## Clinical Diagnosis: Acute Thrombosis on Chronic Atherosclerotic Disease This patient presents with **acute limb ischemia (ALI) secondary to in-situ thrombosis** of atherosclerotic arteries, not embolism. ## Key Distinguishing Features | Feature | Acute Embolism | Acute Thrombosis (This Case) | |---------|----------------|------------------------------| | **Onset** | Sudden (minutes to hours) | Gradual (hours to days) | | **Prodrome** | None; previously asymptomatic limb | Claudication or rest pain history | | **Vessel pattern** | Single large artery (e.g., femoral) | Multiple small/medium arteries | | **Proximal pulses** | Normal/palpable | Weak or diminished | | **Cause** | Cardiac (AF, MI, valve disease) | Atherosclerosis, diabetes, smoking | | **Imaging** | Patent proximal vessels, single occlusion | Stenosis/occlusion of multiple vessels | **This patient's findings:** - **Gradual onset over 36 hours** (not sudden) - **Multiple vessel involvement** (anterior tibial, peroneal, posterior tibial stenosis) - **Weak but palpable proximal pulses** (not normal) - **Risk factors for atherosclerosis** (diabetes, hypertension, age 55) - **No cardiac history** (no AF, recent MI, or valvular disease mentioned) ## Pathophysiology of Acute Thrombosis on Chronic Atherosclerosis ```mermaid flowchart TD A[Chronic atherosclerotic disease]:::outcome --> B[Arterial stenosis develops over years]:::outcome B --> C{Triggering event}:::decision C -->|Plaque rupture| D[Exposure of thrombogenic core]:::action C -->|Endothelial erosion| E[Platelet aggregation]:::action D --> F[Thrombus formation at stenotic site]:::action E --> F F --> G[Acute reduction in distal perfusion]:::outcome G --> H[Limb ischemia develops over hours]:::outcome H --> I{Collateral circulation adequate?}:::decision I -->|Yes| J[Marginal ischemia - Rutherford I-IIa]:::outcome I -->|No| K[Severe ischemia - Rutherford IIb-III]:::urgent ``` ## Why This Is Thrombosis, Not Embolism **High-Yield:** 1. **Gradual onset (36 hours):** Embolism is sudden; thrombosis develops over hours to days as collaterals become exhausted. 2. **Multiple vessel involvement:** Thrombosis affects the diseased vessel and its branches; embolism typically lodges at a single bifurcation (femoral, popliteal). 3. **Weak proximal pulses:** Suggests chronic atherosclerotic disease affecting the entire arterial tree; normal proximal pulses favor embolism. 4. **Diabetes and hypertension:** Major risk factors for atherosclerotic thrombosis, not embolism. **Key Point:** - **Embolism = sudden, single large artery, normal proximal pulses, cardiac source.** - **Thrombosis = gradual, multiple small arteries, weak proximal pulses, atherosclerotic risk factors.** ## Clinical Pearl In diabetic patients, **acute-on-chronic ischemia** is common because diabetes accelerates atherosclerosis and creates a milieu of endothelial dysfunction, hypercoagulability, and impaired collateral formation. The gradual onset here reflects the patient's chronic stenotic disease suddenly decompensating due to thrombosis. ## Rutherford Classification (This Patient) Based on **cyanosis, mottling, blistering, and intact motor function**, this patient is **Rutherford IIb (immediately threatened)**—sensory loss is present (pain is a sign of ischemic neuropathy), and tissue damage is imminent. ## Management Implications **Acute thrombosis on atherosclerotic disease** may be managed by: 1. **IV heparin** (anticoagulation) 2. **Thrombolysis** (catheter-directed, if no contraindications and limb is viable) 3. **Surgical thrombectomy** (if thrombolysis fails or contraindicated) 4. **Percutaneous angioplasty ± stenting** (after acute phase, for underlying stenosis) This differs from **pure embolism**, which typically requires **immediate embolectomy** without time for imaging or thrombolysis. 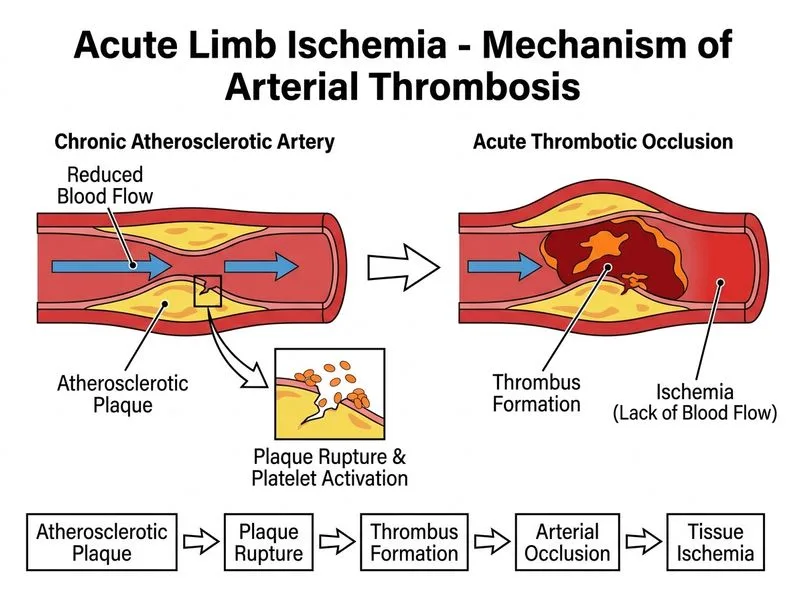
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.