## Histopathological Diagnosis of Alcoholic Cirrhosis ### Clinical Context This patient presents with **decompensated cirrhosis** secondary to chronic alcohol use: - **Compensatory features**: Jaundice, coagulopathy (INR 2.1), hypoalbuminemia (2.8 g/dL), ascites - **Portal hypertension signs**: Spider angiomas, palmar erythema, firm hepatomegaly - **Imaging confirmation**: Cirrhotic echotexture + portal vein dilation (15 mm) ### Histopathological Progression of Alcoholic Liver Disease | Stage | Histology | Timeline | Reversibility | |-------|-----------|----------|----------------| | **Steatosis** | Macrovesicular fat, minimal inflammation | Early (weeks–months) | Fully reversible | | **Alcoholic hepatitis** | Steatosis + acute inflammation, Mallory–Denk bodies, neutrophilic infiltration | Months | Partially reversible | | **Fibrosis** | Perisinusoidal and bridging fibrosis, stellate cell activation | Months–years | Partially reversible | | **Cirrhosis** | Bridging fibrosis, regenerative nodules, architectural distortion, loss of normal lobular pattern | Years–decades | Irreversible | ### Why Option 1 (Bridging Fibrosis with Regenerative Nodules) is Correct **Key Point:** The patient has **established cirrhosis** (not early alcoholic hepatitis), evidenced by: - Clinical decompensation (ascites, coagulopathy, hypoalbuminemia) - Imaging findings (cirrhotic echotexture, portal vein dilation) - Markedly elevated AST >> ALT (characteristic of cirrhosis) At this stage, the liver shows: 1. **Bridging fibrosis** — fibrosis connecting portal tracts and bridging to central veins 2. **Regenerative nodules** — islands of regenerating hepatocytes separated by fibrous septa 3. **Loss of normal architecture** — obliteration of the normal hepatic lobular pattern 4. Possible **Mallory–Denk bodies** (though less prominent in established cirrhosis than in acute alcoholic hepatitis) **High-Yield:** Cirrhosis is defined histologically as **diffuse fibrosis with nodular regeneration and architectural distortion**, not merely the presence of Mallory–Denk bodies or steatosis. ### Why the Other Options Are Wrong **Option 0 (Hepatic steatosis with acute inflammation and Mallory–Denk bodies):** - This describes **acute alcoholic hepatitis**, an earlier stage - Mallory–Denk bodies are prominent in acute hepatitis but less conspicuous in cirrhosis - Acute hepatitis is reversible; this patient has irreversible cirrhosis **Option 2 (Microvesicular steatosis with hepatocyte ballooning and minimal fibrosis):** - Microvesicular steatosis is rare in alcoholic liver disease (more typical of acute fatty liver of pregnancy, drug toxicity) - "Minimal fibrosis" contradicts the imaging and clinical evidence of cirrhosis - This pattern would not produce portal hypertension **Option 3 (Acute hepatitis with portal inflammation and interface hepatitis only):** - Describes **chronic hepatitis** without cirrhosis - Interface hepatitis (inflammation at the portal–parenchymal boundary) is seen in earlier stages - Does not explain the architectural distortion, nodules, or portal hypertension evident in this patient **Clinical Pearl:** The **AST:ALT ratio > 2** in alcoholic liver disease is a hallmark finding and reflects mitochondrial damage; it becomes more pronounced as cirrhosis develops. This patient's AST 280 vs. ALT 95 (ratio ~3) is classic for advanced alcoholic liver disease. **Mnemonic: ABCD of Alcoholic Liver Disease Progression** - **A**cute steatosis (reversible) - **B**ridging fibrosis (partially reversible) - **C**irrhosis (irreversible) - **D**ecompensation (ascites, encephalopathy, bleeding) 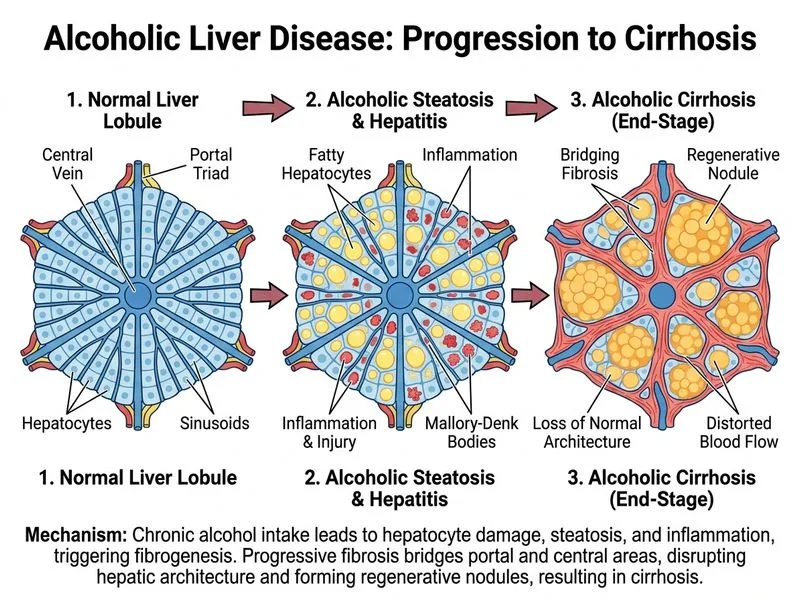
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.