## Clinical Diagnosis: Benign Acanthosis Nigricans ### Presentation Analysis This patient presents with acanthosis nigricans (velvety hyperpigmented skin in flexural areas) in the **absence of systemic alarm features**. The key discriminating factors are: - **Gradual onset** (6 months) - **Obesity** (BMI 32 kg/m²) - **Prediabetic range glucose** (HbA1c 6.8%) - **No weight loss** - **Normal malignancy screening** (pelvic ultrasound, mammography) ### Pathophysiology of Benign Acanthosis Nigricans **Key Point:** Benign AN is driven by **hyperinsulinemia and insulin resistance**, not malignancy. The mechanism involves: 1. **Insulin resistance** → compensatory hyperinsulinemia 2. **Elevated insulin levels** → activation of insulin-like growth factor-1 (IGF-1) receptors on keratinocytes 3. **Keratinocyte proliferation** → acanthosis (thickening) and hyperpigmentation 4. **Exaggerated dermatoglyphics** → characteristic velvety appearance ### Classification of Acanthosis Nigricans | Feature | Benign AN | Malignant AN | |---------|-----------|-------------| | **Onset** | Gradual (months to years) | Rapid (< 1 year) | | **Associated symptoms** | Weight gain or stable weight | Weight loss, systemic symptoms | | **BMI** | Usually elevated (> 25) | Variable | | **Malignancy** | None | Present (gastric, lung, breast, pancreatic) | | **Response to treatment** | Improves with weight loss | Resistant to weight loss; follows cancer course | | **Frequency** | 90% of AN cases | 5–10% of AN cases | ### Why This Patient Has Benign AN **High-Yield:** Benign acanthosis nigricans is characterized by: 1. **Obesity** (BMI 32) — primary risk factor 2. **Insulin resistance** (HbA1c 6.8% in prediabetic range) 3. **Gradual, stable course** — 6 months without progression 4. **No systemic alarm features** — no weight loss, no malignancy on screening 5. **Female gender with regular menses** — excludes PCOS (which would show menstrual irregularity) **Clinical Pearl:** Benign AN is strongly associated with the **metabolic syndrome pentad**: central obesity, hypertension, dyslipidemia, hyperglycemia, and hyperinsulinemia. This patient's obesity and prediabetes fit this pattern. ### Management Approach **Mnemonic: WEIGHT** — Weight loss, Exercise, Antidiabetic agents, Insulin-sensitizing drugs, Glucose control, Treat metabolic syndrome 1. **Lifestyle modification** — weight loss (5–10% reduction improves insulin sensitivity) 2. **Glycemic control** — metformin as first-line agent 3. **Address metabolic syndrome** — lipid management, blood pressure control 4. **Reassurance** — benign AN is not a sign of cancer in this clinical context ### Why Malignancy Screening Is Negative **Warning:** Do not over-investigate benign AN. In the absence of systemic alarm features (weight loss, constitutional symptoms, abnormal imaging), extensive cancer screening is not indicated. This patient's normal pelvic ultrasound and mammography are reassuring. ### Differential Exclusion **PCOS:** Would present with menstrual irregularity, elevated androgens, and polycystic ovaries on ultrasound—this patient has regular menses and normal pelvic imaging. **Hypothyroidism:** Causes weight gain but NOT acanthosis nigricans; TSH would be elevated. 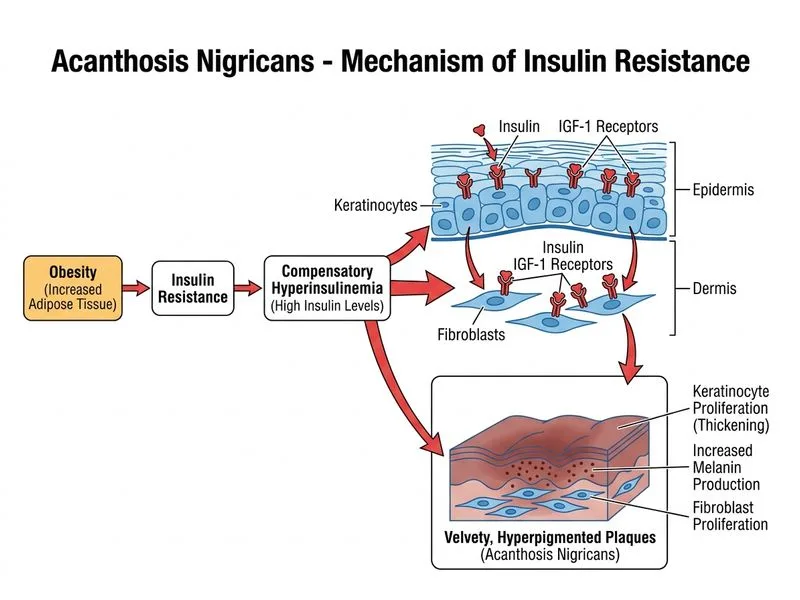
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.