## Clinical Diagnosis: Iron Deficiency Anemia ### Key Laboratory Findings | Parameter | Patient Value | Normal Range | Interpretation | |-----------|---------------|--------------|----------------| | Hemoglobin | 7.2 g/dL | 12–16 g/dL | Moderate anemia | | MCV | 62 fL | 80–100 fL | Microcytic | | MCH | 18 pg | 27–33 pg | Hypochromic | | RBC count | 5.8 × 10^12/L | 4.0–5.5 × 10^12/L | Elevated (relative) | | Serum iron | 25 μg/dL | 60–170 μg/dL | **Markedly low** | | Ferritin | 8 ng/mL | 12–150 ng/mL | **Depleted stores** | | TIBC | 420 μg/dL | 250–425 μg/dL | Upper normal/elevated | | Transferrin saturation | 6% | 20–50% | **Severely reduced** | **Key Point:** The combination of **low serum iron, low ferritin, elevated TIBC, and reduced transferrin saturation** is pathognomonic for iron deficiency anemia. Ferritin < 12 ng/mL is the most sensitive marker of iron depletion. ### Pathophysiology 1. **Source of iron loss:** Chronic menorrhagia (2 years) → continuous blood loss 2. **Iron stores depletion:** Ferritin falls first 3. **Serum iron depletion:** Transferrin saturation drops 4. **Erythropoiesis impairment:** Microcytic, hypochromic RBCs develop 5. **Compensatory response:** RBC count increases (attempt to maintain oxygen delivery) ### Peripheral Blood Smear Findings **High-Yield:** - Microcytic, hypochromic RBCs (reduced hemoglobin content) - Target cells (due to relative increase in cell membrane relative to hemoglobin) - Occasional pencil cells (severe hypochromia) - Anisocytosis (variation in RBC size) ### Diagnostic Criteria for Iron Deficiency Anemia **Mnemonic: TIBC-FS** (Transferrin Iron Ferritin Saturation) - **T**IBIC: Elevated (> 400 μg/dL) - **I**ron: Low (< 60 μg/dL) - **B**ody stores (Ferritin): Depleted (< 12 ng/mL) - **F**erritin: Low - **S**aturation: Reduced (< 16%) ### Clinical Pearl In a woman of reproductive age with microcytic anemia and menorrhagia, iron deficiency is the diagnosis until proven otherwise. The severely low ferritin (8 ng/mL) is diagnostic — ferritin is an acute phase reactant and will be falsely elevated in inflammation, so a low ferritin in anemia is highly specific for iron depletion. ### Next Steps in Management 1. Confirm diagnosis with bone marrow iron stain (Prussian blue) — absent iron 2. Investigate source of blood loss (gynecology referral for menorrhagia management) 3. Initiate iron supplementation (ferrous sulfate 325 mg daily) 4. Recheck hemoglobin in 4–6 weeks (expect rise of 1–2 g/dL per week) [cite:Harrison 21e Ch 90] 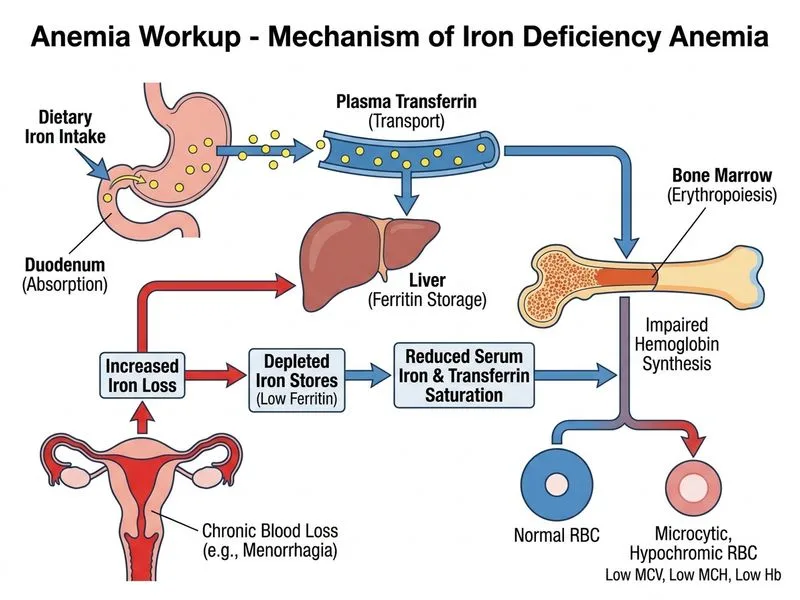
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.