## Identifying the Cause of Primary Addison Disease ### Clinical Context The patient has confirmed primary adrenal insufficiency: - Low cortisol (8 μg/dL) - Markedly elevated ACTH (156 pg/mL) — loss of negative feedback **Key Point:** Once primary adrenal insufficiency is confirmed, the next step is to determine the underlying etiology, as management and prognosis differ significantly. ### Major Causes of Primary Addison Disease | Cause | Frequency | Geographic Variation | Key Diagnostic Test | |-------|-----------|----------------------|---------------------| | **Autoimmune** | 80–90% (developed countries) | Common in North America, Europe | 21-OH antibodies, adrenal peroxidase antibodies | | **Tuberculosis** | 10–20% (developed); 70–90% (endemic regions) | High in India, Africa, Southeast Asia | TB serology, chest X-ray, TB culture, CT adrenal imaging | | **Fungal infection** | <5% | Histoplasmosis (USA), coccidioidomycosis | Fungal serology, imaging | | **Adrenal hemorrhage** | <5% | Post-trauma, anticoagulation, sepsis | CT/MRI imaging | | **Metastatic malignancy** | <5% | Lung, breast, lymphoma | CT imaging, imaging of primary | ### Why Antibody Testing is the Appropriate Next Investigation **High-Yield:** In a patient with confirmed primary adrenal insufficiency in a non-endemic TB region (or with no TB risk factors), autoimmune Addison disease is the most likely diagnosis and should be confirmed first with antibody testing. 1. **Highest pretest probability:** Autoimmune etiology accounts for 80–90% of cases in developed countries 2. **Non-invasive and specific:** 21-hydroxylase (21-OH) antibodies are present in 60–75% of autoimmune Addison disease; adrenal peroxidase (TPO) antibodies in 50–60% 3. **Guides management:** Autoimmune Addison disease has specific associations (polyglandular autoimmune syndrome types 1 and 2) requiring screening for other autoimmune endocrinopathies (thyroid disease, type 1 diabetes, hypogonadism) 4. **Prognostic value:** Antibody-positive patients have a chronic, stable course; antibody-negative patients require imaging to exclude other causes **Clinical Pearl:** Approximately 50% of patients with autoimmune Addison disease have other autoimmune endocrine disorders (Schmidt syndrome = Addison + thyroid disease; polyglandular autoimmune syndrome type 2). Confirming autoimmune etiology triggers screening for these associated conditions. ### When to Pursue Other Investigations ```mermaid flowchart TD A[Primary adrenal insufficiency confirmed]:::outcome --> B{Check 21-OH and adrenal peroxidase antibodies}:::action B -->|Positive| C[Autoimmune Addison disease]:::outcome C --> D[Screen for associated autoimmune diseases]:::action B -->|Negative| E{TB risk factors or endemic region?}:::decision E -->|Yes| F[TB serology, chest X-ray, CT abdomen]:::action E -->|No| G[CT abdomen to exclude hemorrhage, malignancy, fungal infection]:::action F --> H[Identify TB or other etiology]:::outcome G --> H ``` **Mnemonic:** **AUTO-FIRST** = AUTOimmune antibodies FIRST in non-endemic areas; TB imaging if risk factors present. 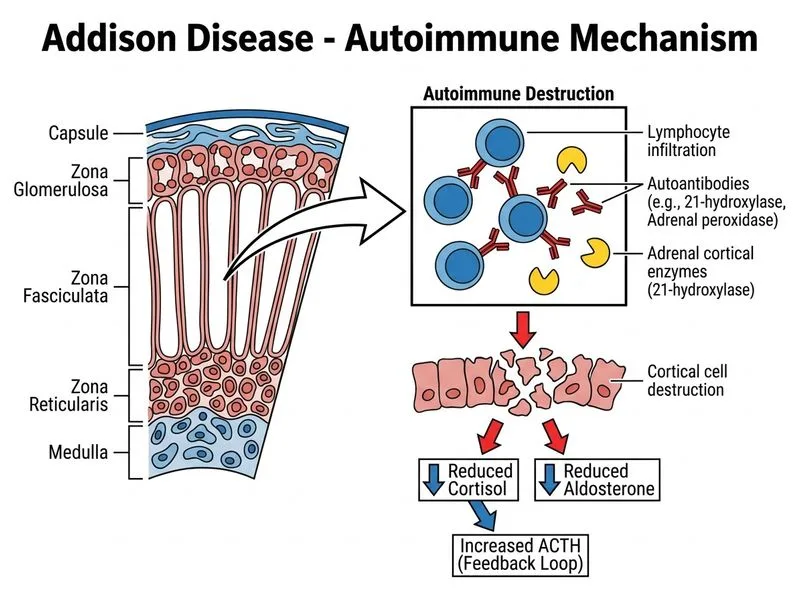
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.