## Clinical Diagnosis: Anemia of Chronic Disease (ACD) Secondary to CKD ### Pathophysiology of ACD in CKD 1. **Erythropoietin (EPO) deficiency:** Kidneys produce 90% of EPO; reduced GFR → inadequate EPO secretion 2. **Impaired RBC lifespan:** Uremic toxins shorten RBC survival 3. **Iron sequestration:** Hepcidin elevation (due to inflammation) → iron trapping in macrophages 4. **Blunted reticulocyte response:** Inadequate EPO → insufficient reticulocytosis despite anemia 5. **Chronic inflammation:** CKD induces low-grade inflammation (elevated IL-6, TNF-α, CRP) ### Key Laboratory Differentiation | Feature | Patient Value | ACD Pattern | IDA Pattern | |---------|---------------|-------------|-------------| | Hemoglobin | 8.5 g/dL | Low | Low | | MCV | 88 fL | Normal/low-normal | **Microcytic** | | Serum iron | 95 μg/dL | **Normal/low-normal** | **Very low** | | Ferritin | 285 ng/mL | **Elevated/normal** | **Very low** | | TIBC | 280 μg/dL | **Normal/low** | **Elevated** | | Transferrin saturation | 34% | **Normal** | **Very low** | | Reticulocyte count | 0.8% | **Inappropriately low** | Variable | | Iron stores (bone marrow) | — | **Present** | **Absent** | **Key Point:** ACD is characterized by **normal or elevated ferritin with normal iron studies** — the iron is present but sequestered and unavailable for erythropoiesis. This contrasts sharply with iron deficiency anemia, where ferritin is depleted. ### Why Reticulocyte Count is Diagnostic **High-Yield:** In a patient with Hb 8.5 g/dL (moderate anemia), the reticulocyte count should be **> 2–3%** as a compensatory response. A reticulocyte count of 0.8% is **inappropriately low** and indicates: - Bone marrow failure to respond to anemia (hypoproliferative) - EPO deficiency (hallmark of ACD in CKD) - NOT hemolysis (which would show high reticulocytes) - NOT iron deficiency alone (which would show some reticulocytosis) ### Mnemonic: ACD vs. IDA — "FERRITIN tells the tale" - **F**erritin **E**levated → **ACD** (iron sequestered, stores intact) - **F**erritin **D**epleted → **IDA** (iron lost, stores empty) ### Clinical Pearl ACD is the **second most common cause of anemia in hospitalized patients** (after IDA). In CKD, it is nearly universal by eGFR < 30 mL/min/1.73m². The normocytic normochromic RBC morphology and normal iron panel rule out IDA; the low reticulocyte count rules out hemolysis. ### Management of ACD in CKD 1. **Erythropoiesis-stimulating agents (ESAs):** Epoetin alfa or darbepoetin alfa (target Hb 10–11 g/dL) 2. **Iron supplementation:** Even with normal iron studies, iron supplementation may improve ESA response 3. **Treat underlying CKD:** ACE inhibitors, ARBs, SGLT2 inhibitors 4. **Manage inflammation:** Control blood pressure, reduce uremic toxins via dialysis 5. **Avoid ESA overtreatment:** Target Hb > 12 g/dL increases cardiovascular risk [cite:Harrison 21e Ch 90; KDIGO 2021 Anemia in CKD] 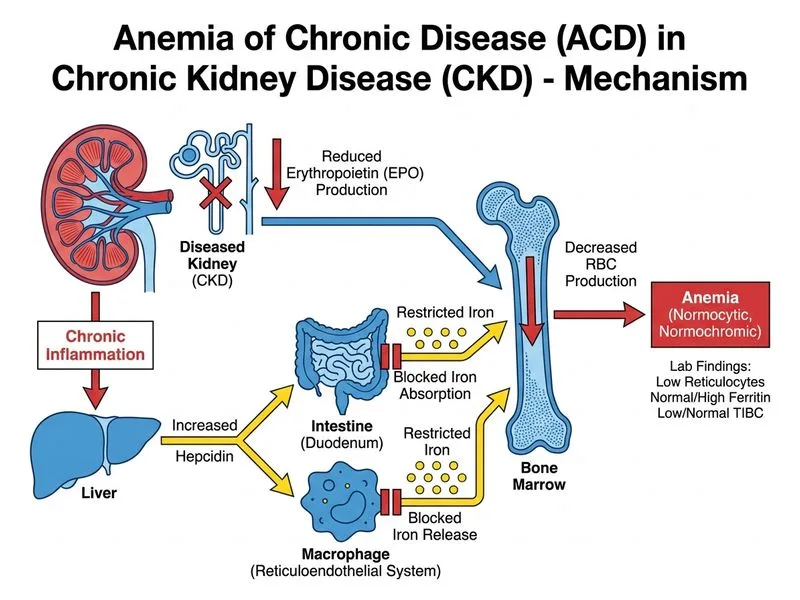
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.