## Epidermal Barrier Defect in Atopic Dermatitis **Key Point:** The primary pathophysiological defect in atopic dermatitis is impaired epidermal barrier function due to mutations and reduced expression of filaggrin (FLG) and other structural proteins. ### Filaggrin and Barrier Function Filaggrin is a crucial structural protein that: - Aggregates keratin filaments in the stratum corneum - Breaks down into natural moisturizing factors (NMF) that maintain hydration - Maintains tight junctions and corneodesmosomes **High-Yield:** Filaggrin gene mutations (FLG) are found in 20–30% of atopic dermatitis patients and are the strongest genetic risk factor. Loss-of-function mutations lead to: 1. Impaired barrier integrity 2. Increased transepidermal water loss (TEWL) 3. Enhanced allergen and irritant penetration 4. Secondary immune activation ### Why This Is Primary The "outside-in" hypothesis emphasizes that barrier dysfunction precedes immune dysregulation: - Defective barrier → increased TEWL → increased allergen penetration - Allergen exposure → innate immune activation → Th2 response - This contrasts with the older "inside-out" hypothesis (now secondary) ### Other Barrier Proteins Affected | Protein | Function | Status in AD | |---------|----------|-------------| | Filaggrin | Keratin aggregation, NMF production | **Reduced/mutated** | | Loricrin | Cornified envelope formation | Decreased | | Involucrin | Structural protein | Decreased | | Claudins | Tight junction proteins | Dysregulated | | Ceramides | Lipid barrier | Depleted | **Clinical Pearl:** This explains why atopic dermatitis patients benefit from frequent emollients and moisturizers — they compensate for the defective barrier by providing external hydration and lipid replacement. [cite:Robbins 10e Ch 25] 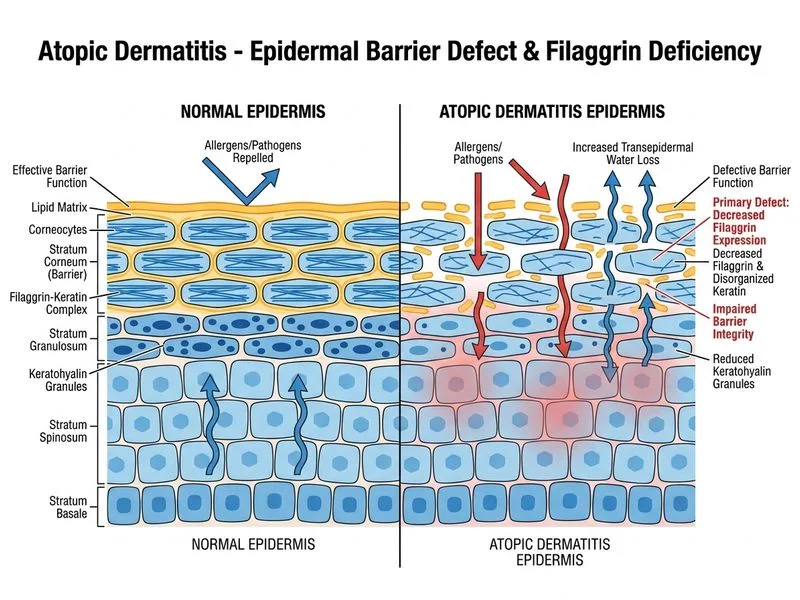
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.