## Diagnosis & Clinical Context **Key Point:** This is a classic presentation of **atopic dermatitis (AD)** in a child, evidenced by: - Age of onset (typically 2–5 years) - Characteristic distribution (flexural surfaces) - Intense pruritus with lichenification and xerosis - Dennie–Morgan fold (a hallmark sign) - Elevated serum IgE - Family history of atopy (father's allergic rhinitis) - Seasonal variation (worse in winter when humidity is low) ## First-Line Management Algorithm ```mermaid flowchart TD A[Atopic Dermatitis Flare]:::outcome --> B{Severity?}:::decision B -->|Mild to Moderate| C[Emollients + Topical Corticosteroid]:::action B -->|Severe/Widespread| D[Systemic Corticosteroid Short Course]:::action C --> E[Hydrocortisone 1% or Triamcinolone 0.1%]:::action D --> F[Prednisolone 0.5-1 mg/kg/day × 1-2 weeks]:::action E --> G[Twice daily + emollients]:::action F --> G G --> H[Review in 1-2 weeks]:::outcome ``` ## Why Topical Corticosteroid Is Correct **High-Yield:** For **mild-to-moderate acute flares** in children, the evidence-based first-line approach is: 1. **Emollients** (moisturizers) — foundation of all AD management 2. **Topical corticosteroid** — rapid anti-inflammatory effect - Hydrocortisone 1% (Class VII, safest for face/neck/intertriginous areas) - Triamcinolone 0.1% (Class IV, for body) - Apply twice daily for 1–2 weeks, then taper **Clinical Pearl:** Topical corticosteroids are the gold standard for localized AD because they: - Act within 24–48 hours - Minimize systemic absorption (especially with hydrocortisone) - Are safe for long-term use in children when used correctly - Reduce pruritus and allow skin barrier repair **Key Point:** Emollients must accompany topical steroids — they repair the impaired skin barrier (defective filaggrin, ceramide loss) that is fundamental to AD pathogenesis. ## Steroid Potency & Pediatric Safety | Potency Class | Agent | Pediatric Use | Notes | |---|---|---|---| | VII (Weakest) | Hydrocortisone 1% | Safe, face/neck | First-line for mild AD | | IV | Triamcinolone 0.1% | Safe, short-term | Body/trunk | | II–III | Clobetasol, Betamethasone | Avoid in children | Risk of atrophy, HPA axis suppression | **Mnemonic: STEP-UP** — **S**teroids (topical first), **T**acrolimus (if steroid-sparing needed), **E**mollients (always), **P**hototherapy (severe), **U**pdate with systemic agents (last resort), **P**robiotic/allergen avoidance (adjunctive). ## Why This Child Does NOT Need Systemic Corticosteroids Yet Although his AD is chronic and moderately severe (lichenification, widespread), the lesions are: - Localized to flexural areas (not generalized) - Responsive to seasonal factors (suggesting environmental control is possible) - Not described as acute, severe, or unresponsive to topical therapy Systemic corticosteroids (prednisolone) are reserved for: - Severe, acute flares with widespread involvement - Failure of topical therapy after 2–4 weeks - Risk of rebound flare upon discontinuation [cite:Irvine et al. (AAD/AADA Guidelines) 2016; Sharma et al. (IADVL) 2019] 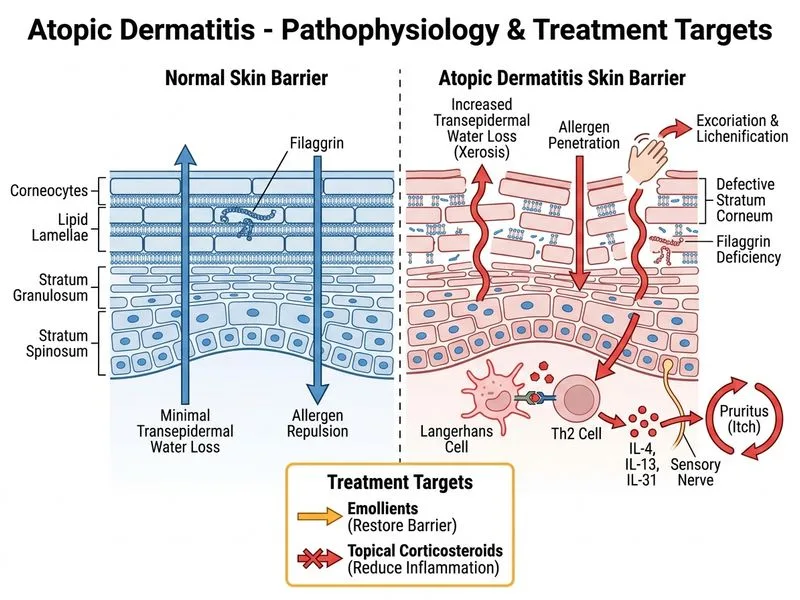
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.