## Distinguishing Atopic Dermatitis from Seborrheic Dermatitis ### Key Clinical Discriminator **Key Point:** The most reliable discriminating feature is the **character of scales, degree of pruritus, and anatomical distribution**: seborrheic dermatitis presents with **oily, yellowish, greasy scales** with **minimal to mild pruritus** and a **predilection for sebaceous gland-rich areas** (scalp, face, chest, intertriginous zones). Atopic dermatitis, conversely, causes intense pruritus with dry scales and affects flexural surfaces. ### Comparison Table | Feature | Atopic Dermatitis | Seborrheic Dermatitis | |---------|-------------------|----------------------| | **Scale Character** | Dry, fine, white scales | Oily, yellowish, greasy, waxy scales | | **Pruritus Intensity** | Severe, often unbearable; sleep-disturbing | Mild to moderate; often absent | | **Primary Distribution** | Flexural (antecubital, popliteal), face, neck | Scalp, face (T-zone), chest, intertriginous areas | | **Anatomical Basis** | Abnormal skin barrier, immune dysregulation | Malassezia yeast, sebaceous gland activity | | **Skin Appearance** | Dry, lichenified in chronic cases | Oily, erythematous with greasy scale | | **Associated Conditions** | Asthma, allergic rhinitis, food allergy | Parkinson's, HIV/AIDS, psoriasis | | **Response to Antifungals** | No response | Responds to azoles, selenium sulfide | | **Age of Onset** | Usually childhood (< 5 years) | Can occur at any age; often 20–40 years | ### Pathophysiological Basis **High-Yield:** Seborrheic dermatitis is driven by **Malassezia yeast** overgrowth in sebaceous gland-rich areas, whereas atopic dermatitis is a **Th2-mediated immune disorder** with a defective skin barrier (filaggrin mutations). This explains why seborrheic dermatitis responds to antifungals (ketoconazole, selenium sulfide) while atopic dermatitis does not. ### Clinical Pearl **Clinical Pearl:** A patient with greasy, yellowish scales on the scalp and nasolabial folds with minimal itching is seborrheic dermatitis until proven otherwise. Conversely, a patient with intense pruritus, dry skin, and lichenified flexural surfaces is atopic dermatitis. The **character of scales and degree of pruritus** are the quickest bedside discriminators. ### Mnemonic **Mnemonic: "GREASY SEB"** — **G**reasy scales, **R**ich in sebaceous areas, **E**asy (minimal pruritus), **A**ssociated with Malassezia, **S**kin is **E**asy to treat (antifungals), **Y** (yeast-driven); **S**eborrheic, **E**asy pruritus, **B**ased on yeast. ### Why Other Features Are Not Discriminators - **Intense pruritus and sleep disturbance:** While characteristic of atopic dermatitis, seborrheic dermatitis can also cause pruritus in some patients, making this not a reliable sole discriminator. - **Lichenification:** This is a chronic change specific to atopic dermatitis but does not occur in seborrheic dermatitis; however, lichenification is a sign of chronicity, not acute discrimination. - **Exacerbation with stress and seasonal variation:** Both conditions can be stress-exacerbated and show seasonal patterns; this is not discriminatory. 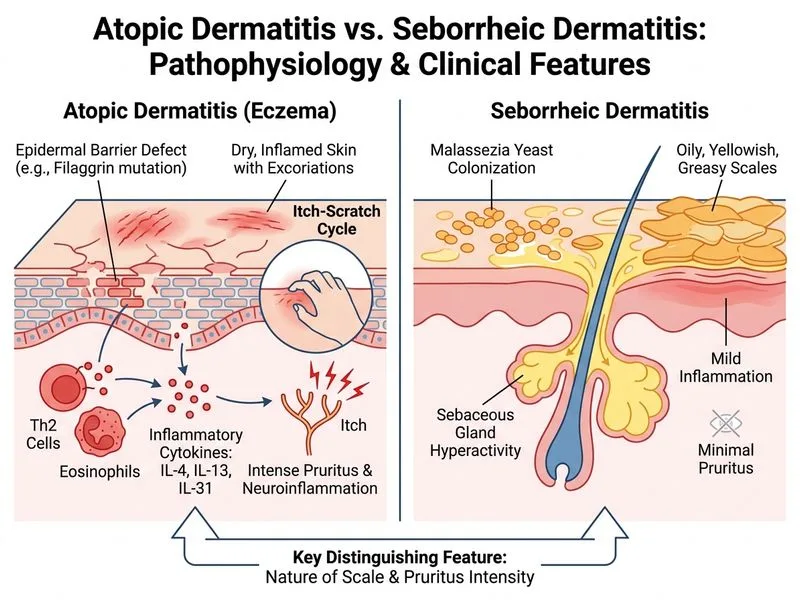
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.