## Distinguishing Acute Thrombotic from Acute Embolic Limb Ischemia ### Clinical Differentiation **Key Point:** The **history of claudication and presence of contralateral pulses** is the best clinical (bedside) discriminator between acute thrombotic and acute embolic arterial occlusion. | Feature | Acute Embolism | Acute Thrombosis | |---------|----------------|------------------| | **Onset** | Sudden (minutes to hours) | Gradual (hours to days) | | **Prior claudication** | Absent | Often present | | **Contralateral pulses** | Normal (healthy vasculature) | Often abnormal (bilateral atherosclerosis) | | **Collateral circulation** | Absent (healthy artery) | Present (chronic disease) | | **Source** | Cardiac (AF, MI, valve) | Atherosclerotic plaque | | **Limb viability** | Often compromised early | May be better preserved | ### Why Option A is the Best Clinical Discriminator **Acute thrombotic occlusion** develops on a background of chronic atherosclerotic disease. The patient typically has: 1. A **prior history of claudication** in the same limb (chronic arterial insufficiency before the acute event). 2. **Abnormal or absent contralateral pulses** because atherosclerosis is a systemic, bilateral disease. **Acute embolic occlusion** (as in this patient with atrial fibrillation) occurs in a previously healthy artery: 1. **No prior claudication** — the limb was well-perfused before the embolic event. 2. **Normal contralateral pulses** — the contralateral vasculature is unaffected. These two features (claudication history + contralateral pulse status) are directly assessable at the bedside without imaging, making Option A the **best clinical discriminator**. ### Why Option C is Less Precise Option C states "presence of collateral circulation and gradual onset." While both features do favor thrombosis, **collateral circulation** is an imaging/angiographic finding, not a direct clinical feature. The stem asks for a **clinical feature** that best distinguishes the two entities. Furthermore, Option C conflates two separate findings, reducing its precision as a single discriminating feature. Option A captures the same pathophysiologic logic (chronic atherosclerotic disease) through purely clinical, bedside-assessable findings. **High-Yield:** In a patient with acute limb ischemia, check the contralateral limb pulses immediately — absent or diminished contralateral pulses strongly favor thrombosis over embolism. **Clinical Pearl:** A patient with AF presenting with acute limb ischemia and *no* prior claudication and *normal* contralateral pulses almost certainly has an embolism. Conversely, a patient with prior claudication and absent contralateral pulses almost certainly has acute-on-chronic thrombosis. ### Management Implications - **Embolic occlusion**: Urgent embolectomy (Fogarty catheter) within 6–8 hours. - **Thrombotic occlusion**: Thrombolysis or bypass surgery; collaterals may preserve viability longer. **Mnemonic:** **THROMBOSIS = bilateral disease (abnormal contralateral pulses) + prior claudication; EMBOLISM = unilateral sudden event (normal contralateral pulses) + no prior symptoms** *[Reference: Sabiston Textbook of Surgery, Ch 65; Rutherford's Vascular Surgery, 9th ed.]* 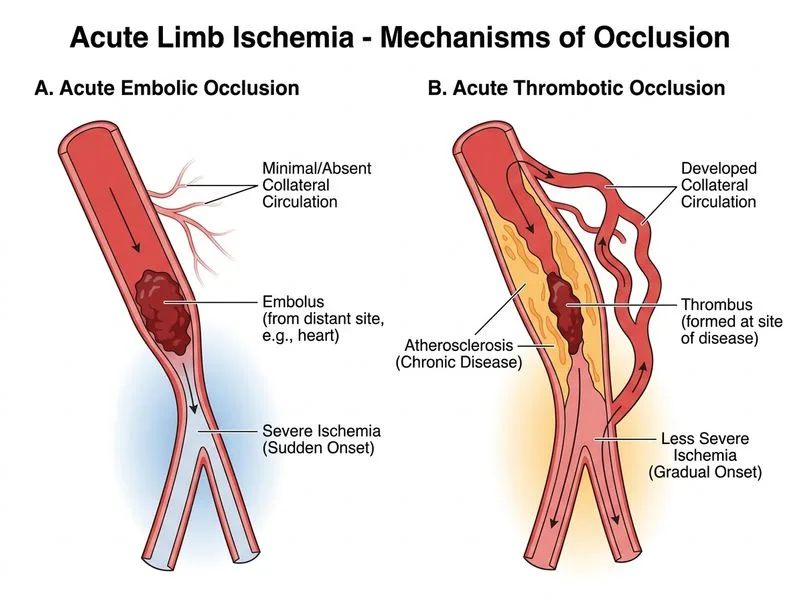
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.