## Clinical Context This patient has acute obstructive jaundice from a CBD stone with failed ERCP due to anatomical difficulty (duodenal diverticulum). The patient is stable without acute pancreatitis, making this a planned intervention scenario. ## Why Percutaneous Transhepatic Cholangiography with PTBD is Correct **Key Point:** When ERCP fails due to anatomical obstruction (duodenal diverticulum, altered anatomy, stricture), percutaneous transhepatic cholangiography (PTC) with percutaneous transhepatic biliary drainage (PTBD) is the first-line alternative interventional radiological approach for biliary decompression and stone management. **High-Yield:** PTC-PTBD has a success rate of 95–98% in achieving biliary decompression and is indicated in: - Failed ERCP with obstructive jaundice - Anatomical contraindications to ERCP (duodenal diverticulum, altered anatomy post-surgery, duodenal obstruction) - Proximal CBD strictures or hilar cholangiocarcinoma - Acute cholangitis unresponsive to antibiotics **Clinical Pearl:** In this case, the duodenal diverticulum at the ampulla makes ERCP technically difficult or impossible. PTC-PTBD bypasses the need for endoscopic access and allows direct access to the biliary tree from the liver. ## PTC-PTBD Technique & Indications **Procedure:** 1. **Access:** Percutaneous puncture of a dilated intrahepatic bile duct (usually right anterior or posterior duct) under ultrasound or fluoroscopic guidance 2. **Catheterisation:** Guidewire and catheter advanced into the CBD and duodenum 3. **Drainage:** Pigtail catheter placed across the obstruction (external drainage) or into the duodenum (internal-external drainage) 4. **Stone management:** Once drainage is established, stones can be extracted via the percutaneous tract (percutaneous cholangioscopy + mechanical lithotripsy) or left for later ERCP via the mature tract **Advantages of PTC-PTBD:** - High technical success (95–98%) - Effective in anatomically difficult cases - Allows both drainage and therapeutic intervention (stone extraction, stent placement) - Can be converted to internal drainage once acute phase resolves **Timing:** In a stable, afebrile patient without pancreatitis, PTC-PTBD can be performed electively within 24–48 hours. In acute cholangitis, it is emergent (within 12 hours). ## Why Other Options Are Incorrect **Surgical CBD exploration:** Indicated for failed endoscopic and percutaneous interventions, or in patients unfit for percutaneous intervention. In a stable patient with a patent percutaneous route available, surgery is not first-line. Operative mortality in elective CBD exploration is 1–2%, but morbidity is higher than percutaneous approach. **Repeat ERCP with double-guide-wire technique:** While double-guide-wire technique can aid in difficult ERCP cases, the anatomical obstruction (duodenal diverticulum at ampulla) is a structural contraindication to ERCP, not a technical failure amenable to repeated attempts. Repeated ERCP attempts increase pancreatitis risk (5–7% per attempt) and are not justified here. **ESWL followed by observation:** Extracorporeal shock wave lithotripsy is used for intrahepatic stones or large CBD stones (>20 mm) in selected cases, but it is not first-line for acute obstructive jaundice. ESWL requires multiple sessions, carries risk of pancreatitis, and does not provide immediate drainage. In this case, the patient has obstructive jaundice and needs urgent decompression, not fragmentation alone. ## Management Algorithm for Failed ERCP ```mermaid flowchart TD A[Obstructive jaundice + CBD stone]:::outcome --> B[ERCP attempted]:::action B --> C{ERCP successful?}:::decision C -->|Yes| D[Sphincterotomy + stone extraction]:::action C -->|No| E{Reason for failure?}:::decision E -->|Anatomical obstruction| F[PTC-PTBD]:::action E -->|Technical difficulty| G[Repeat ERCP ± double-guide-wire]:::action E -->|Altered anatomy/post-surgery| F F --> H[Biliary drainage established]:::outcome H --> I{Stone size & location?}:::decision I -->|Small CBD stone| J[Percutaneous cholangioscopy + extraction]:::action I -->|Large stone| K[ESWL or surgical extraction]:::action J --> L[Remove PTBD catheter]:::action K --> L ``` ## Comparison: ERCP vs. PTC-PTBD | Feature | ERCP | PTC-PTBD | | --- | --- | --- | | **Access** | Endoscopic (via ampulla) | Percutaneous (via liver) | | **Success rate** | 85–95% (lower in altered anatomy) | 95–98% | | **Anatomical contraindications** | Duodenal diverticulum, altered anatomy, duodenal obstruction | None (if dilated ducts) | | **Pancreatitis risk** | 3–7% | <1% | | **Time to drainage** | Immediate (if successful) | 24–48 hrs (elective); <12 hrs (emergency) | | **Stone extraction** | Direct via sphincterotomy | Via percutaneous tract (cholangioscopy) | | **Morbidity** | 5–10% (post-sphincterotomy bleeding, pancreatitis) | 5–8% (sepsis, catheter dislodgement, bile leak) | | **First-line in failed ERCP?** | No | Yes | **Key Point:** PTC-PTBD is the gold-standard alternative when ERCP fails due to anatomical obstruction. It provides reliable biliary decompression and allows staged stone extraction. 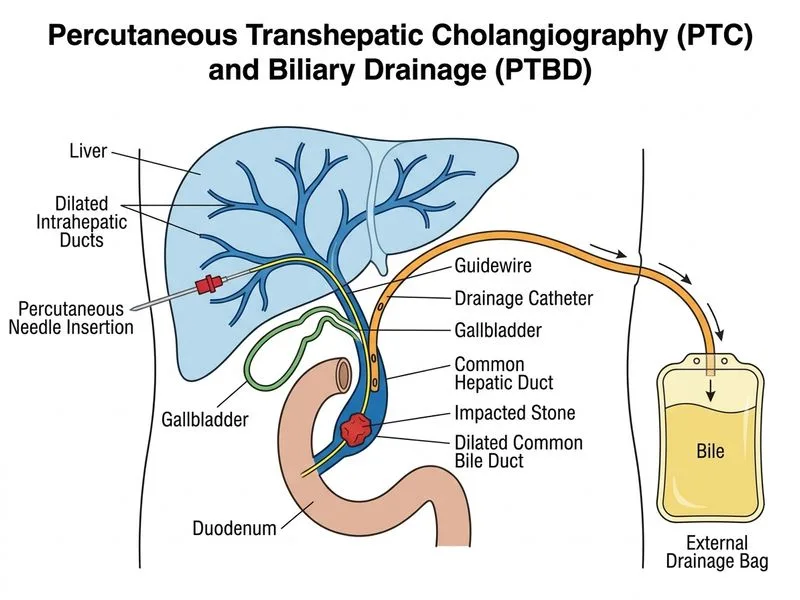
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.