## Diagnosis: Benign Acanthosis Nigricans (Metabolic Type) ### Clinical Context This patient presents with AN in the setting of: 1. **Long-standing type 2 diabetes** (15 years) 2. **Gradual onset** (2 years of progression) 3. **Stable weight** and no systemic B symptoms 4. **Normal imaging** (no malignancy detected) 5. **Hyperinsulinemia** (implied by need for dual antidiabetic therapy) ### Pathophysiology of Benign AN **Key Point:** Benign AN is driven by **chronic hyperinsulinemia and insulin resistance**, not malignancy. Elevated insulin levels stimulate insulin-like growth factor-1 (IGF-1) receptors on keratinocytes and melanocytes, leading to epidermal proliferation and melanin deposition. ### Benign vs. Malignant Acanthosis Nigricans | Feature | Benign AN | Malignant AN | |---|---|---| | **Onset** | Gradual (months to years) | Acute (weeks to months) | | **Associated condition** | Obesity, diabetes, PCOS, metabolic syndrome | Malignancy (90% of cases) | | **Progression** | Stable or slow | Rapid | | **Age of onset** | Usually < 40 years | Usually > 50 years | | **Systemic symptoms** | None | Weight loss, abdominal pain, B symptoms | | **Imaging findings** | Normal | Malignancy on imaging/endoscopy | | **Prognosis** | Improves with weight loss and glycemic control | Depends on underlying malignancy | | **Response to treatment** | Good response to insulin sensitizers | Poor response to metabolic treatment | **High-Yield:** The **15-year diabetes history + gradual 2-year progression + stable weight + normal imaging** is the diagnostic constellation for benign AN. This patient does NOT fit the malignant profile (acute onset, weight loss, imaging abnormality). ### Mechanism in Type 2 Diabetes 1. Insulin resistance → compensatory hyperinsulinemia 2. Elevated fasting insulin (likely > 15 mIU/L in this patient) 3. IGF-1 and insulin bind to growth factor receptors on skin 4. Keratinocyte proliferation → acanthosis 5. Melanocyte stimulation → hyperpigmentation **Clinical Pearl:** Benign AN often improves with: - Weight loss (even 5–10%) - Improved glycemic control (HbA1c < 7%) - Addition of insulin sensitizers (metformin, thiazolidinediones) ### Why Imaging Is Reassuring The **unremarkable chest X-ray and abdominal ultrasound** effectively exclude occult malignancy in this case. In benign AN, imaging is normal by definition. **Mnemonic for AN Workup:** **MASS** = Malignancy screening, Age (acute onset?), Systemic symptoms (weight loss?), Stable imaging = Benign AN 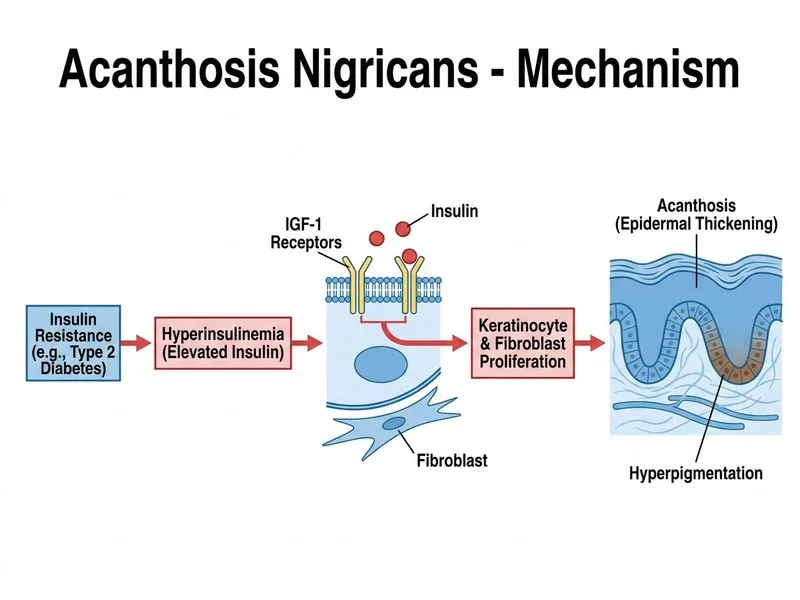
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.