## Distinguishing Perforated from Non-Perforated Acute Appendicitis ### Clinical Scenario Both perforated and non-perforated appendicitis present with fever, leukocytosis, and peritoneal signs. However, **radiological evidence of perforation** is the gold standard discriminator. ### Key Differentiating Feature **Key Point:** Free air (pneumoperitoneum) on imaging—erect chest X-ray or CT abdomen—is pathognomonic for perforation. This finding indicates breach of the appendiceal wall and spillage of luminal contents into the peritoneal cavity, fundamentally altering the clinical course and management urgency. ### Comparison Table | Feature | Non-Perforated Appendicitis | Perforated Appendicitis | | --- | --- | --- | | **Free air on imaging** | Absent | Present (pneumoperitoneum) | | **Fever & tachycardia** | Present in both | Present, often more severe | | **Peritoneal signs** | Present in both | Present, diffuse | | **Inflammatory markers** | Elevated in both | More markedly elevated | | **Clinical course** | Responds to early surgery | Rapid deterioration; sepsis risk | | **Imaging modality** | Ultrasound or CT | CT or erect CXR (free air) | ### Radiological Findings **High-Yield:** - **Erect chest X-ray:** Free air appears as a **lucent crescent** under the diaphragm (best seen on left side). Sensitivity ~70% for perforation. - **CT abdomen/pelvis:** Free air is seen as lucency in the peritoneal cavity; **most sensitive (>95%)** and specific. Also shows appendiceal wall discontinuity, abscess formation, and degree of inflammation. - **Ultrasound:** May show appendiceal perforation (loss of wall layers, echogenic debris in pelvis) but less reliable than CT. ### Clinical Pearl **Clinical Pearl:** A patient with 5 days of symptoms (as in this stem) is at high risk for perforation. The **duration of symptoms >48 hours** correlates with increased perforation risk. Imaging confirmation of free air mandates urgent surgical intervention and aggressive resuscitation (IV fluids, broad-spectrum antibiotics, vasopressor support if needed). ### Mnemonic **Mnemonic:** **PERFORATION SIGNS** = **P**neumoperitoneum on imaging, **E**vidence of wall breach on CT, **R**apid clinical deterioration, **F**ree air on erect CXR, **O**bstetric/surgical emergency, **R**esuscitation + urgent surgery required, **A**bscess/loculated fluid, **T**oxemia/sepsis, **I**nflammatory markers markedly elevated, **O**pen appendectomy (not laparoscopic initially), **N**eed for ICU monitoring. ### Why Other Options Are Misleading - **Fever & tachycardia:** Present in both non-perforated and perforated appendicitis; not discriminatory. - **Inflammatory markers:** Both conditions show elevated CRP and procalcitonin; perforated appendicitis shows *higher* levels, but there is significant overlap, making this non-specific. - **Peritoneal signs:** Both present with rebound and guarding; perforation may show *more diffuse* peritonitis, but this is a matter of degree, not a reliable discriminator. 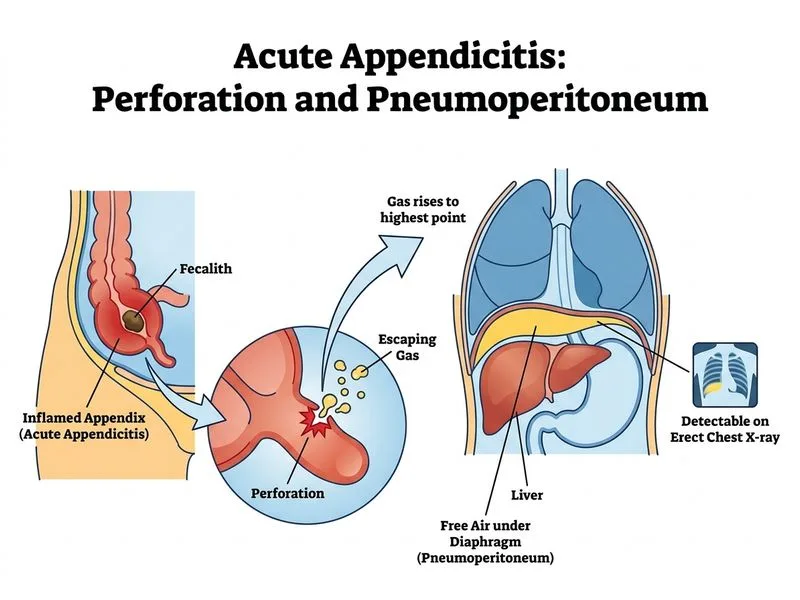
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.