## Acute Limb Ischemia: Thrombotic vs. Embolic—Treatment Selection ### Clinical Context: Thrombosis vs. Embolism **Key Point:** This patient has **acute thrombosis** (not embolism) of the SFA in the setting of chronic PAD. This is fundamentally different from the previous case and changes the management strategy. | Feature | Embolism | Thrombosis | |---------|----------|------------| | Onset | Sudden (minutes) | Gradual (hours–days) | | Collateral circulation | Poor | Often well-developed | | Underlying vessel | Normal | Atherosclerotic | | Preferred treatment | Surgical embolectomy | Thrombolysis or PTA | | Reason | Speed; poor collaterals | Dissolves thrombus; preserves vessel; collaterals provide time | ### Why CDT is Preferred in This Case **High-Yield:** In acute thrombosis with viable tissue, catheter-directed thrombolysis offers: 1. **Dissolution of thrombus** rather than mechanical removal 2. **Identification of underlying stenosis** (allows PTA/stent placement) 3. **Preservation of collateral circulation** (important in chronic PAD) 4. **Lower morbidity** than thrombectomy in patients with comorbidities 5. **Time window**: Chronic PAD patients have better collaterals; thrombolysis can be attempted even at 3 days if tissue is still viable **Clinical Pearl:** The **absence of motor weakness** is the critical finding here. Motor paralysis indicates irreversible ischemia; sensory loss alone (especially in chronic PAD) suggests viable tissue that can tolerate the 2–4 hour thrombolysis window. ### Decision Algorithm for Acute Limb Ischemia ```mermaid flowchart TD A[Acute Limb Ischemia]:::outcome --> B{Etiology?}:::decision B -->|Embolism<br/>Sudden onset| C{Viable?}:::decision B -->|Thrombosis<br/>Gradual onset| D{Viable?}:::decision C -->|Yes| E[Surgical embolectomy<br/>ASAP]:::action C -->|No| F[Amputation]:::urgent D -->|Yes: No paralysis| G[Catheter-directed<br/>thrombolysis]:::action D -->|No: Paralysis| H[Consider embolectomy<br/>or amputation]:::urgent G --> I[Identify stenosis<br/>PTA/stent if needed]:::action E --> J[Restore flow<br/>Monitor reperfusion]:::action ``` ### Rutherford Category Assessment **This patient is Category IIa–IIb:** - Sensory loss: present (mild–moderate) - Motor weakness: **absent** ← This is the key finding - Foot perfusion: preserved enough to attempt thrombolysis **Key Point:** Absence of paralysis = tissue is still viable and can tolerate the thrombolysis window (2–4 hours, sometimes up to 14 days in chronic PAD with good collaterals). ### Why the Other Options Are Wrong **Mottled skin + sensory loss alone** does NOT indicate irreversibility if **motor function is preserved**. Mottling in chronic PAD is often reversible with reperfusion. **Age and comorbidities** are relative contraindications to surgery, but they do not change the fundamental treatment algorithm. CDT is chosen because of the **thrombotic etiology and viable tissue**, not age. **3-day duration** is actually an advantage for thrombolysis in thrombotic occlusion (collaterals have had time to develop and maintain viability). In embolism, this would be too late. [cite:Sabiston Textbook of Surgery 21e Ch 64; Rutherford's Vascular Surgery 8e Ch 134] 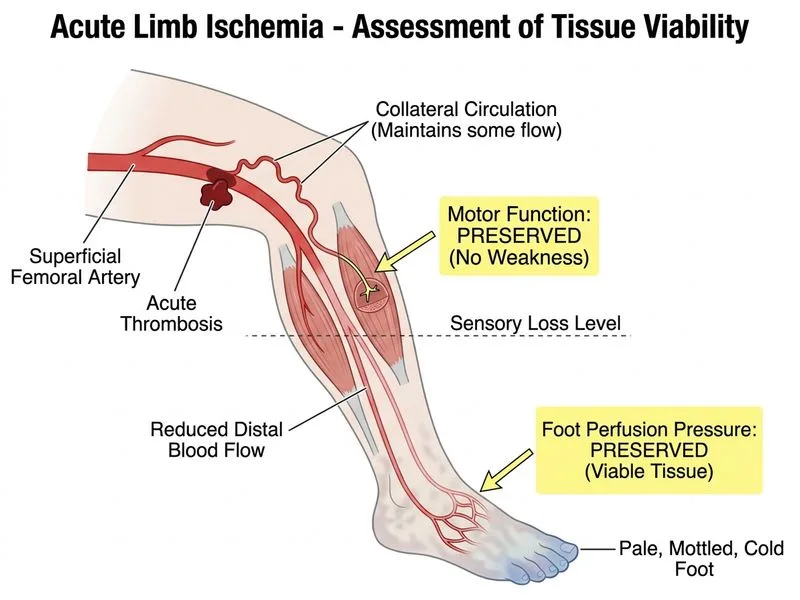
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.