## Acute Asthma Exacerbation: Severity Assessment **Key Point:** This patient has a **moderate-to-severe acute exacerbation** based on: - PEF 55% of personal best (moderate: 40–69%; severe: <40%) - SpO₂ 92% on room air (target >94%) - Use of accessory muscles - Diffuse wheeze on auscultation ## Acute Exacerbation Management Algorithm ```mermaid flowchart TD A[Acute Asthma Exacerbation]:::outcome --> B{Severity Assessment}:::decision B -->|Mild: PEF >80%<br/>SpO₂ >95%| C[SABA + ICS<br/>Oral corticosteroids<br/>Outpatient follow-up]:::action B -->|Moderate: PEF 40-80%<br/>SpO₂ 90-95%| D[Frequent SABA<br/>Oral corticosteroids<br/>Oxygen to SpO₂ >94%<br/>Consider admission]:::action B -->|Severe: PEF <40%<br/>SpO₂ <90%<br/>Silent chest/confusion| E[Continuous SABA nebulization<br/>IV corticosteroids<br/>IV magnesium<br/>Oxygen<br/>ADMIT ICU]:::urgent D --> F[Reassess in 1-2 hours]:::action F --> G{Response?}:::decision G -->|Good| H[Discharge with<br/>ICS + LABA + OCS]:::action G -->|Poor| I[Admit for IV therapy]:::urgent ``` ## Stepwise Treatment for Moderate Exacerbation | Intervention | Rationale | Dosing | |---|---|---| | **Oxygen** | Maintain SpO₂ >94% to ensure adequate tissue oxygenation | Titrate FiO₂ to target | | **SABA (Salbutamol)** | Rapid bronchodilation; frequent dosing in exacerbation | 2.5–5 mg nebulized every 15–20 min × 1 hour, then every 1–4 hours | | **Oral corticosteroids** | Reduce airway inflammation; reduce relapse rate by 50% | Prednisolone 40–50 mg daily × 5–7 days (no taper needed) | | **ICS (increase dose)** | Enhance anti-inflammatory effect; prevent relapse | Double or triple baseline dose; continue after exacerbation | | **Ipratropium** | Anticholinergic; synergistic with SABA (optional in moderate cases) | 0.5 mg nebulized with SABA | **High-Yield:** Oral corticosteroids are MANDATORY in acute exacerbations — they reduce hospital admission and relapse rates. Systemic corticosteroids are superior to increasing inhaled doses alone. **Mnemonic: SOBA** — **S**ABA frequent, **O**xygen to SpO₂ >94%, **B**ronchodilators (SABA ± ipratropium), **A**ntibiotics only if infection suspected. ## Why NOT the Other Options? **Option A (Increase ICS + montelukast):** - Increasing inhaled corticosteroid dose alone is insufficient for acute exacerbation. - Oral (systemic) corticosteroids are required to suppress systemic inflammation. - Montelukast has no role in acute exacerbation management; it is a maintenance agent. **Option C (IV magnesium + aminophylline, admit):** - IV magnesium and aminophylline are reserved for **severe exacerbations** with PEF <40%, SpO₂ <90%, or silent chest. - This patient has moderate exacerbation (PEF 55%, SpO₂ 92%) and can be managed in outpatient/observation setting initially. - Aminophylline has a narrow therapeutic window and is rarely used in modern asthma management; SABA + corticosteroids are first-line. **Option D (Antibiotics + follow-up):** - Antibiotics are NOT indicated unless there is evidence of bacterial infection (fever, productive cough with purulent sputum, pneumonia on CXR). - Asthma exacerbations are usually viral; unnecessary antibiotics promote resistance. - Delaying corticosteroids and SABA therapy increases risk of deterioration. **Clinical Pearl:** The combination of oral corticosteroids + frequent SABA ± oxygen is the cornerstone of acute exacerbation management. Response should be reassessed in 1–2 hours; if poor, admission is indicated. 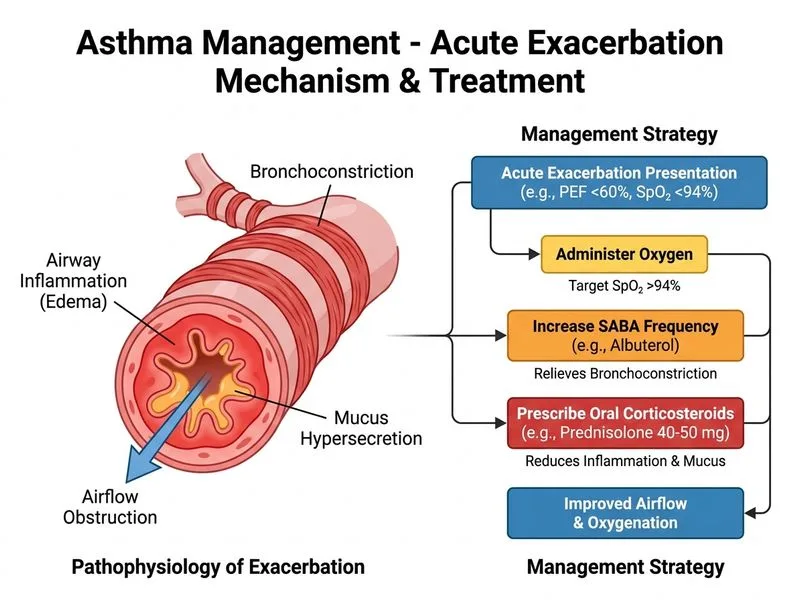
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.