## Clinical Diagnosis This patient has **atopic dermatitis (AD)** based on: - Chronic, relapsing course (3 years) - Pruritus-dominant presentation - Flexural and facial involvement - Lichenification (chronic scratching) - Seasonal pattern (worse in winter—dry air, low humidity) - Negative prick testing (rules out IgE-mediated contact allergy) - Family history of atopy (daughter affected) ## Pathophysiology of Atopic Dermatitis ### The Filaggrin Defect: Central Mechanism **High-Yield:** Loss-of-function mutations in the **FLG gene** (filaggrin) are the most important genetic risk factor for atopic dermatitis. Filaggrin is a key structural protein in the stratum corneum that: 1. **Aggregates keratin filaments** → maintains mechanical strength 2. **Breaks down into natural moisturizing factors (NMF)** → maintains hydration 3. **Maintains skin pH** → supports antimicrobial barrier ### Consequence: Impaired Barrier Function ```mermaid flowchart TD A[FLG mutation or reduced expression]:::outcome --> B[Decreased filaggrin protein]:::outcome B --> C[Defective stratum corneum structure]:::outcome C --> D[Increased transepidermal water loss TEWL]:::outcome D --> E[Dry skin xerosis]:::outcome E --> F[Increased penetration of irritants & allergens]:::action F --> G[Innate immune activation]:::action G --> H[Th2-skewed adaptive immunity]:::action H --> I[IL-4, IL-5, IL-13 production]:::outcome I --> J[IgE elevation & mast cell sensitization]:::outcome J --> K[Pruritus & inflammation]:::urgent ``` **Key Point:** The **"outside-in" hypothesis** of AD pathogenesis emphasizes that the primary defect is barrier dysfunction, not primary immune dysregulation. Barrier impairment allows allergen and irritant penetration, which then triggers secondary Th2 immune activation. ### Why Filaggrin Deficiency Explains This Patient's Features | Feature | Mechanism | |---------|----------| | Xerosis (dry skin) | Loss of NMF and increased TEWL | | Seasonal worsening | Low humidity in winter increases TEWL | | Pruritus | Irritant penetration; nerve fiber upregulation | | Lichenification | Chronic scratching response to barrier dysfunction | | Negative prick test | Primary defect is barrier, not IgE-mediated allergy | | Family history | FLG mutations are inherited (autosomal dominant) | ## Role of Secondary Immune Dysregulation **Clinical Pearl:** While filaggrin defects initiate AD, secondary Th2-skewed immune responses (elevated IgE, IL-4, IL-5) perpetuate inflammation. However, these are **consequences**, not the primary driver. ## Why NOT the Other Options? ### Option 1: IgE-Mediated Mast Cell Degranulation - **Trap:** AD does involve elevated IgE and mast cell involvement, but this is **secondary** to barrier dysfunction. - **Key distinction:** Prick testing is **negative**, indicating no IgE-mediated sensitization to common allergens. - The primary defect is barrier impairment, not allergic sensitization. ### Option 2: Delayed-Type Hypersensitivity (Contact Dermatitis) - **Trap:** AD can coexist with contact dermatitis, but the patient denies occupational exposure and has negative prick testing. - Contact dermatitis is a Th1-mediated response; AD is Th2-mediated. - The distribution (hands, wrists, face) and seasonal pattern fit AD, not occupational contact dermatitis. ### Option 3: Sebaceous Gland Dysfunction - **Trap:** AD is characterized by **lipid depletion** in the stratum corneum, but this is due to barrier defects (including filaggrin loss), not sebaceous gland pathology. - Sebaceous glands are not the primary source of stratum corneum lipids; they contribute to skin surface lipids. - This mechanism does not explain the genetic basis or family history. ## Clinical Implications **High-Yield:** Understanding filaggrin deficiency explains why AD management focuses on: - **Barrier repair:** Frequent emollients with ceramides, cholesterol, and free fatty acids (mimic healthy SC lipids) - **Avoiding irritants:** Harsh soaps, detergents worsen barrier dysfunction - **Topical corticosteroids:** Reduce secondary inflammation - **Calcineurin inhibitors:** Steroid-sparing option for maintenance [cite:Robbins & Cotran Pathologic Basis of Disease 10e Ch 25; Harrison's Principles of Internal Medicine 21e Ch 319] 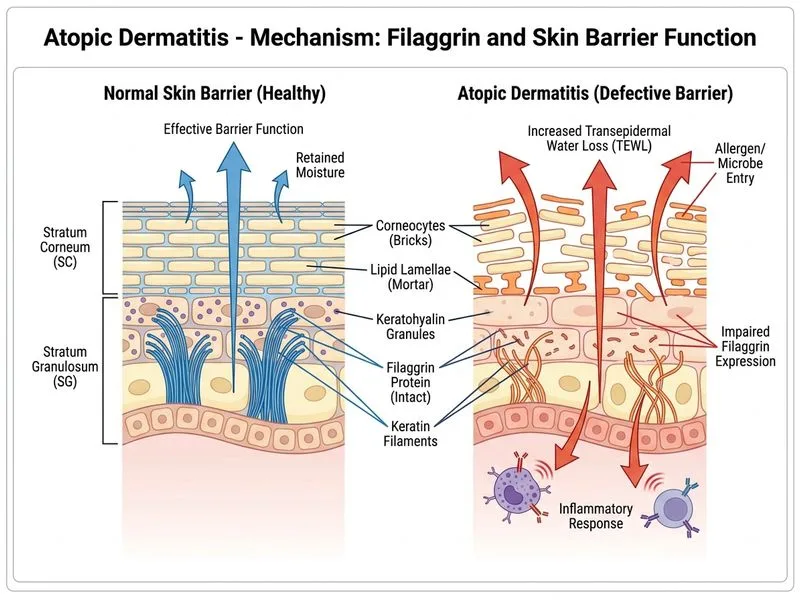
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.