## Distinguishing Acute Bacterial from Viral Sinusitis ### Clinical Presentation Comparison | Feature | Acute Viral Rhinosinusitis | Acute Bacterial Sinusitis | |---------|---------------------------|---------------------------| | **Onset** | Sudden, peaks day 3–5 | Often follows viral prodrome | | **Nasal discharge** | Clear to mucopurulent, improves by day 7–10 | Purulent, persists or worsens after day 10 | | **Symptom trajectory** | Improves after 5–7 days | Worsens after initial improvement (biphasic) | | **Fever pattern** | Low-grade, early (day 1–3) | May be absent or high-grade, later onset | | **Facial pain** | Mild pressure, resolves with viral illness | Severe, localized, persistent | | **Duration** | Self-limited, <10 days | >10 days without improvement | **Key Point:** The **biphasic pattern** — initial improvement followed by worsening with purulent discharge after day 10 — is the hallmark of bacterial superinfection and distinguishes it from uncomplicated viral rhinosinusitis. ### Pathophysiology 1. Viral infection damages mucociliary clearance and epithelium 2. Secondary bacterial colonization (commonly *Streptococcus pneumoniae*, *Haemophilus influenzae*, *Moraxella catarrhalis*) 3. Purulent exudate accumulates → persistent or worsening symptoms **Clinical Pearl:** A patient who "gets worse after getting better" within the first 2 weeks of URI is the classic presentation of acute bacterial sinusitis and warrants imaging and antibiotic therapy. **High-Yield:** The **10-day rule** is critical for NEET PG: symptoms persisting or worsening beyond 10 days of onset strongly suggest bacterial sinusitis and warrant CT imaging and/or empiric antibiotics. 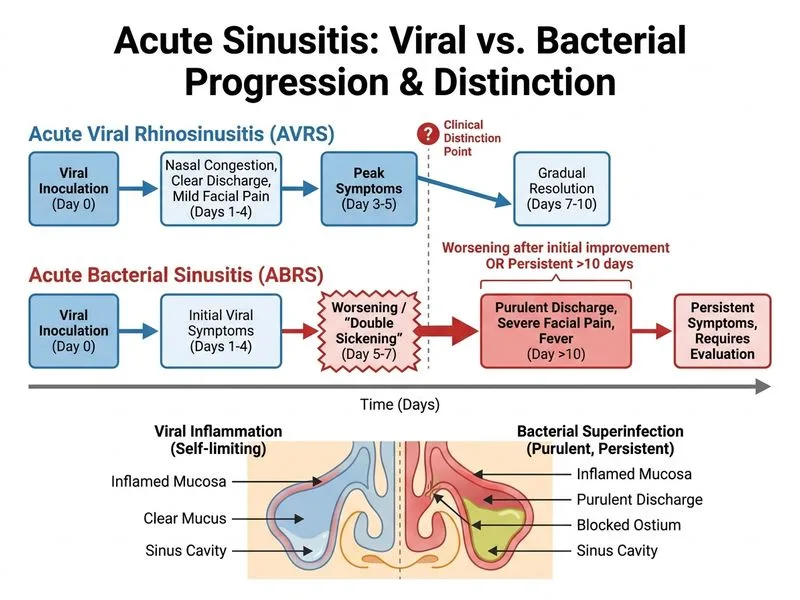
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.