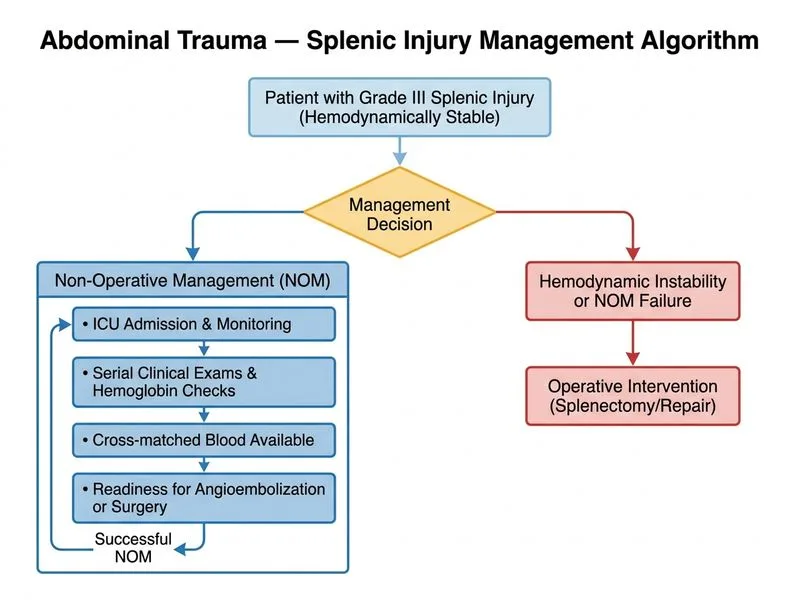
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.