## Diagnostic Approach to Acanthosis Nigricans ### Role of Skin Biopsy **Key Point:** Skin biopsy is the gold standard for confirming acanthosis nigricans histologically and ruling out malignant transformation or other dermatoses. **Histopathological Features:** - Hyperkeratosis (often papillomatous) - Acanthosis (thickened epidermis) - Hyperpigmentation of basal layer - Preserved dermal–epidermal interface - Absence of malignant cells ### Why Biopsy is Essential **Clinical Pearl:** While acanthosis nigricans is clinically recognizable in most cases, biopsy becomes crucial when: 1. Diagnosis is uncertain 2. Rapid onset or atypical morphology raises concern for malignancy-associated variant 3. Patient anxiety about malignant potential is high 4. Lesions show unusual features (erosion, ulceration, bleeding) **High-Yield:** Acanthosis nigricans can be associated with internal malignancy in 5–10% of cases (gastric, lung, breast, ovarian cancers). Biopsy helps exclude malignant infiltration or paraneoplastic transformation. ### Differential Diagnosis on Histology | Feature | Benign Acanthosis Nigricans | Malignancy-Associated | Pseudoacanthosis Nigricans | |---------|------------------------------|----------------------|---------------------------| | Epidermal thickening | Marked | Marked | Minimal | | Dermal infiltrate | Absent | Present (lymphocytes, tumor cells) | Absent | | Basal pigmentation | Increased | Increased | Normal | | Atypia | None | May be present | None | **Warning:** Clinical appearance alone cannot reliably distinguish benign from malignancy-associated acanthosis nigricans; histology is mandatory for definitive diagnosis. 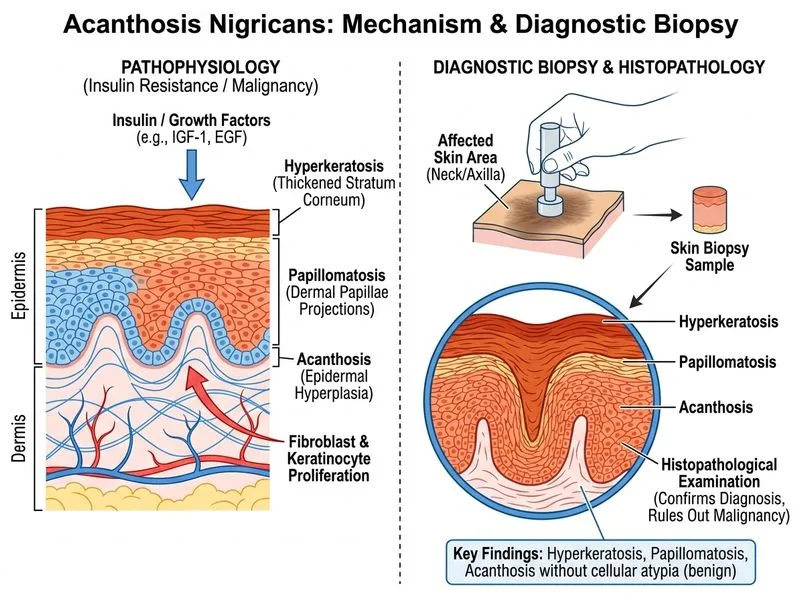
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.