## Clinical Assessment **Key Point:** This patient has **subacute/chronic limb ischemia** (3-day history) with **Rutherford Grade I–IIa** (viable limb: intact sensory and motor function). The occlusion is thrombotic (atherosclerotic SFA disease), not embolic. ## Differentiation: Acute vs Subacute/Chronic Ischemia | Feature | Acute Embolic | Acute Thrombotic | Subacute/Chronic | |---------|---------------|------------------|------------------| | Onset | Minutes–hours | Hours–days | Days–weeks | | Source | AF, cardiac | Atherosclerosis | Atherosclerosis | | Collaterals | Absent | Developing | Well-developed | | Viability | Threatened quickly | Threatened | Often viable | | Treatment | Embolectomy | Thrombolysis/PTA/Surgery | Thrombolysis/PTA/Surgery | **High-Yield:** In **subacute/chronic ischemia with viable limb**, catheter-directed thrombolysis (CDT) or percutaneous transluminal angioplasty (PTA) is preferred over emergency surgery because: - Collaterals are established → limb is not immediately threatened - Thrombolysis/PTA restores native anatomy and improves long-term patency - Surgery (thrombectomy/bypass) is reserved for thrombolysis failure or contraindication ## Management Algorithm for Subacute/Chronic Ischemia ```mermaid flowchart TD A[Subacute/Chronic Limb Ischemia]:::outcome --> B{Viable limb?}:::decision B -->|Yes| C[Heparin + Antiplatelet]:::action B -->|No| D[Amputation]:::urgent C --> E{Thrombolysis candidate?}:::decision E -->|Yes| F[CDT or PTA]:::action E -->|No| G[Surgical revascularization]:::action F --> H{Success?}:::decision H -->|Yes| I[Discharge with anticoagulation]:::outcome H -->|No| J[Surgical salvage]:::action ``` **Clinical Pearl:** Palpable popliteal pulse + intact motor/sensory = collateral circulation is adequate. The limb is **not immediately threatened**, so there is time for diagnostic angiography and endovascular intervention. **Mnemonic:** **CDT vs Surgery in Subacute Ischemia** — **C**atheter-**D**irected **T**hrombolysis is first-line if: - **C**ollaterals present (viable limb) - **D**uration < 14 days (thrombus still lytic) - **T**hrombus (not chronic occlusion) ## Why Heparin + Thrombolysis/PTA? 1. **Heparin:** Prevents thrombus propagation and improves collateral flow immediately. 2. **CDT:** Dissolves thrombus, restores native vessel, better long-term outcomes than surgery. 3. **PTA:** If stenosis is the primary lesion, restores flow directly. 4. **Time window:** 3 days is within the 14-day window for effective thrombolysis. [cite:Sabiston Textbook of Surgery Ch 64; Rutherford Vascular Surgery 9e] 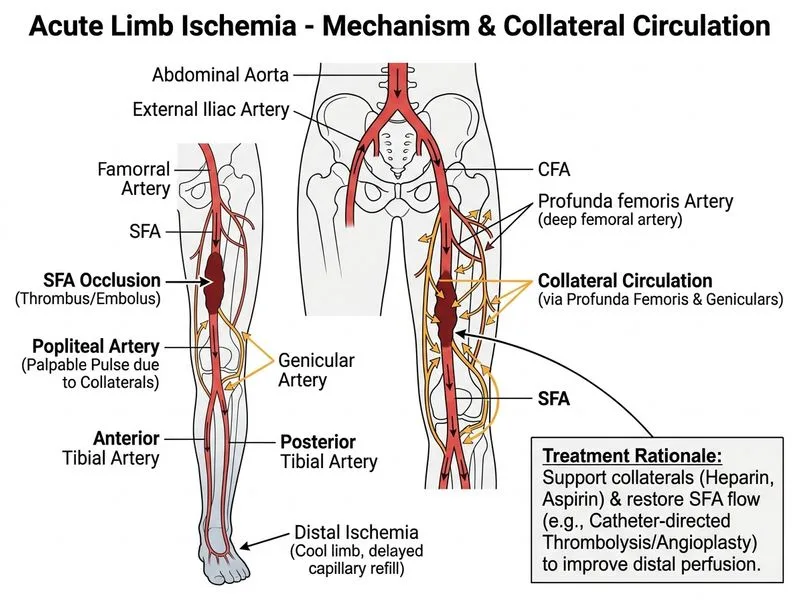
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.