## Mechanism of Spinal Instability in Advanced Ankylosing Spondylitis ### Pathophysiology of AS-Related Spine Fragility Ankylosing spondylitis causes progressive fusion of the spine through **syndesmophyte formation** — bony bridges that fuse vertebral bodies, facet joints, and ligaments. Over decades, this creates a **rigid, bamboo-like spine** that is paradoxically brittle and osteoporotic. **Key Point:** The fused AS spine loses its normal segmental mobility and shock-absorbing capacity. Instead of distributing forces across multiple joints, all stress concentrates at the level of fracture, creating a **long-lever-arm effect**. ### Why Option 1 (Correct Answer) is Best The syndesmophytes create: 1. **Rigid fusion** — eliminates normal spinal flexibility 2. **Osteoporosis** — AS patients have reduced bone mineral density (BMD) due to chronic inflammation and immobility 3. **Lever-arm concentration** — a minor fall that would normally be absorbed by segmental motion instead creates a shear force concentrated at a single level 4. **Fracture pattern** — fractures in AS often occur through the disc space or syndesmophyte (as in this case), not through normal bone This explains why **trivial trauma** (standing fall, sneeze, cough) can cause catastrophic fractures with cord compression in advanced AS. **Clinical Pearl:** AS patients with advanced disease are at **50–100× higher risk** of spinal fracture than the general population, and fractures are often **unstable and neurologically devastating**. ### Why Each Distractor is Wrong **Option 0 (OPLL):** While OPLL does narrow the spinal canal and increase vulnerability, it is a separate condition (common in East Asian populations with cervical spondylosis) and is NOT the primary mechanism of instability in AS. OPLL does not explain the **lever-arm effect** or the **osteoporotic fragility** unique to AS. **Option 2 (Facet/disc destruction):** Facet joint and disc involvement occurs in AS, but these are **secondary to syndesmophyte fusion**, not the primary mechanism. The key problem is not inflammation per se, but the **rigid fusion** that concentrates forces. **Option 3 (Ligamentum flavum calcification):** This is a feature of cervical spondylosis and OPLL, not AS. It does not explain the **osteoporosis**, **syndesmophyte fusion**, or **lever-arm instability** seen in AS. ### Imaging & Clinical Correlation ```mermaid flowchart TD A[Advanced AS: Syndesmophyte fusion + Osteoporosis]:::outcome --> B[Rigid spine loses shock absorption]:::outcome B --> C[Minor trauma: fall, cough, sneeze]:::action C --> D{Force distribution?}:::decision D -->|Normal spine| E[Force absorbed across multiple levels]:::action D -->|AS spine| F[Force concentrated at single level]:::urgent F --> G[Shear stress through disc/syndesmophyte]:::urgent G --> H[Fracture with posterior displacement]:::urgent H --> I[Cord compression + Paraplegia]:::urgent ``` **High-Yield:** Fractures in AS are often **unstable** and require **urgent surgical stabilization**. Delayed diagnosis or conservative management can lead to progressive neurological deterioration. ## Management Implications - **Imaging:** MRI to assess cord compression; CT for fracture pattern - **Urgent surgical stabilization** (fusion) is usually indicated - **Mortality:** Spinal fractures in AS have high morbidity and mortality if not treated urgently [cite:Harrison 21e Ch 337] 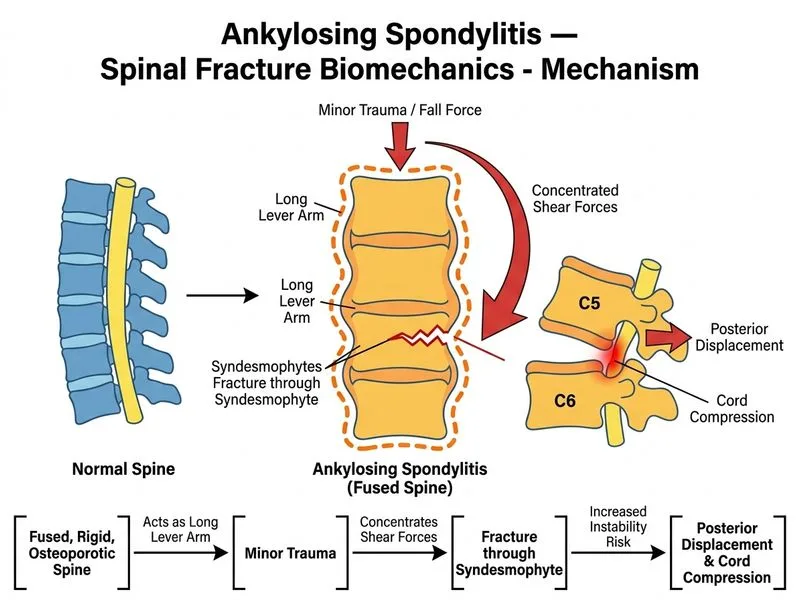
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.