## Management of Blunt Hepatic Injury ### Key Principles in Penetrating Liver Trauma **Key Point:** In penetrating trauma to the liver, the decision between operative and non-operative management depends on haemodynamic stability, peritoneal signs, and imaging findings. Haemodynamically stable patients with isolated liver injuries and no peritoneal signs can be managed non-operatively [cite:ATLS 10th Edition]. ### Classification of Hepatic Injuries | Grade | Injury | Mortality (Blunt) | |-------|--------|-------------------| | I | Laceration <1 cm, haematoma <10% surface | <5% | | II | Laceration 1–3 cm, haematoma 10–50% surface | <5% | | III | Laceration >3 cm, haematoma >50% surface | 5–10% | | IV | Laceration involving hepatic vein or >75% parenchyma | 10–15% | | V | Juxtahepatic venous injury, hepatic avulsion | 25–50% | | VI | Hepatic vein injury at IVC junction | >50% | **High-Yield:** In this case, the injury is Grade I–II (small laceration, no active bleeding, no biloma), making it ideal for non-operative management. ### Criteria for Non-Operative Management in Penetrating Liver Injury 1. **Haemodynamic stability** (BP >90 mmHg, HR <120/min) 2. **No peritoneal signs** (rebound, rigidity, guarding) 3. **FAST negative** (no free fluid) 4. **CT imaging** showing isolated liver injury without active extravasation 5. **Reliable patient** for serial examination 6. **ICU/HDU availability** with immediate surgical backup ### Management Protocol **Clinical Pearl:** Non-operative management of hepatic injuries has a success rate >95% in carefully selected, haemodynamically stable patients. 1. **Immediate phase:** - ICU/HDU admission - Continuous monitoring (BP, HR, O₂ sat) - Two large-bore IV lines, cross-matched blood available - NPO status 2. **First 24–48 hours:** - Bed rest (no mobilization) - Serial abdominal examination q2–4h - Serial haemoglobin (baseline, 6h, 12h, 24h) - Repeat imaging only if clinical deterioration 3. **Days 2–7:** - Gradual mobilization if stable - Oral intake when stable - Discharge with activity restriction (6–8 weeks) ### Indications for Conversion to Surgery - Haemodynamic instability despite resuscitation - Peritoneal signs (rebound, rigidity) - Decreasing haemoglobin despite transfusion - Evidence of biliary peritonitis (fever, elevated WBC) - Pseudoaneurysm on imaging ### Why This Patient Qualifies for NOM - Haemodynamically stable (BP 118/76, HR 98) - Minimal peritoneal irritation (no rebound/rigidity) - FAST negative (no free fluid) - CT shows small laceration, no active bleeding, no biloma - Reliable for examination --- ## Decision Algorithm ```mermaid flowchart TD A[Penetrating liver injury]:::outcome --> B{Haemodynamically stable?}:::decision B -->|No| C[Resuscitate]:::action C --> D{Response to fluids?}:::decision D -->|No| E[Exploratory laparotomy]:::urgent D -->|Yes| F[Reassess] B -->|Yes| G{Peritoneal signs or FAST+?}:::decision G -->|Yes| E G -->|No| H[CT imaging]:::action H --> I{Active bleeding or high-grade injury?}:::decision I -->|Yes| E I -->|No| J[Non-operative management]:::action J --> K[ICU, serial exam, bed rest]:::action K --> L{Clinical deterioration?}:::decision L -->|Yes| E L -->|No| M[Discharge with restrictions]:::outcome ``` ### Why Not Diagnostic Laparoscopy? **Tip:** Diagnostic laparoscopy is NOT indicated in this patient because: - FAST is negative (no free fluid) - CT has already defined the injury - No peritoneal signs suggesting other injuries - Laparoscopy adds operative risk without diagnostic benefit in a stable patient ### Why Not Percutaneous Drainage? - No biloma or fluid collection present on imaging - Drainage is reserved for infected collections (biloma, abscess) - Not indicated for simple lacerations without fluid accumulation 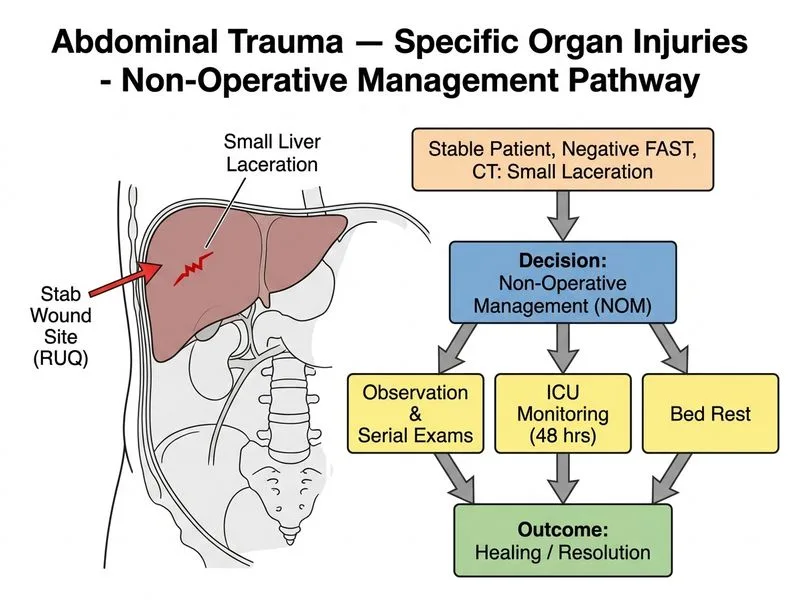
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.