## Diagnosis and Management of Atopic Dermatitis ### Clinical Presentation This child presents with classic features of atopic dermatitis (AD): - Age of onset: typically before 5 years (this child is 6) - Distribution: face, neck, and flexural surfaces (antecubital/popliteal fossae) - Symptoms: intense pruritus with lichenification and excoriation - Seasonal variation: worse in winter (dry climate) - Associated atopy: allergic rhinitis and family history of asthma - Elevated serum IgE **Key Point:** The Hanifin and Rajka criteria require 3 of 4 major criteria (pruritus, typical morphology/distribution, chronic/relapsing course, personal history of atopy) — this patient meets all. ### First-Line Topical Management **High-Yield:** Topical corticosteroids (TCS) are the gold standard first-line agents for acute flares of atopic dermatitis in children and adults [cite:Inamadar & Palit, IAD Guidelines]. | Agent | Potency | Indication | Onset | |-------|---------|-----------|-------| | Mometasone furoate 0.1% | Mild-to-moderate | First-line for face, neck, flexural areas | 3–5 days | | Triamcinolone acetonide 0.1% | Mild-to-moderate | Flexural dermatitis | 3–5 days | | Tacrolimus 0.03% | Steroid-sparing | Second-line; useful for steroid-sensitive areas (face) after initial TCS control | Slower onset | | Pimecrolimus | Mild | Maintenance; not for acute flares | Slower | **Clinical Pearl:** Mometasone furoate 0.1% is preferred for this child because: 1. It is a mild-to-moderate potency steroid suitable for children 2. It has rapid onset (3–5 days) for acute flare control 3. It is safe for use on the face and neck (unlike potent steroids) 4. It is cost-effective and widely available in India ### Why Tacrolimus Is NOT First-Line Here **Warning:** While topical tacrolimus 0.03% is effective and steroid-sparing, it is reserved for: - Steroid-dependent cases - Steroid-sensitive areas after initial TCS control - Maintenance therapy - NOT as first-line for acute flares (slower onset, higher cost) ### Adjunctive Measures - Emollients (frequent application): essential for all AD patients - Avoid irritants and allergens - Avoid excessive bathing; use lukewarm water - Systemic antihistamines if sleep disturbance **Mnemonic:** **SCAT** for AD management = **S**teroids (topical, first-line), **C**alcineurin inhibitors (steroid-sparing), **A**djuvant (emollients, antihistamines), **T**reatment of triggers. 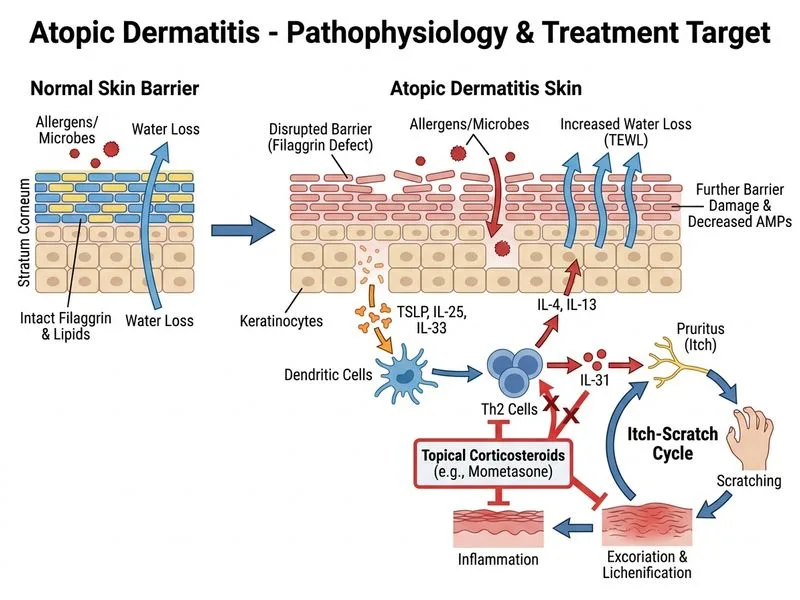
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.