## Digoxin's Mechanism in Atrial Fibrillation Rate Control **Key Point:** Digoxin controls ventricular rate in atrial fibrillation through dual mechanisms: (1) direct AV nodal effects via vagomimetic action, and (2) inhibition of Na⁺/K⁺-ATPase. The vagomimetic effect is the primary rate-control mechanism. ### Digoxin's Dual Mechanism #### 1. **Vagomimetic (Parasympathomimetic) Effect** — PRIMARY for Rate Control - Enhances vagal tone at the AV node - Increases acetylcholine sensitivity - Opens G-protein-coupled K⁺ channels → hyperpolarization - **Result:** ↑↑ AV nodal refractoriness, ↓↓ AV conduction velocity - Slows ventricular response to atrial fibrillation #### 2. **Na⁺/K⁺-ATPase Inhibition** — SECONDARY; Inotropic Effect - Inhibits the cardiac glycoside-binding site on Na⁺/K⁺-ATPase - ↑ Intracellular Na⁺ → ↓ Na⁺/Ca²⁺ exchanger activity → ↑ Intracellular Ca²⁺ - Enhanced sarcoplasmic reticulum calcium storage - **Result:** Positive inotropic effect (improves contractility) - This is why digoxin is beneficial in AF + heart failure **High-Yield:** In atrial fibrillation, digoxin does NOT slow the atrial rate; it only slows the ventricular response by blocking AV nodal conduction. The atrial fibrillation persists. ### Clinical Presentation of Digoxin Toxicity The patient's symptoms (nausea, visual disturbances, hypokalemia, ECG changes) indicate **digoxin toxicity**: | Feature | Mechanism | Clinical Manifestation | |---------|-----------|------------------------| | GI toxicity | Vagal stimulation + direct effect | Nausea, vomiting, anorexia | | Visual toxicity | Retinal effects | Yellow-green halos, blurred vision | | Hypokalemia | Increased Na⁺/K⁺-ATPase activity (paradoxically) | K⁺ shift into cells; ↑ toxicity risk | | ECG: ↓ QT, sagging ST | Increased vagal tone + Na⁺/K⁺-ATPase inhibition | "Digoxin effect" (therapeutic or toxic) | | Arrhythmias | Enhanced automaticity + AV block | Ectopic beats, PACs, VT, bradycardia | **Warning:** Hypokalemia INCREASES digoxin toxicity risk. Potassium supplementation is critical in digoxin-treated patients. ### Digoxin vs Other Rate-Control Agents in AF | Drug Class | Agent | Primary Mechanism | Rate Control | Inotropy | AF Efficacy | |------------|-------|-------------------|--------------|----------|-------------| | Cardiac Glycoside | Digoxin | Vagomimetic + Na⁺/K⁺-ATPase inhibition | ↓↓ AV nodal conduction | ↑↑ (positive) | Moderate | | Beta-blocker | Metoprolol | β1 antagonism | ↓ AV nodal conduction | ↓ (negative) | Good | | CCB | Verapamil | L-type Ca²⁺ channel block | ↓ AV nodal conduction | ↓ (negative) | Good | | Class Ic | Flecainide | Na⁺ channel block | Minimal | ↓ (negative) | Excellent (converts AF) | | Class III | Amiodarone | Multi-channel block | ↓ AV nodal conduction | Variable | Excellent | **Clinical Pearl:** Digoxin is now reserved for AF with concurrent heart failure (where its positive inotropic effect is beneficial) or sedentary patients. It is NOT first-line for rate control in AF without HF because beta-blockers and CCBs are safer and more effective. **Mnemonic for Digoxin Toxicity: "NAVEL"** - **N**ausea / vomiting - **A**rrhythmias (ectopic beats, AV block) - **V**isual disturbances (yellow-green halos) - **E**lectrolyte abnormalities (hypokalemia) - **L**ow heart rate (bradycardia, AV block) [cite:Harrison 21e Ch 297; KD Tripathi 8e Ch 32] 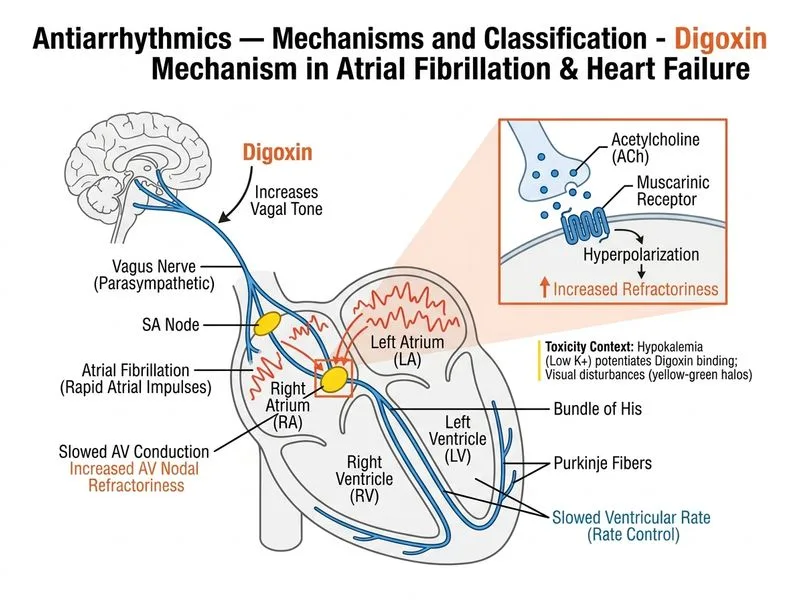
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.