## Pathophysiology of Acanthosis Nigricans in Insulin Resistance **Key Point:** Acanthosis nigricans is a cutaneous manifestation of insulin resistance, not diabetes per se. The hyperinsulinemia drives the skin changes through paracrine signaling. ### Mechanism The pathophysiology involves: 1. **Hyperinsulinemia** → elevated circulating insulin levels (often 2–3× normal) 2. **IGF-1 receptor activation** → insulin cross-reacts with IGF-1 receptors on keratinocytes, fibroblasts, and dermal papillae 3. **Downstream effects:** - Increased keratinocyte proliferation (acanthosis = epidermal thickening) - Enhanced melanin synthesis and transfer to basal keratinocytes (hyperpigmentation) - Increased dermal glycosaminoglycan deposition (velvety texture) **High-Yield:** Acanthosis nigricans is a **marker of insulin resistance**, not a marker of diabetes itself. It occurs in: - Type 2 diabetes (most common) - Polycystic ovary syndrome (PCOS) - Obesity - Acromegaly - Cushing syndrome - Rarely, internal malignancy (paraneoplastic form, usually associated with gastric or lung cancer) ### Clinical Pearl The presence of acanthosis nigricans in a patient with type 2 diabetes indicates **severe insulin resistance** and is associated with increased cardiovascular risk. It often precedes overt diabetes by months to years. **Mnemonic: "ACANTHOSIS = ACTivation of IGF-1 receptors by hyperINsulinemia"** ### Why This Patient? This patient has: - Elevated fasting glucose (186 mg/dL) and HbA1c (9.2%) → poorly controlled type 2 diabetes - Elevated fasting insulin (28 mIU/L, normal < 12) → **hyperinsulinemia** (the key driver) - Normal abdominal ultrasound → rules out internal malignancy as the cause - Typical distribution (neck, axillae, inframammary) → classic for metabolic acanthosis nigricans The insulin level is the critical clue: hyperinsulinemia, not hyperglycemia alone, causes acanthosis nigricans. 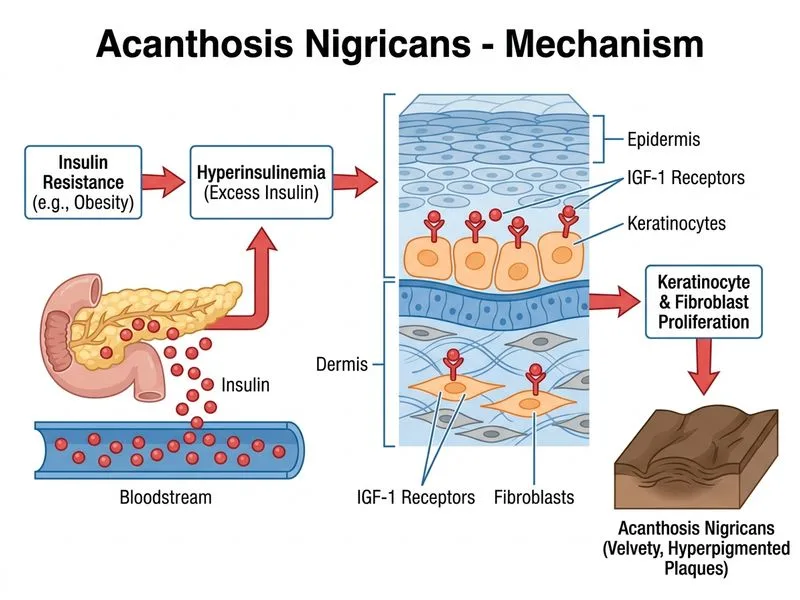
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.