## Management of Blunt Renal Trauma — Grade III Laceration ### Renal Injury Grading (American Association for the Surgery of Trauma) | Grade | Injury Description | Imaging Findings | |-------|-------------------|------------------| | I | Contusion or minor laceration | Hematuria, no laceration on imaging | | II | Laceration <1 cm depth, no collecting system injury | Cortical laceration, contained hematoma | | III | Laceration >1 cm depth without collecting system injury | Deep laceration, perinephric hematoma, no extravasation | | IV | Laceration involving collecting system OR vascular injury | Urine extravasation OR renal artery/vein injury | | V | Shattered kidney OR renal artery/vein injury | Fragmentation OR vascular injury | **Key Point:** This patient has a **Grade III renal injury** — a deep laceration with contained perinephric hematoma but **no collecting system disruption and no active extravasation**. These are the hallmarks of an injury suitable for **non-operative management (NOM)**. ### Indications for Non-Operative Management of Renal Trauma 1. **Hemodynamic stability** (this patient: BP 118/74, HR 88) ✓ 2. **No peritoneal signs** (no mention of peritonitis) ✓ 3. **Contained hematoma** (perinephric, not extraperitoneal) ✓ 4. **No collecting system disruption** (confirmed on CT) ✓ 5. **No active extravasation** (confirmed on CT) ✓ 6. **Ability to monitor closely** (ICU/high-dependency unit available) ✓ ### Non-Operative Management Protocol ```mermaid flowchart TD A[Blunt renal trauma]:::outcome --> B{Hemodynamically<br/>stable?}:::decision B -->|No| C[Resuscitate + consider<br/>operative exploration]:::urgent B -->|Yes| D{Grade of injury<br/>on CT?}:::decision D -->|Grade I-III,<br/>no collecting system<br/>injury| E[Bed rest,<br/>analgesia,<br/>NPO initially]:::action D -->|Grade IV-V or<br/>collecting system<br/>injury| F[Operative exploration<br/>± nephrectomy]:::urgent E --> G[Serial clinical exams<br/>+ vitals monitoring]:::action G --> H{Deterioration?}:::decision H -->|Fever, pain,<br/>hemodynamic change| I[Repeat imaging<br/>± intervention]:::action H -->|Stable| J[Gradual mobilization<br/>after 48-72 hrs]:::action I --> K{Active bleeding<br/>or infection?}:::decision K -->|Yes| L[Angiographic embolization<br/>or nephrectomy]:::urgent K -->|No| J ``` ### Key Management Points **High-Yield:** The **vast majority** (>95%) of **Grade I–III renal injuries** in hemodynamically stable patients are managed **conservatively** without operative intervention. Nephrectomy is reserved for: - Hemodynamic instability unresponsive to resuscitation - Grade IV–V injuries (collecting system disruption, vascular injury) - Complications during observation (sepsis, uncontrolled bleeding) **Clinical Pearl:** **Bed rest** is the cornerstone of early management: - Keeps intra-renal pressure low - Reduces risk of hematoma expansion - Duration: typically 48–72 hours, then gradual mobilization if stable **Mnemonic:** **STABLE KIDNEY** = **S**table hemodynamics, **T**ained (contained) hematoma, **A**no collecting system injury, **B**lunt trauma, **L**ow-grade (I–III), **E**xpectant management, **K**eep in bed, **I**maging follow-up if deteriorates, **D**rain only if infected, **N**ephrectomy only if unstable, **E**arly mobilization if stable, **Y**ield to observation. ### Monitoring During Observation 1. **Vital signs:** Hourly for first 24 hours, then 4-hourly 2. **Abdominal examination:** Serial exams for peritonitis, flank tenderness 3. **Urine output:** Monitor for hematuria resolution (usually clears within 48 hours) 4. **Repeat imaging:** Only if clinical deterioration (fever, hemodynamic instability, increasing pain) 5. **Activity:** Bed rest for 48–72 hours, then gradual mobilization ### Why This Option Is Correct This patient meets **all criteria for non-operative management**: - Hemodynamically stable - Grade III injury (deep laceration but no collecting system disruption) - Contained perinephric hematoma - No active extravasation - No peritoneal signs Conservative management preserves renal function, avoids operative morbidity, and has excellent outcomes (>95% success rate) in appropriately selected patients. 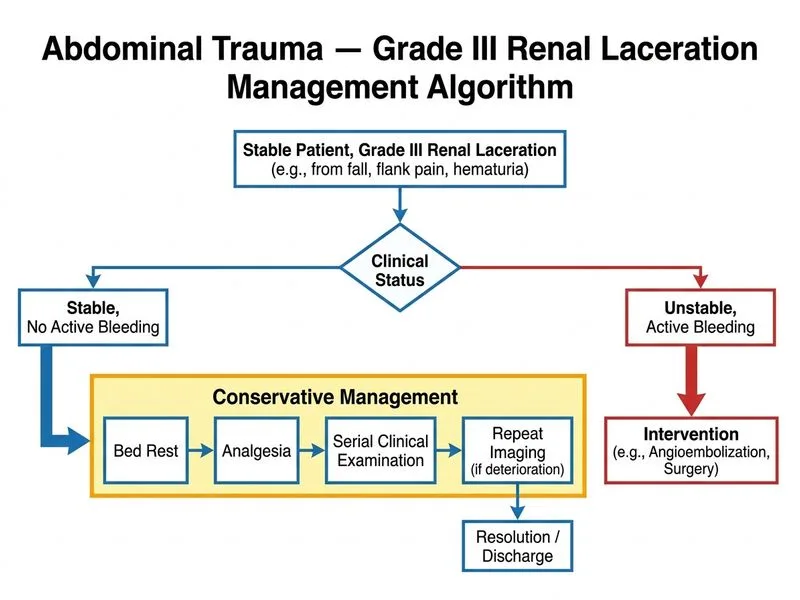
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.