## Diagnosis: Primary Osteoarthritis (OA) ### Clinical and Radiological Context This patient presents with a 10-year history of progressive knee OA with classic degenerative imaging findings. The absence of inflammatory markers, erosions, and soft tissue swelling, combined with the characteristic radiological triad, confirms primary OA. ### Radiological Features of Osteoarthritis **Key Point:** The radiological hallmark of OA is the **Kellgren-Lawrence triad**: joint space narrowing, osteophyte formation, and subchondral sclerosis. These reflect cartilage loss and bone remodeling, not inflammation. ### Kellgren-Lawrence Grading Scale for OA | Grade | Radiological Features | Clinical Correlation | |-------|----------------------|----------------------| | **0** | Normal | No symptoms | | **1** | Doubtful joint space narrowing, possible osteophytes | Minimal symptoms | | **2** | Definite osteophytes, possible joint space narrowing | Mild pain, stiffness | | **3** | Moderate joint space narrowing, multiple osteophytes, sclerosis | Moderate pain, functional limitation | | **4** | Severe joint space narrowing, large osteophytes, severe sclerosis | Severe pain, disability | This patient is **Grade 3–4** based on the imaging description. ### Pathological Basis of Radiological Findings 1. **Joint space narrowing:** Loss of hyaline cartilage due to mechanical wear and enzymatic degradation 2. **Osteophytes (bone spurs):** Marginal bony proliferation as a reparative response to cartilage loss 3. **Subchondral sclerosis:** Increased bone density beneath damaged cartilage due to remodeling and microfractures 4. **Subchondral cysts:** Intra-osseous cysts (geodes) formed by synovial fluid intrusion through cartilage defects **High-Yield:** Subchondral cysts are a hallmark of advanced OA and appear as lucent lesions on plain radiographs and well-defined lesions on MRI. They correlate with cartilage loss above them. ### MRI Findings in OA ```mermaid flowchart TD A[Osteoarthritis MRI Findings]:::outcome --> B[Cartilage Changes]:::action A --> C[Bone Marrow Changes]:::action A --> D[Soft Tissue Changes]:::action B --> B1[Cartilage thinning/loss] B --> B2[Surface irregularity] C --> C1[Bone marrow edema] C --> C2[Subchondral cysts] C --> C3[Osteophytes] D --> D1[Synovial hypertrophy] D --> D2[Effusion] ``` **Clinical Pearl:** Bone marrow edema on MRI in OA indicates active remodeling and is associated with pain progression. It reflects microfractures and increased bone turnover in response to cartilage loss. ### Distinguishing OA from Other Arthropathies | Feature | OA | RA | Psoriatic OA | Gout | |---------|----|----|--------------|------| | **Onset** | Insidious, >40 yrs | Acute, any age | Insidious | Acute | | **Joint space** | Narrowed early | Preserved early | Narrowed | Preserved | | **Erosions** | Central | Marginal | Both | Punched-out | | **Osteophytes** | Prominent | Absent | Minimal | Absent | | **Sclerosis** | Present | Absent | Absent | Absent | | **Soft tissue swelling** | Absent | Symmetrical | Asymmetrical | Tophi | | **Inflammatory markers** | Normal | Elevated | Normal/elevated | Normal | **Warning:** Do not confuse OA with RA based on joint involvement alone. The key differentiators are the radiological pattern (marginal vs. central erosions, presence of osteophytes and sclerosis) and inflammatory markers. ### Why This Patient Has Primary OA - 10-year progressive history (typical for OA) - Bilateral knee involvement (common site for weight-bearing OA) - **Osteophytes with joint space narrowing and sclerosis** (pathognomonic triad) - **Subchondral cysts** (hallmark of advanced OA) - No soft tissue swelling or erosions - No mention of inflammatory markers being elevated [cite:Robbins 10e Ch 6; Kelley's Textbook of Rheumatology Ch 93] 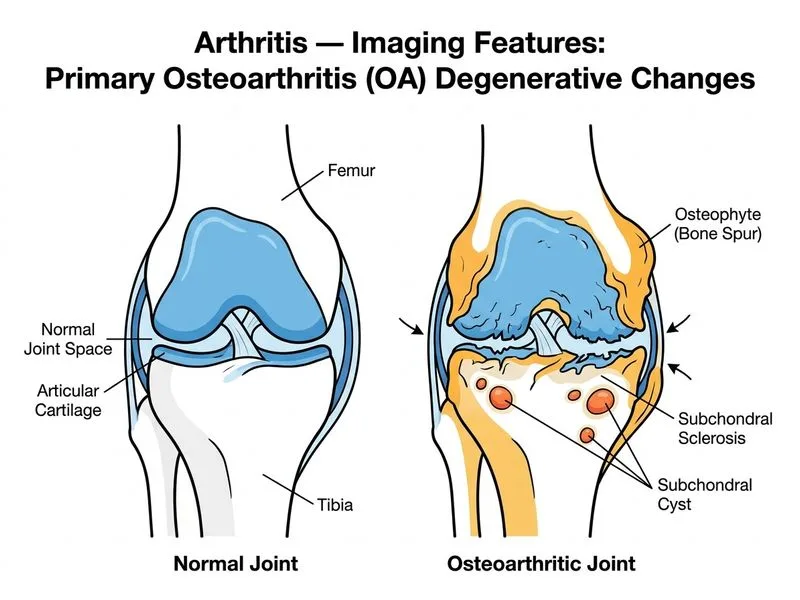
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.