## Diagnosis and Clinical Reasoning **Key Point:** This patient has acute appendicitis with classic clinical presentation and imaging confirmation. The combination of clinical signs (McBurney's point tenderness, rebound, guarding, Rovsing's sign positive) and imaging findings (dilated, non-compressible appendix >6 mm on ultrasound) establishes the diagnosis. ## Why Immediate Appendectomy is Correct **High-Yield:** In acute appendicitis with clear clinical and radiological diagnosis, immediate appendectomy is the gold standard. Delay increases risk of perforation, peritonitis, and sepsis. **Clinical Pearl:** McBurney's point (located 1/3 distance from anterior superior iliac spine to umbilicus) tenderness is the most specific clinical sign for appendicitis. Rovsing's sign (pain in RLQ on palpation of LLQ) indicates peritoneal irritation and supports the diagnosis. ## Imaging Confirmation Ultrasound findings diagnostic of appendicitis: - Appendiceal diameter >6 mm (this patient: 8 mm) - Non-compressibility - Echogenic periappendiceal fat - Free fluid in pelvis No further imaging is needed when clinical and ultrasound findings are concordant. ## Timeline Consideration **Mnemonic:** **APPENDIX** — Acute Perforation Prompt Endoscopy/Early Diagnosis Needs Immediate eXcision - <24 hours: low perforation risk (~5%) - 24–48 hours: moderate risk (~25%) - >48 hours: high risk (>30%) This patient is at 24 hours; further delay increases morbidity. 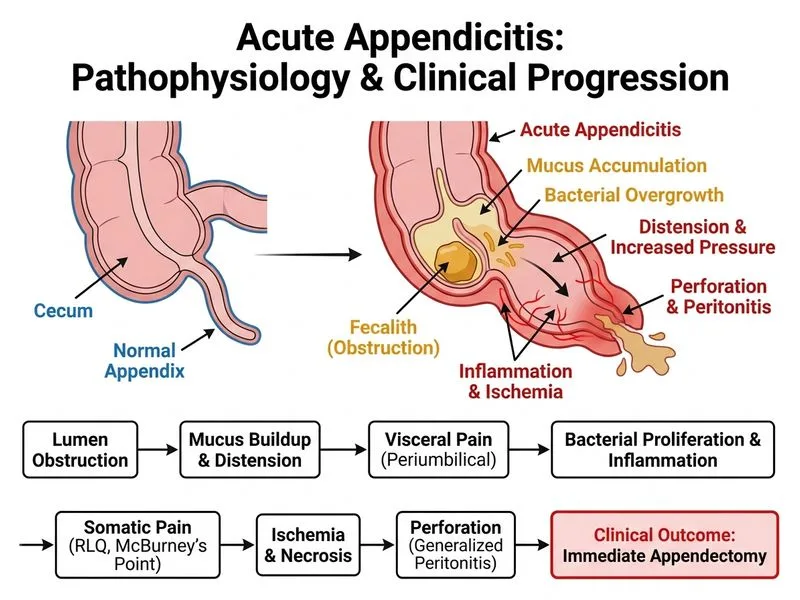
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.