## Management of Blunt Pancreatic Injury with Ductal Disruption ### Pancreatic Injury Grading and Ductal Involvement **Key Point:** Pancreatic injuries with ductal disruption (Grade III–V) require operative intervention. The presence of ductal injury is the critical factor determining need for surgery — **haemodynamic stability does NOT eliminate the need for surgery**, and **normal serum amylase does NOT exclude ductal injury** (sensitivity of amylase for ductal disruption is only ~60–70%). **High-Yield:** Blunt pancreatic injury is rare (0.5–1% of abdominal trauma) but carries high morbidity if ductal injury is missed. Ductal disruption leads to pancreatic fistula, abscess, and pseudocyst formation if not addressed operatively. ### Pancreatic Injury Grading (AAST) | Grade | Injury Description | Management | | --- | --- | --- | | **I** | Contusion/haematoma, no ductal injury | Observation | | **II** | Laceration <50% parenchyma, no ductal injury | Observation | | **III** | Laceration >50% parenchyma OR distal ductal injury | Distal pancreatectomy ± splenectomy | | **IV** | Laceration with proximal ductal disruption or ampullary involvement | **Operative repair / damage control** | | **V** | Pancreatic head destruction / massive injury | Whipple (rarely) or damage control | ### Why Option A (Exploratory Laparotomy) is the Best Next Step This patient has: - **Grade IV pancreatic laceration** — major parenchymal injury with **proximal/major ductal disruption** - **Peripancreatic fluid collection** — radiological sign of ductal disruption - **Haemodynamic stability** — allows planned operative intervention rather than damage-control-only approach The "best next step" in a haemodynamically stable patient with confirmed Grade IV ductal injury is **exploratory laparotomy** to: 1. Directly assess the extent and location of ductal injury (Kocher maneuver, intraoperative pancreatography if needed) 2. Perform definitive repair based on intraoperative findings: - **Distal duct injury** → Distal pancreatectomy ± splenectomy - **Proximal/body duct injury** → Primary repair with external drainage ± ERCP stent as adjunct 3. Debride devitalized tissue and drain peripancreatic collection ### Why the Other Options Are Incorrect - **Option B (Distal pancreatectomy with splenectomy):** This is the correct *definitive procedure* for **distal** (body/tail) ductal injuries (Grade III). However, the stem specifies Grade IV injury with major ductal disruption — the location is not specified as distal, and committing to distal pancreatectomy without exploratory assessment risks inappropriate management of a proximal injury. The **best next step** is laparotomy to assess and then decide; distal pancreatectomy may be the outcome of that laparotomy, but it is not the next step. - **Option C (ERCP + stent + percutaneous drainage):** ERCP with stenting is appropriate for **Grade III injuries** with minor/distal ductal disruption in stable patients, or as an adjunct post-operatively. It is **not** the primary management for Grade IV major ductal injury, where operative control is required (Cameron & Current Surgical Therapy, 13th ed.). - **Option D (Observation + serial amylase):** Observation is appropriate only for Grade I–II injuries without ductal involvement. **Normal amylase does NOT exclude ductal injury** — up to 40% of patients with ductal disruption have normal initial amylase. Observation in Grade IV injury risks pancreatic fistula, abscess, and pseudocyst with 30–40% mortality if untreated. **Clinical Pearl (Harrison's / Schwartz's Principles of Surgery):** In blunt pancreatic trauma, the single most important determinant of management is **ductal integrity**. CT findings of peripancreatic fluid, laceration depth >50%, and Grade IV classification mandate operative exploration regardless of haemodynamic status or amylase level. **Warning:** Delaying surgery in confirmed Grade IV ductal injury — even in a stable patient — significantly increases the risk of pancreatic fistula, infected necrosis, and mortality. 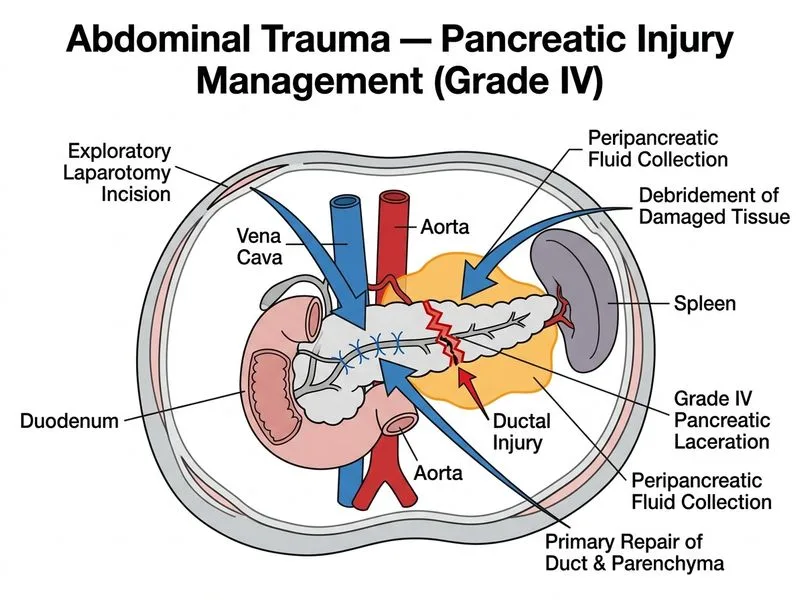
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.