## Acute Alcoholic Hepatitis: Histopathological Hallmarks ### Clinical Presentation This patient presents with **acute alcoholic hepatitis** superimposed on chronic alcoholic liver disease: - **Acute symptoms**: Fever, RUQ pain, jaundice (onset over days) - **Biochemical pattern**: Marked elevation of AST (520) >> ALT (180), AST:ALT ratio ~3 - **Synthetic dysfunction**: Elevated INR (1.8), low albumin (2.9 g/dL) - **Inflammatory response**: Leukocytosis (14,500/μL) - **Exclusion of viral hepatitis**: Negative serology for HAV, HBV, HCV - **Imaging**: Hepatomegaly with coarse echotexture and ascites (suggests underlying cirrhosis) ### Histopathology of Acute Alcoholic Hepatitis **Key Point:** Acute alcoholic hepatitis is characterized by a **triad of findings**: | Finding | Description | Specificity | |---------|-------------|-------------| | **Neutrophilic infiltration** | Polymorphonuclear leukocytes surrounding hepatocytes and in the portal tracts | High — hallmark of acute alcoholic hepatitis | | **Mallory–Denk bodies** | Cytoplasmic inclusions of denatured proteins (ubiquitin, keratin) staining with orcein or trichrome | Specific but not pathognomonic (also seen in Wilson disease, NAFLD, PBC) | | **Hepatocyte ballooning** | Swollen, pale hepatocytes with rarefied cytoplasm due to steatosis and cellular injury | Indicates acute hepatocellular injury | | **Macrovesicular steatosis** | Large lipid droplets displacing the nucleus | Common but not specific | | **Cholestasis** | Bile plugs in canaliculi and hepatocytes | Variable; more prominent in severe cases | ### Why Option 0 is Correct **High-Yield:** The **neutrophilic infiltration around hepatocytes** (also called "satellitosis") is the **most specific histological finding for acute alcoholic hepatitis**. This pattern is: - Characteristic of the acute inflammatory phase - Associated with hepatocyte necrosis and injury - Correlates with clinical severity and prognosis When combined with **Mallory–Denk bodies** and **hepatocyte ballooning**, this triad is diagnostic of acute alcoholic hepatitis. **Clinical Pearl:** The **Maddrey discriminant function** (DF) predicts prognosis in acute alcoholic hepatitis: $$DF = (PT_{patient} - PT_{control}) \times 4.6 + Bilirubin_{(mg/dL)}$$ If DF > 32, mortality is high (~35%), and corticosteroid therapy may be considered. This patient's elevated INR and bilirubin suggest significant disease. ### Why the Other Options Are Wrong **Option 1 (Microvesicular steatosis with mitochondrial inclusions and minimal inflammation):** - Microvesicular steatosis is **rare in alcoholic liver disease**; it is characteristic of acute fatty liver of pregnancy, reye syndrome, and certain drug toxicities (valproate, tetracycline) - Alcoholic liver disease produces **macrovesicular** steatosis, not microvesicular - Minimal inflammation contradicts the acute presentation and leukocytosis **Option 2 (Granulomatous inflammation with caseating necrosis):** - This pattern is seen in **tuberculosis, sarcoidosis, fungal infections, and drug reactions** - Granulomatous hepatitis is not a feature of alcoholic liver disease - Caseating granulomas would suggest tuberculosis or fungal disease, which are excluded by the clinical context **Option 3 (Bile duct proliferation with cholestasis and portal fibrosis):** - Bile duct proliferation is a feature of **cholestasis** (from biliary obstruction, PBC, PSC, or drug-induced liver injury) - While cholestasis can occur in severe alcoholic hepatitis, it is not the **specific** hallmark - Portal fibrosis is a feature of **chronic** alcoholic liver disease, not the acute exacerbation **Mnemonic: MAD Hepatitis (Mallory–Denk bodies, Acute inflammation, Diffuse steatosis)** - **M** — Mallory–Denk bodies (orcein-positive cytoplasmic inclusions) - **A** — Acute neutrophilic infiltration (satellitosis) - **D** — Diffuse macrovesicular steatosis **Warning:** Do not confuse **acute alcoholic hepatitis** (acute inflammatory phase) with **cirrhosis** (chronic fibrotic end-stage). This patient likely has both: acute alcoholic hepatitis superimposed on underlying cirrhosis (evidenced by ascites, coarse echotexture, and low albumin). The biopsy will show both acute inflammation and chronic fibrosis. 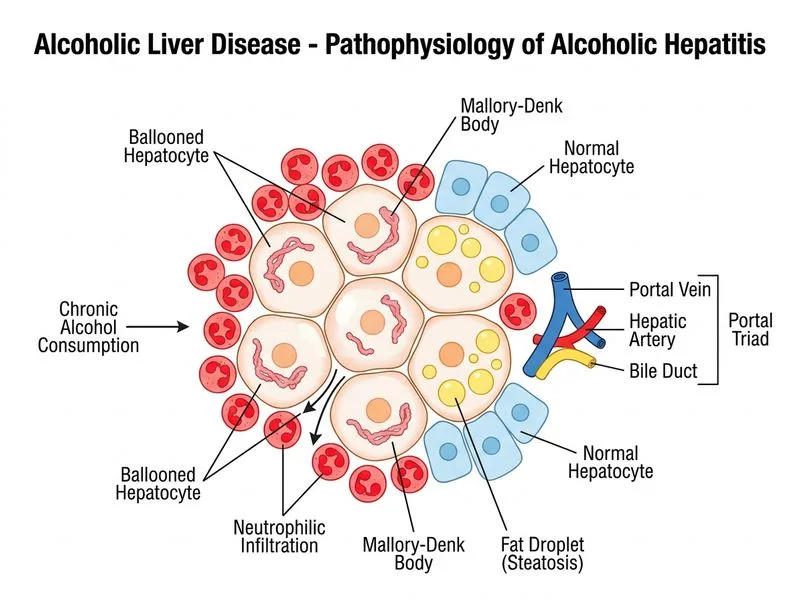
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.