## Clinical Context This patient presents with **iron deficiency anemia (IDA)** with clear biochemical confirmation: low serum iron, low ferritin, elevated TIBC, and microcytic hypochromic indices. The diagnosis is established. ## Rationale for Correct Answer **Key Point:** Once iron deficiency anemia is biochemically confirmed, the immediate next step is to **initiate iron replacement therapy**, not to investigate the cause first. In India, the most common causes of IDA are: - Nutritional deficiency (especially in rural/lower socioeconomic populations) - Chronic blood loss (GI, menstrual, hookworm) Oral iron therapy is the **first-line and preferred route** in uncomplicated IDA: - Ferrous salts (sulfate, gluconate, fumarate) are most bioavailable - Standard dose: 200 mg elemental iron daily - Expected reticulocytosis in 3–5 days - Hemoglobin rise of 1–2 g/dL per month - Cost-effective and well-tolerated in most patients **Clinical Pearl:** Response to iron therapy is itself diagnostic — a rising reticulocyte count and hemoglobin within 3 weeks confirms iron deficiency and rules out other causes of microcytic anemia (thalassemia trait, sideroblastic anemia). ## When to Investigate the Cause Investigation for the **source of blood loss** (endoscopy, imaging) is warranted **after**: 1. Confirming response to iron therapy (therapeutic trial) 2. In post-menopausal women or men (no physiologic blood loss) 3. If anemia is severe (Hb < 5 g/dL) or symptomatic 4. If there is clinical suspicion of GI malignancy This patient is pre-menopausal; menstrual loss or nutritional deficiency is most likely. Endoscopy is not the immediate next step. ## Why Not IV Iron or Further Testing? - **IV iron** is reserved for: malabsorption, intolerance to oral iron, or need for rapid repletion (pregnancy, pre-operative) - **Transferrin saturation & sTfR** are confirmatory tests, not management steps; they add no value once diagnosis is made [cite:Harrison 21e Ch 97] 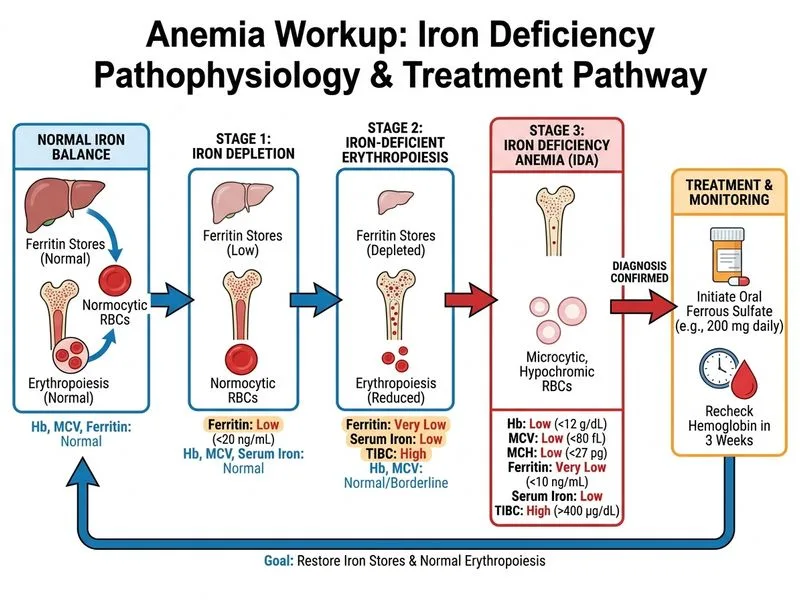
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.