## Perforated vs. Non-Perforated Acute Appendicitis ### Clinical and Pathophysiological Distinction | Feature | Non-Perforated Appendicitis | Perforated Appendicitis | |---------|-------------------------------|------------------------| | **Peritoneal signs** | Localized to RLQ | Diffuse (generalized peritonitis) | | **Bowel sounds** | Normal or slightly decreased | Absent or markedly diminished | | **Abdominal distension** | Minimal | Marked (ileus) | | **Fever** | 38–39°C | Often >39°C, septic | | **WBC** | 11,000–15,000 | >15,000, often >20,000 | | **Peritoneal fluid** | Minimal/localized | Purulent, feculent | | **Imaging (CT/ultrasound)** | Thickened appendix, localized inflammation | Free air, abscess, diffuse peritoneal fluid | | **Clinical course** | Responds to antibiotics + surgery | Septic shock risk, requires urgent surgery | ### Key Point: **The hallmark discriminator is the *pattern of peritoneal signs*: localized RLQ signs in non-perforated disease versus *diffuse peritonitis* with absent bowel sounds and abdominal distension in perforated appendicitis.** **High-Yield:** Perforated appendicitis presents as an *acute surgical abdomen* with: - Diffuse rebound and guarding (not focal to RLQ) - Absent or severely diminished bowel sounds (paralytic ileus) - Abdominal distension (third-spacing, ileus) - Systemic toxicity (high fever, tachycardia, hypotension) **Clinical Pearl:** The transition from localized to diffuse peritonitis often occurs 24–48 hours after perforation. Early recognition is critical: a patient with appendicitis who develops *sudden worsening* of pain with diffuse peritoneal signs and ileus has likely perforated. **Mnemonic: PERFORATION SIGNS** — **P**urulent fluid, **E**xtended (diffuse) peritonitis, **R**educed bowel sounds, **F**ever (high), **O**bstruction (ileus), **R**igidity (generalized), **A**bscess (on imaging), **T**oxicity (septic), **I**nflammatory markers (very high), **O**peration (urgent), **N**eed for resuscitation. **Warning:** ~~Fever and elevated WBC alone~~ do not distinguish perforation from non-perforation; both conditions present with these findings. The key is the *distribution* of peritoneal signs and the presence of *ileus*. 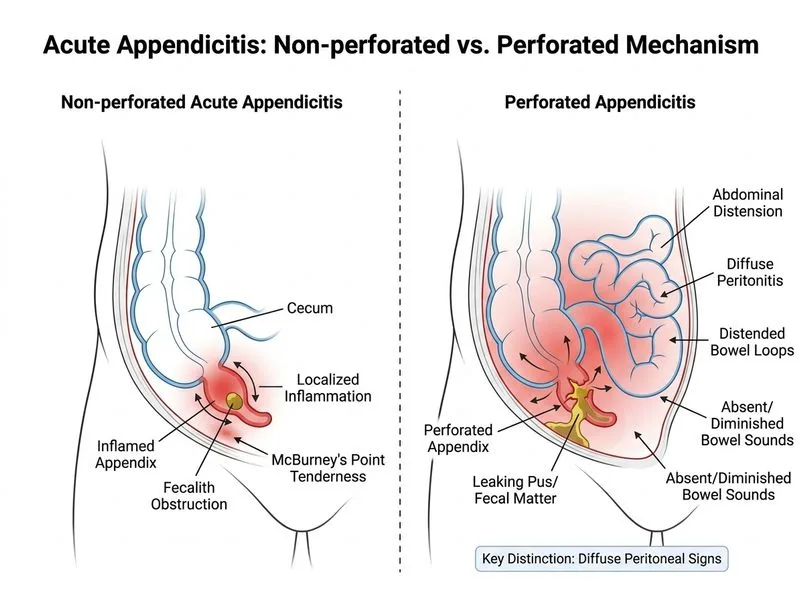
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.