## Clinical Assessment This patient presents with **decompensated cirrhosis** (ascites, encephalopathy, coagulopathy) secondary to alcoholic liver disease. The AST/ALT ratio >2 and clinical context confirm alcoholic aetiology. The constellation of findings—INR >2.5, bilirubin >5 mg/dL, grade II encephalopathy, and thrombocytopenia—indicates **acute-on-chronic liver failure (ACLF)** or end-stage cirrhosis. ## Management Hierarchy **Key Point:** In a patient with decompensated cirrhosis and encephalopathy, immediate priorities are: 1. **Supportive care** to stabilize acute complications 2. **Assess transplant candidacy** (MELD score, contraindications, abstinence period) 3. **Referral** only after stabilization and candidacy assessment ### Immediate Interventions - **Lactulose** — first-line for hepatic encephalopathy; reduces ammonia absorption - **Rifaxomicin** — non-absorbed antibiotic; reduces ammonia-producing bacteria (preferred over neomycin in current practice) - **Nutritional support** — branched-chain amino acids (BCAA), protein restriction if worsening encephalopathy - **Abstinence counselling** — mandatory; transplant requires ≥6 months sobriety (some centres 3 months) ### Why Not Immediate Transplant Referral? **Clinical Pearl:** Transplant centres require: - Stabilization of acute complications first - Demonstration of 6-month abstinence (or 3 months in selected ACLF cases) - Exclusion of active infection, malignancy, cardiopulmonary contraindications - MELD score calculation and waitlist prioritization Direct referral without stabilization and abstinence assessment is premature and wastes transplant resources. ### Why Not Corticosteroids or Pentoxifylline? **Warning:** These agents are indicated only in **alcoholic hepatitis** (acute inflammation with jaundice, elevated transaminases, and systemic inflammation). This patient has **cirrhosis with decompensation**, not acute hepatitis. Corticosteroids increase infection risk in cirrhotic patients and are contraindicated in the presence of active encephalopathy or renal dysfunction. ### Why Not Ursodeoxycholic Acid? Ursodeoxycholic acid is used in primary biliary cholangitis (PBC) and primary sclerosing cholangitis (PSC), not alcoholic cirrhosis. It has no proven benefit in alcoholic liver disease. ## High-Yield Summary Table | Scenario | Next Step | | --- | --- | | Acute alcoholic hepatitis (no cirrhosis) | Corticosteroids (if Maddrey score ≥32) + pentoxifylline | | Decompensated cirrhosis, stable | Supportive care + assess transplant candidacy | | Decompensated cirrhosis + ACLF | Supportive care + ICU monitoring + urgent transplant evaluation | | Variceal bleeding + cirrhosis | Variceal ligation/sclerotherapy + propranolol + antibiotics | [cite:Harrison 21e Ch 297] 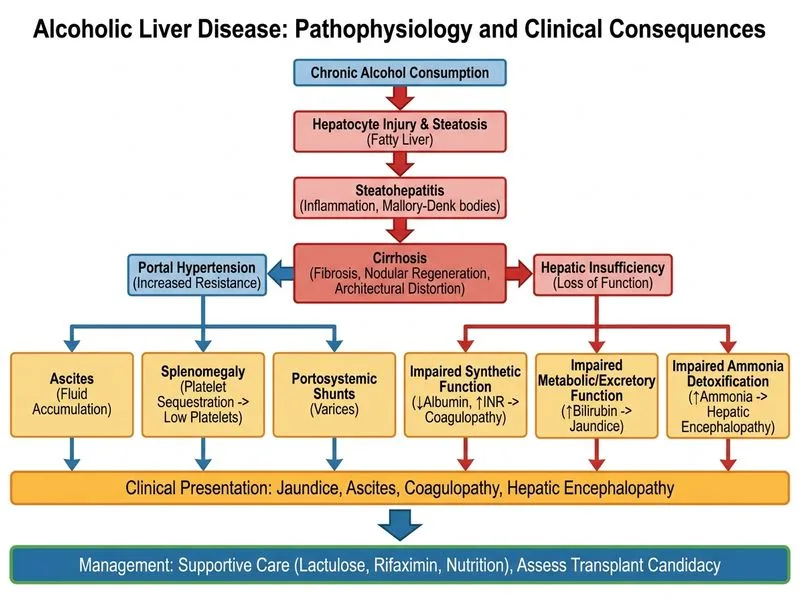
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.