## Clinical Assessment **Key Point:** Haemodynamic instability in the setting of blunt abdominal trauma with imaging evidence of active extravasation is an absolute indication for emergency surgical intervention. ### Indicators for Operative Management | Factor | Status | Implication | | --- | --- | --- | | Haemodynamic stability | Unstable (SBP 95) despite resuscitation | Mandatory OR | | FAST findings | Positive (free fluid) | Intra-abdominal bleeding | | CT findings | Active extravasation from spleen | Ongoing hemorrhage | | Pancreatic injury | Main duct disruption | Requires definitive repair | | Transfusion requirement | 2 units PRBC already given | Significant blood loss | **High-Yield:** The combination of **haemodynamic instability + active extravasation on CT** mandates immediate laparotomy. Non-operative management is only appropriate in haemodynamically *stable* patients with blunt splenic injury. ### Why Splenectomy Is Indicated Here 1. Active extravasation indicates ongoing hemorrhage that cannot be controlled conservatively 2. Shattered spleen (Grade V) with instability is not amenable to splenic-preserving repair 3. Pancreatic main duct disruption requires operative exploration and drainage/repair **Clinical Pearl:** In unstable patients with blunt splenic trauma, splenectomy is faster and more reliable than attempting splenic repair, which can delay hemorrhage control and increase mortality. ### Pancreatic Considerations Main pancreatic duct injury requires: - Operative visualization and assessment - Distal pancreatectomy if the injury is in the body/tail - Drainage (closed suction drain) if repair is attempted - Avoidance of primary repair of duct injuries (high morbidity) **Mnemonic:** **UNSTABLE + ACTIVE BLEED = OR** — Haemodynamic instability with active extravasation is never managed non-operatively. [cite:ATLS 10th Edition Ch 8] 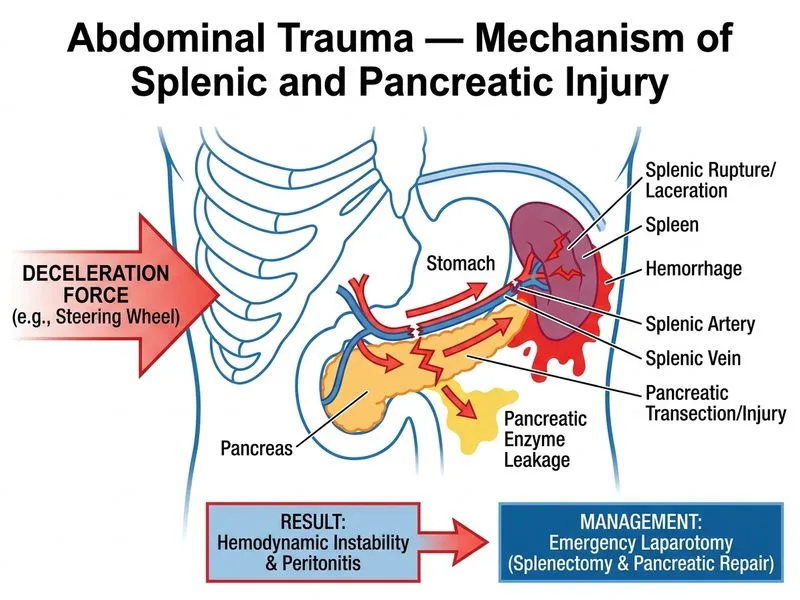
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.