## Clinical Context This patient has a tuberculous cavity with secondary aspergilloma causing significant haemoptysis (200 mL/day). The clinical scenario requires urgent haemostasis while maintaining medical therapy. ## Why Bronchial Artery Embolisation is Correct **Key Point:** Bronchial artery embolisation (BAE) is the first-line interventional radiological treatment for massive haemoptysis in patients with cavitary TB and aspergilloma when bronchoscopy is not feasible or contraindicated. **High-Yield:** BAE achieves haemostasis in 85–90% of cases of TB-related haemoptysis, with recurrence rates of 10–15% at 1 year. It bridges the patient through the acute bleeding phase while anti-TB therapy continues. **Clinical Pearl:** The bronchial arteries (typically 1–2 mm diameter, arising from the descending thoracic aorta at T5–T6 level) are hypertrophied in chronic TB and aspergilloma due to chronic inflammation and neovascularisation. These are the primary bleeding source in haemoptysis, not the pulmonary circulation. ## Technique & Indications **Indications for BAE in TB-related haemoptysis:** - Massive haemoptysis (>200 mL/24 hr) with haemodynamic instability or respiratory compromise - Recurrent haemoptysis despite medical therapy - Aspergilloma in a cavity - Contraindication to surgery or bronchoscopy **Procedure:** 1. Femoral artery access; catheterisation of descending thoracic aorta 2. Selective bronchial artery catheterisation (may be bilateral) 3. Angiography to identify hypertrophied bronchial arteries and confirm bleeding source 4. Embolisation using polyvinyl alcohol (PVA) particles (150–250 µm or 250–350 µm) or coils 5. Post-embolisation angiography to confirm cessation of flow **Contraindications to BAE:** - Spinal artery arising from the bronchial artery (risk of spinal cord infarction) — recognised on angiography - Severe aortic atherosclerosis preventing catheterisation - Uncorrected coagulopathy ## Why Other Options Are Incorrect **Percutaneous transthoracic needle aspiration:** Does not address the bleeding source; risks further haemorrhage and pneumothorax. Not indicated for haemostasis. **Immediate surgical resection:** Considered only after failed BAE or in stable patients with recurrent haemoptysis despite BAE. Surgery in acute massive haemoptysis carries high mortality (15–30%) due to difficulty in airway management and blood loss control intraoperatively. **Conservative management:** Inappropriate for 200 mL/day haemoptysis. Observation alone risks exsanguination and respiratory failure. Anti-TB therapy alone does not acutely stop bleeding from an aspergilloma. ## Management Algorithm ```mermaid flowchart TD A[TB cavity with aspergilloma + haemoptysis]:::outcome --> B{Haemoptysis volume & stability?}:::decision B -->|Mild <50 mL/day| C[Medical management + anti-TB]:::action B -->|Massive ≥200 mL/day| D{Bronchoscopy feasible?}:::decision D -->|Yes| E[Bronchoscopic localisation + endobronchial therapy]:::action D -->|No/Contraindicated| F[Bronchial artery embolisation]:::action F --> G[Angiography + selective BAE]:::action G --> H{Success?}:::decision H -->|Yes| I[Continue anti-TB therapy]:::action H -->|No/Recurrence| J[Surgical resection]:::action ``` ## Complications of BAE | Complication | Frequency | Prevention | | --- | --- | --- | | Spinal cord infarction | 0.5–2% | Identify spinal artery on angiography; use proximal embolisation or avoid if spinal artery present | | Oesophageal ulceration | 1–3% | Avoid embolisation of oesophageal arteries | | Recurrent haemoptysis | 10–15% at 1 year | May require repeat BAE or surgery | | Aortic dissection | <1% | Careful catheter manipulation; avoid aggressive guidewire advancement | | Contrast-induced nephropathy | 2–5% | Hydration; consider iso-osmolar contrast | **Key Point:** BAE is a temporising measure, not curative. It controls acute bleeding and allows time for anti-TB therapy to take effect. Definitive cure requires completion of anti-TB therapy (6–9 months) and, if needed, surgical resection of the cavity. 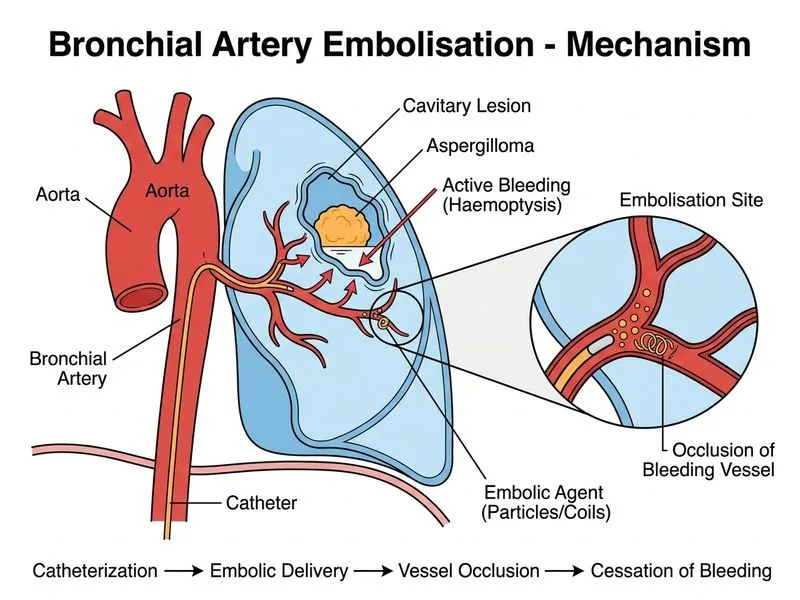
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.