## Clinical Diagnosis: Anemia of Chronic Kidney Disease ### Clinical Context This patient presents with anemia in the setting of **advanced chronic kidney disease (CKD Stage 3b-4)** with creatinine 2.1 mg/dL and eGFR 28 mL/min. The bone pain is a clue to secondary hyperparathyroidism and renal osteodystrophy, common in CKD. ### Laboratory Interpretation | Parameter | Value | Interpretation | |-----------|-------|----------------| | Hemoglobin | 8.9 g/dL | Moderate anemia | | MCV | 78 fL | Microcytic | | Serum creatinine | 2.1 mg/dL | Moderate renal impairment | | eGFR | 28 mL/min | CKD Stage 3b | | Serum iron | 92 µg/dL | Normal (60–170 µg/dL) | | TIBC | 280 µg/dL | Normal (250–425 µg/dL) | | Serum ferritin | 180 ng/mL | **Elevated** (normal < 30 ng/mL) | | Reticulocyte count | 0.8% | **Inappropriately low** for degree of anemia (should be > 2%) | | Bone marrow | Normocellular, adequate iron | **No iron deficiency; no dysplasia** | **Key Point:** The **inappropriately low reticulocyte response** (0.8% when Hb is 8.9 g/dL) in a patient with renal impairment is pathognomonic for **erythropoietin (EPO) deficiency**—the hallmark of anemia of CKD. ### Pathophysiology of Anemia in CKD 1. **Reduced EPO production**: Kidneys produce 90% of EPO; GFR < 30 mL/min → severe EPO deficiency 2. **Shortened RBC lifespan**: Uremic toxins damage RBC membrane 3. **Iron metabolism**: Hepcidin dysregulation (but iron stores adequate in this case) 4. **Bone marrow suppression**: Uremic toxins inhibit erythropoiesis 5. **Result**: Normocytic or **slightly microcytic** anemia with **blunted reticulocyte response** **High-Yield:** Anemia of CKD is the **most common cause of anemia in patients with eGFR < 30 mL/min**. The reticulocyte count is the key discriminator: it is inappropriately low relative to the degree of anemia. ### Why NOT the Other Options? #### Anemia of Chronic Disease (ACD) from RA - ACD causes **normocytic or slightly microcytic** anemia ✓ (matches this case) - BUT: ACD is typically mild (Hb > 10 g/dL) unless very severe RA - **Ferritin is elevated in ACD** ✓ (matches this case) - **However**: The reticulocyte count in ACD is also low, making it a differential - **Distinguishing feature**: **The degree of renal impairment (eGFR 28) is the dominant factor**; CKD is the primary driver of anemia here, not RA alone - If only RA, we would expect normal renal function #### Iron Deficiency Anemia - Serum ferritin is 180 ng/mL (elevated, not low) → **rules out IDA** - Serum iron is normal → **rules out IDA** - TIBC is normal → **rules out IDA** - Bone marrow has adequate iron stores → **rules out IDA** #### Sideroblastic Anemia - Methotrexate can rarely cause sideroblastic changes, but bone marrow shows **no dysplasia, no ringed sideroblasts** - Ferritin would be elevated (matches), but diagnosis requires bone marrow findings - Reticulocyte count would not be this low - Rare and not the primary diagnosis in this CKD patient **Clinical Pearl:** In CKD, measure **EPO level** and **reticulocyte count**. A low reticulocyte count (< 1.5%) with anemia in CKD confirms EPO deficiency and indicates need for ESA (erythropoiesis-stimulating agent) therapy. ### Management Implications - **First-line**: Recombinant human EPO (epoetin alfa) or ESA (darbepoetin alfa) - **Iron supplementation**: May be needed if iron studies become depleted - **Target Hb**: 10–11 g/dL (avoid over-correction; increases cardiovascular risk) - **Address secondary hyperparathyroidism** (bone pain suggests this) **Mnemonic: "CKD Anemia = EPO Deficiency"** — When eGFR < 30 and reticulocyte count is low, think EPO deficiency first. 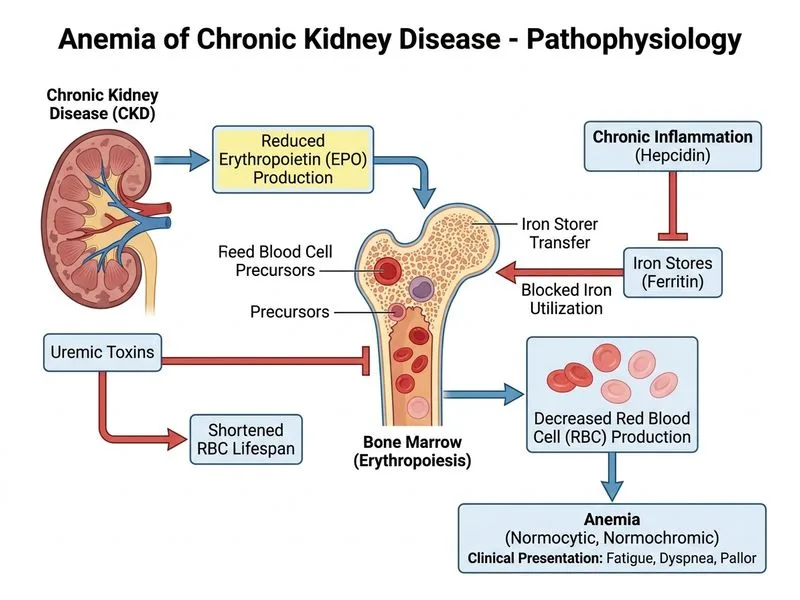
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.