## Clinical Context The patient presents with microcytic anemia (MCV 62 fL), low ferritin (12 ng/mL), and clinical signs of iron deficiency (glossitis, pallor). The triad of anemia, low MCV, and low ferritin is diagnostic of iron deficiency anemia (IDA). ## Why Upper GI Endoscopy Is Correct **Key Point:** In iron deficiency anemia, once the diagnosis is confirmed biochemically, the next step is to identify the source of blood loss. Upper GI endoscopy is the investigation of choice for suspected upper GI bleeding in IDA. **Clinical Pearl:** Glossitis (inflamed tongue) and dysphagia are classic signs of chronic iron deficiency and warrant investigation for occult GI bleeding. The most common sources in India are peptic ulcer disease and gastric malignancy. **High-Yield:** The diagnostic algorithm for IDA is: 1. Confirm diagnosis: low Hb, low MCV, low ferritin, elevated TIBC 2. Identify source: Upper GI endoscopy (if upper GI symptoms or age >40) → Lower GI colonoscopy (if no upper source found) 3. Treat underlying cause + iron supplementation ## Why Other Options Are Incorrect | Investigation | Why Not Chosen | |---|---| | **Serum B12 and folate** | The MCV is low (microcytic), not macrocytic. B12/folate deficiency causes macrocytic anemia. | | **Peripheral smear and reticulocyte count** | These are supportive tests but do not identify the cause of iron loss. Reticulocyte count helps assess bone marrow response but is not the next investigation. | | **Bone marrow aspiration** | Invasive and unnecessary when biochemical markers (ferritin, TIBC, serum iron) already confirm IDA. Reserved for cases with diagnostic uncertainty or concurrent cytopenias. | 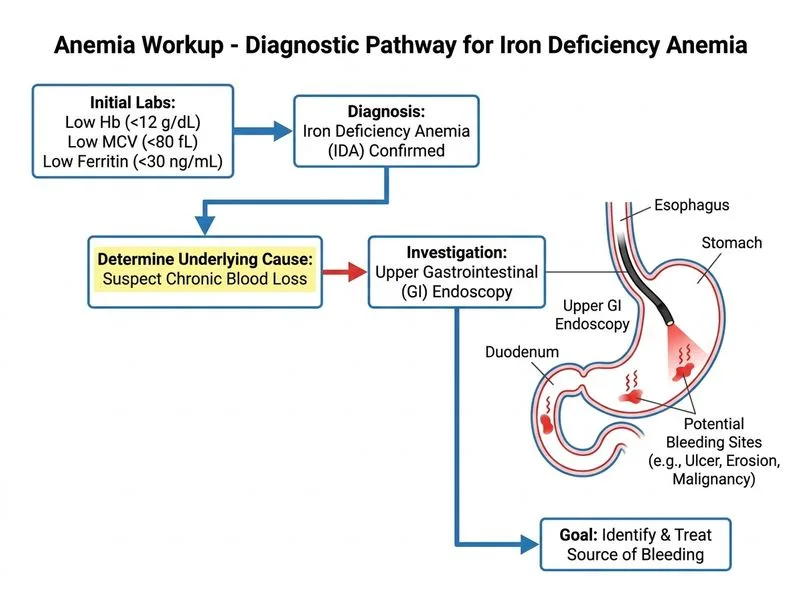
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.