## Acute Asthma Exacerbation: Severity Assessment and Stepwise Management ### Clinical Classification This patient meets criteria for **moderate-to-severe acute exacerbation**: - PEF 60% of predicted (moderate: 40–69%) - Respiratory rate 28/min (tachypnea) - Inability to speak full sentences - Hypoxemia (SpO₂ 92%) **Key Point:** Acute asthma exacerbation severity is determined by PEF, respiratory rate, accessory muscle use, and ability to speak — not just wheezing. ### Immediate Management Algorithm ```mermaid flowchart TD A[Acute asthma exacerbation]:::outcome --> B{Assess severity}:::decision B -->|Mild-moderate| C[SABA nebulized<br/>+ Oral/IV corticosteroid<br/>+ Oxygen to SpO2 94-98%]:::action B -->|Severe/life-threatening| D[SABA + anticholinergic<br/>nebulized immediately]:::action D --> E[IV/oral corticosteroid<br/>Oxygen, IV access]:::action E --> F{Response in 1-2 hrs?}:::decision F -->|Good| G[Discharge on ICS/LABA<br/>+ oral steroid course]:::action F -->|Poor| H[Consider IV magnesium<br/>or IV salbutamol]:::action ``` ### Step-by-Step Rationale 1. **Immediate bronchodilation (0–15 minutes)** - **Salbutamol 5 mg nebulized** (short-acting β₂-agonist, SABA) — rapid onset, reverses bronchoconstriction - **Ipratropium 0.5 mg nebulized** (anticholinergic) — synergistic effect with SABA in moderate-to-severe exacerbations; blocks vagal bronchoconstriction - Combination shown to improve FEV₁ faster than SABA alone in acute exacerbations [cite:Harrison 21e Ch 297] 2. **Oxygen therapy** - Target SpO₂ 94–98% (avoid hyperoxia, which may worsen CO₂ retention in rare cases) - Patient is already hypoxic (92%) 3. **Systemic corticosteroid** (within 1 hour) - Oral prednisolone 40–50 mg or IV hydrocortisone 100 mg - Reduces airway inflammation; takes 4–6 hours to peak effect but must be given early - Oral and IV are equivalent efficacy in non-vomiting patients **High-Yield:** In acute exacerbation, **nebulized SABA + anticholinergic + oxygen + systemic corticosteroid** is the gold standard. Do not delay steroids while awaiting response to bronchodilators. ### Why Option 1 Is Insufficient Oral prednisolone alone without immediate bronchodilation is too slow and inadequate for a patient with PEF 60% and hypoxemia. Bronchodilation must precede or accompany steroid therapy. ### Why Option 3 (IV Magnesium) Is Second-Line Magnesium sulphate is reserved for **severe exacerbations unresponsive to SABA + anticholinergic + steroids** after 1–2 hours. It is not first-line and should not delay SABA/anticholinergic therapy. ### Why Option 4 (Montelukast) Is Inappropriate Leukotriene antagonists are for **chronic asthma control** or mild exacerbations triggered by allergen/exercise. They have no role in acute moderate-to-severe exacerbation management and are far too slow (onset hours). **Clinical Pearl:** Always give SABA + anticholinergic + corticosteroid together in moderate-to-severe exacerbations. Magnesium and IV SABA are rescue therapies for non-responders. 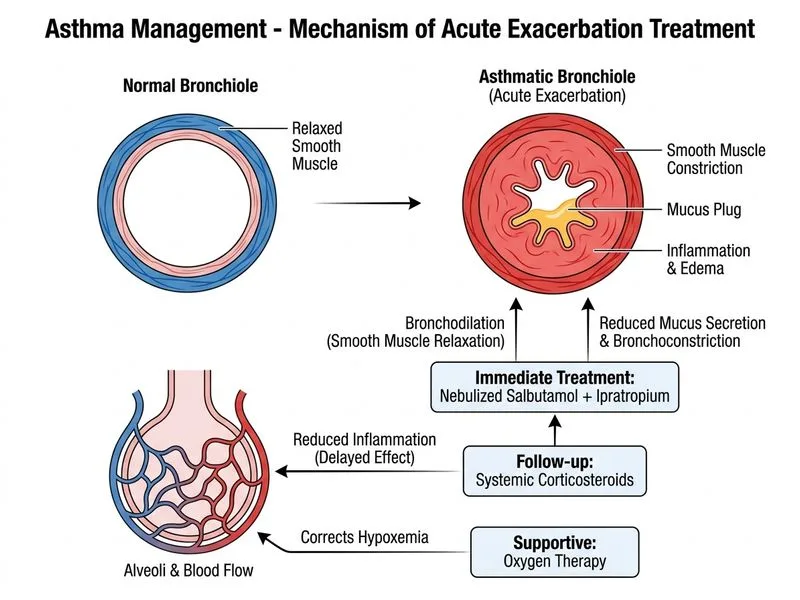
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.