## Distinguishing Acanthosis Nigricans: Insulin Resistance vs. Paraneoplastic ### Clinical Presentation Comparison | Feature | Insulin Resistance–Associated | Paraneoplastic | |---------|-------------------------------|----------------| | **Onset** | Gradual (months to years) | Rapid (weeks to months) | | **Distribution** | Flexural (neck, axillae, groin, inframammary) | Widespread (palms, soles, mucosa, dorsal surfaces) | | **Associated findings** | Obesity, hypertension, dyslipidemia, PCOS, acne, hirsutism | Weight loss, systemic symptoms, malignancy signs | | **Prognosis** | Improves with weight loss and glycemic control | Parallels malignancy course | | **Malignancy risk** | <1% | 50–90% (gastric, lung, breast, ovarian) | ### Key Point: **Insulin resistance–associated acanthosis nigricans is characterized by gradual onset, flexural distribution, and metabolic comorbidities (obesity, diabetes, dyslipidemia, PCOS).** The paraneoplastic variant presents acutely with widespread distribution including palms, soles, and mucous membranes, and is accompanied by systemic symptoms and weight loss. ### High-Yield: In this patient with type 2 diabetes, HbA1c 11.2%, and classic flexural distribution (neck, axillae), the **gradual onset with metabolic abnormalities** is the key discriminator pointing to insulin resistance–associated disease rather than paraneoplastic acanthosis nigricans. ### Clinical Pearl: The presence of **lichenification and pruritus** occurs in both forms. **Hyperkeratosis and follicular plugging** are non-specific histologic findings. The **rapid onset with palms/soles involvement** is the hallmark of paraneoplastic disease and warrants urgent malignancy screening. 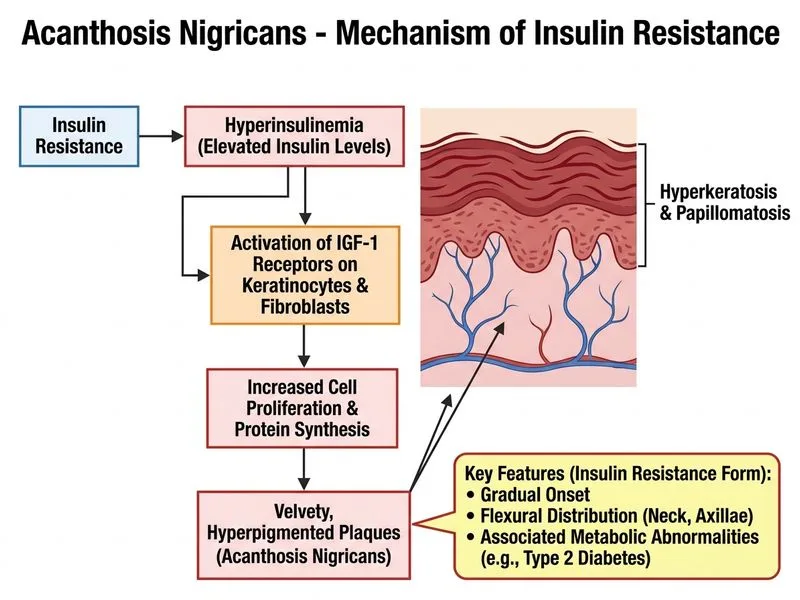
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.