## Biomechanics of Fracture in Ankylosing Spondylitis **Key Point:** Ankylosing spondylitis (AS) transforms the spine into a rigid, osteoporotic column that behaves like a long bone rather than a segmented structure. This fundamentally alters fracture mechanics and neurological risk. ### Why the Correct Answer is Right In AS, progressive ossification of the disc and ligaments (including the anterior and posterior longitudinal ligaments and facet joints) creates a **bamboo spine**—a continuous, inflexible bony structure. When subjected to trauma: 1. **Loss of segmental mobility** — Normal spines dissipate energy through intervertebral motion and ligamentous stretch. The fused AS spine cannot do this. 2. **Stress concentration** — All mechanical force is concentrated at a single fracture site rather than distributed across multiple segments. 3. **Osteoporosis** — AS patients have reduced bone mineral density, making the rigid bone more brittle and prone to unstable fractures. 4. **Narrow spinal canal** — The ossification process narrows the canal, leaving little room for cord swelling or displacement without compression. These factors combine to cause **severe, unstable fractures from trivial trauma**—a hallmark of AS spine injury. The fracture often occurs through the disc space (through-and-through fracture) with retropulsion of bone into the canal, causing immediate neurological deficit. **Clinical Pearl:** AS spine fractures are notoriously unstable and have high rates of neurological injury (up to 50% in some series) despite low-energy mechanisms. They are often missed on initial imaging because the rigid spine may show minimal displacement. **High-Yield:** The "3-column" concept applies here—AS fractures typically disrupt all three spinal columns (anterior, middle, posterior) due to the rigid nature of the bone, making them inherently unstable. ### Why the Distractors Are Wrong **Option 1 (Chronic inflammation destroying cord):** While AS is an inflammatory condition, it does not cause primary demyelination or chronic cord degeneration. The neurological injury in AS fractures is acute and mechanical (compression/contusion), not chronic inflammatory. Patients with uncomplicated AS may have normal neurological exams for decades. **Option 2 (Ossified PLL compressing cord pre-fracture):** Although ossification of the posterior longitudinal ligament (OPLL) is a feature of AS and can narrow the canal, it does not cause significant pre-fracture cord compression in most AS patients. The acute neurological deficit in this case is due to the fracture and retropulsion, not the pre-existing OPLL. Additionally, OPLL is more prominent in cervical AS and is a separate pathology (common in Asian populations) from the biomechanical issue at play here. **Option 3 (Glucocorticoid-induced dural weakness):** While chronic corticosteroid use can affect bone quality and wound healing, it does not specifically weaken the dura mater or predispose to cord herniation through fractures. This is a mechanistically incorrect explanation. Dural rupture is rare in AS fractures and is not the primary mechanism of neurological injury. ## Management Implications - **Imaging:** CT with sagittal/coronal reconstruction is essential; MRI to assess cord injury. - **Immobilization:** Most AS fractures require surgical stabilization due to instability. - **Prognosis:** Neurological recovery is often limited; early decompression may help but is not always beneficial if the injury is complete. [cite:Robbins & Cotran 10e Ch 28; Campbell's Operative Orthopaedics 13e Ch 40] 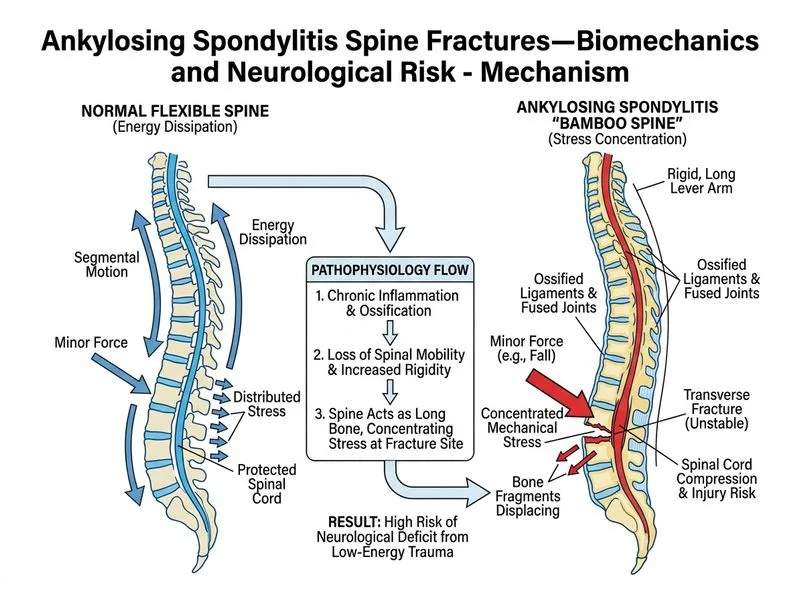
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.