## Clinical Diagnosis This patient has **acute bacterial sinusitis** (maxillary) with classic features: purulent nasal discharge, facial pain, recent URTI, and CT evidence of sinus opacification with air-fluid levels. ## Management Approach for Acute Sinusitis **Key Point:** Acute sinusitis is self-limited in most cases (80–90%) and resolves with conservative management within 2–4 weeks. ### First-Line Management 1. **Nasal saline irrigation** — mechanical clearance of secretions and biofilm 2. **Topical nasal decongestants** (xylometazoline, oxymetazoline) — reduce mucosal edema and improve drainage 3. **Oral antibiotics** — indicated when symptoms persist >7 days or are severe - First-line: Amoxicillin-clavulanate or cephalosporin - Duration: 10–14 days (some guidelines suggest 7 days) 4. **Topical nasal steroids** (mometasone, fluticasone) — reduce inflammation 5. **Analgesics** — for pain relief 6. **Clinical review at 2 weeks** — assess response; if no improvement, consider imaging or specialist referral **High-Yield:** The majority of acute sinusitis cases resolve without surgery. Surgery is reserved for complications (orbital cellulitis, intracranial extension) or chronic disease unresponsive to medical therapy. ## Why Surgery Is NOT Indicated Here - No systemic toxicity or fever - No orbital or intracranial signs - First presentation of acute sinusitis - No immunocompromise - Uncomplicated maxillary involvement **Clinical Pearl:** FESS is indicated in acute sinusitis only when there is acute ethmoid or sphenoid sinusitis with orbital/intracranial complications, or when the patient is critically ill and requires urgent drainage. ## Why Other Options Are Wrong - **Immediate FESS:** Premature; acute sinusitis is self-limited and responds to medical therapy in >80% of cases. - **Long-term corticosteroids:** Not standard for acute sinusitis; topical steroids are sufficient. - **Repeat CT in 2 weeks:** Unnecessary; clinical assessment is the guide. Imaging is reserved for recurrent or chronic disease or suspected complications. [cite:Scott-Brown's Otorhinolaryngology Ch 4, Harrison 21e Ch 146] 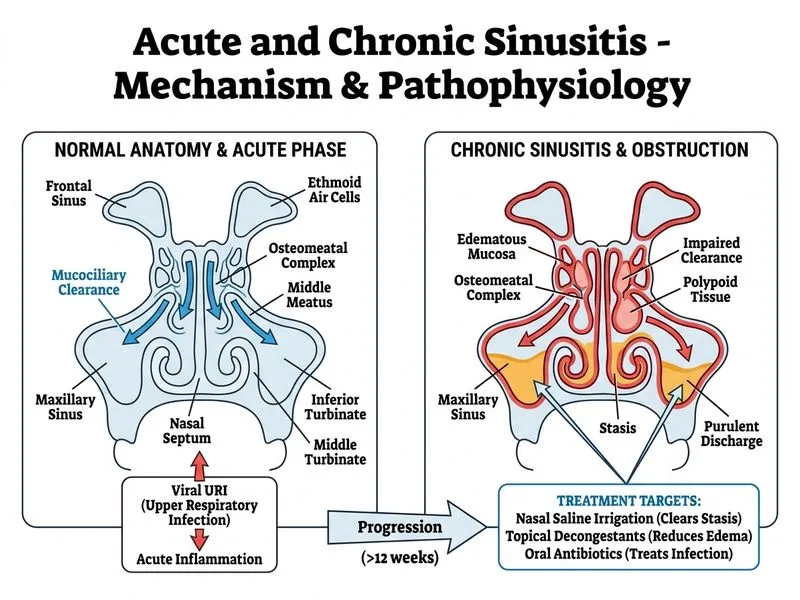
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.