## Investigation of Choice for Post-MI Ventricular Tachycardia Substrate Assessment ### Clinical Context Sustained monomorphic VT in the setting of prior MI reflects a re-entrant circuit within scar tissue. Understanding the extent, location, and characteristics of the scar is essential for: 1. Risk stratification and prognosis 2. Determining candidacy for catheter ablation vs. antiarrhythmic drugs 3. Predicting response to therapy 4. Identifying patients who may benefit from ICD implantation ### Why Cardiac MRI with Late Gadolinium Enhancement (LGE) is Optimal **Key Point:** Cardiac MRI with late gadolinium enhancement is the gold standard for visualizing myocardial scar and fibrosis because: - **Spatial resolution:** Detects scar as small as 1–2 mm with high precision - **Scar characterization:** Distinguishes dense scar (core) from border zone (penumbra), which defines re-entrant circuit anatomy - **Substrate mapping:** Identifies regions of slow conduction and heterogeneous tissue — the substrate for VT - **Ablation planning:** Provides 3D scar geometry for catheter ablation guidance - **Prognostic value:** Scar burden correlates with arrhythmia recurrence and mortality **High-Yield:** LGE-MRI findings in post-MI VT: - Transmural or subendocardial scar (bright signal = fibrosis) - Scar in distribution of infarct-related artery (e.g., anterior wall = LAD territory) - Heterogeneous scar with border zone — site of re-entrant circuit - Scar volume >10 cm³ associated with higher VT recurrence **Clinical Pearl:** In patients with EF ≤35% and prior MI, LGE-MRI helps determine if VT is due to scar-related re-entry (amenable to ablation) vs. other mechanisms, and guides ICD implantation decisions. ### Comparison of Investigations for VT Substrate Assessment | Investigation | Scar Detection | Spatial Resolution | Guides Ablation | Prognostic Value | |---|---|---|---|---| | **Cardiac MRI with LGE** | Excellent | High (1–2 mm) | Yes, 3D mapping | Yes, scar burden | | **Holter monitor** | No | N/A | No | Limited (arrhythmia burden) | | **Transthoracic echo** | No | Poor | No | Wall motion abnormality only | | **Coronary angiography** | No | N/A | No | Assesses coronary patency | ### Antiarrhythmic Strategy Based on Substrate **Mnemonic: SCAR** — **S**car burden, **C**ore vs. border zone, **A**blation candidacy, **R**ecurrence risk. **If extensive scar with poor EF:** - First-line: ICD + amiodarone (Class III agent) - Consider catheter ablation if recurrent ICD shocks **If limited scar with preserved EF:** - Antiarrhythmic monotherapy (sotalol, flecainide, amiodarone) - Catheter ablation may be curative ### Why Other Options Are Incorrect **Holter monitor** — detects arrhythmia frequency and burden but provides no information about substrate anatomy, scar location, or ablation feasibility. It is useful for monitoring treatment response, not for initial substrate assessment. **Transthoracic echocardiography** — assesses global and regional wall motion abnormalities and EF but cannot visualize scar tissue or fibrosis in detail. It does not guide ablation or predict VT mechanism. **Coronary angiography** — identifies coronary stenosis and infarct-related artery but does not characterize myocardial scar or define the VT substrate. It is indicated for revascularization assessment, not arrhythmia mechanism. 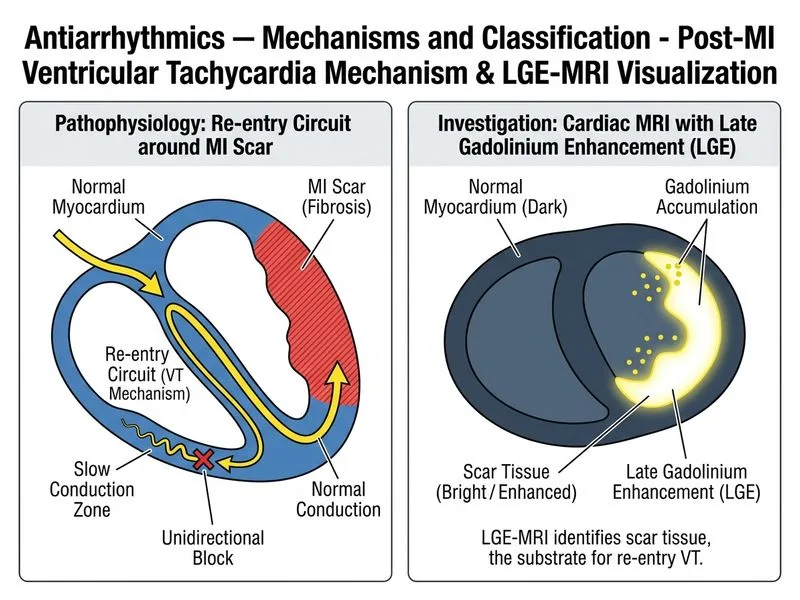
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.