## Acute Limb Ischemia: Thrombotic vs Embolic ### Clinical Presentation Analysis This patient presents with **acute-on-chronic limb ischemia**—a key distinguishing feature: | Feature | This Case | Embolic ALI | Thrombotic ALI | |---------|-----------|-------------|----------------| | **Prior claudication** | Yes (2 years) | No (sudden, no prior symptoms) | Yes (progressive) | | **Artery affected** | Popliteal (atherosclerotic prone) | Any (often femoral) | Distal vessels | | **Embolic source** | None on imaging | Cardiac (AF, MI, valve) | N/A | | **Collateral circulation** | Developed over years | Absent | Present | | **Mechanism** | Thrombosis on plaque | Embolus lodges | Thrombosis on disease | ### Key Point: **Acute thrombosis on a chronically diseased artery is the most common cause of acute limb ischemia in patients with pre-existing peripheral arterial disease.** The 2-year history of claudication indicates established atherosclerotic disease; acute thrombosis occurs when a plaque ruptures or flow becomes critically reduced. ### Pathophysiology of Thrombotic ALI ```mermaid flowchart TD A[Chronic PAD with atherosclerotic plaque]:::outcome --> B[Plaque rupture or ulceration]:::action B --> C[Exposure of thrombogenic core]:::action C --> D[Platelet aggregation + fibrin deposition]:::action D --> E[Acute thrombotic occlusion]:::outcome E --> F{Collateral circulation adequate?}:::decision F -->|Yes| G[Threatened limb]:::outcome F -->|No| H[Viable limb with tissue loss risk]:::outcome ``` ### Why NOT Embolic? **High-Yield:** Embolic ALI typically presents in patients **without prior claudication** because: - Emboli lodge in normal arteries with no collateral development - Sudden onset in a previously asymptomatic limb - Cardiac source (AF, MI, valve disease) is identifiable This patient has **2 years of claudication** → established collateral circulation → thrombotic mechanism. ### Clinical Pearl: **Collateral circulation is the key discriminator.** Patients with chronic PAD develop collaterals over time. When acute thrombosis occurs on this diseased substrate, collaterals partially compensate, resulting in the "threatened" stage rather than immediate gangrene. Embolic ALI, by contrast, occludes normal vessels with no collaterals, causing rapid tissue loss. ### Management Implications Thrombotic ALI (unlike embolic) may be managed with: 1. **Heparin + thrombolysis** (catheter-directed) — effective for thrombi 2. **Surgical thrombectomy** — if thrombolysis contraindicated or fails 3. **Bypass grafting** — if underlying stenosis is severe ### Warning: ~~Embolic ALI~~ — no cardiac source identified; prior claudication excludes embolic mechanism. ~~Dissection~~ — no history of trauma or connective tissue disease; popliteal dissection is rare and usually spontaneous in young patients. 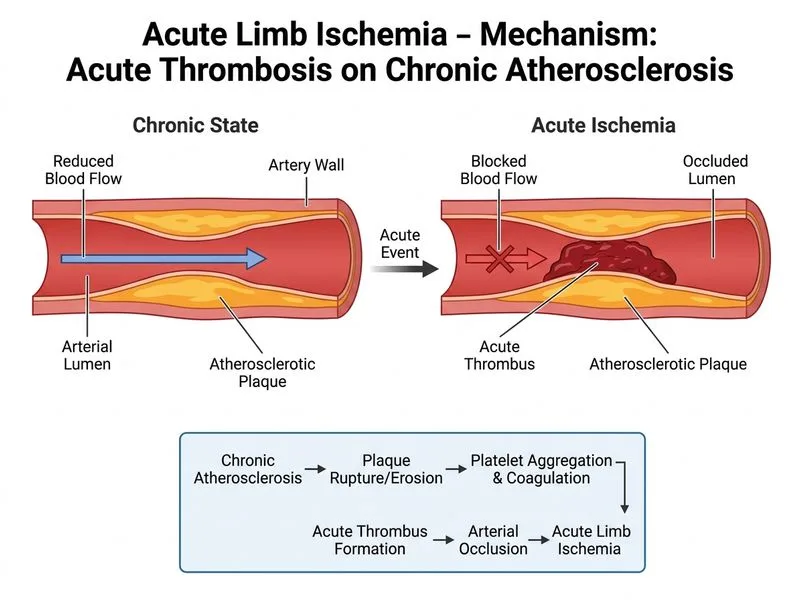
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.