## Management of Acute Atopic Dermatitis Flare ### Clinical Context **Key Point:** This patient has a moderate-to-severe acute flare (40% BSA involvement) with secondary bacterial infection. Management must address inflammation, pruritus, barrier dysfunction, and infection. ### Stepwise Management Hierarchy ```mermaid flowchart TD A["Acute AD Flare<br/>(40% BSA, oozing, crusting)"]:::outcome --> B{"Assess severity<br/>& infection"}:::decision B -->|"Moderate-severe<br/>+ bacterial signs"| C["Step 1: Emollients<br/>(frequent, liberal)"]:::action C --> D["Step 2: Topical corticosteroids<br/>(potent, e.g., clobetasol)<br/>on inflamed areas"]:::action D --> E{"Bacterial infection<br/>present?"}:::decision E -->|"Yes (golden crusts,<br/>oozing)"| F["Oral antibiotics<br/>(anti-staphylococcal)<br/>+ topical antiseptic"]:::action E -->|"No"| G["Monitor & reassess<br/>in 1–2 weeks"]:::outcome F --> H{"Response<br/>adequate?"}:::decision H -->|"Yes"| I["Continue topical therapy<br/>+ maintenance emollients"]:::action H -->|"No / Severe"| J["Consider systemic<br/>corticosteroids or<br/>calcineurin inhibitors"]:::action ``` ### First-Line Approach: The Stepwise Ladder | Step | Intervention | Indication | Notes | |------|--------------|-----------|-------| | **1** | **Emollients** | All AD patients, all flares | Ceramide-rich, fragrance-free; apply within 3 min of bathing | | **2** | **Topical corticosteroids** | Inflamed areas (erythema, oozing) | Potency matched to severity; face/neck = mild-moderate; trunk = potent | | **3** | **Oral antibiotics** | Secondary bacterial infection | *S. aureus* most common; flucloxacillin or cephalexin | | **4** | **Systemic corticosteroids** | Severe flares failing topical therapy | Short course (7–14 days); taper to avoid rebound | | **5** | **Calcineurin inhibitors** | Steroid-sparing; face/neck (avoid atrophy) | Tacrolimus, pimecrolimus; slower onset than steroids | | **6** | **Phototherapy** | Chronic, maintenance phase | Not first-line for acute flares; requires 2–3 weeks | ### Why This Patient Needs Emollients + Topical Corticosteroids + Antibiotics **High-Yield:** The "itch-scratch-infection" cycle in this case requires: 1. **Emollients** — restore barrier function, reduce TEWL, decrease itch 2. **Topical corticosteroids** — suppress inflammation and pruritus rapidly 3. **Oral antibiotics** — treat/prevent *Staphylococcus aureus* superinfection (evidenced by golden crusts) **Clinical Pearl:** Secondary bacterial infection is common in acute AD flares due to impaired barrier and scratching. Golden crusts, oozing, and pustules warrant anti-staphylococcal coverage (flucloxacillin 500 mg QID or cephalexin 500 mg QID for 7–10 days). ### Why NOT Systemic Corticosteroids as First-Line? **Warning:** Although systemic corticosteroids work quickly, they are NOT first-line for acute flares because: - Topical therapy is often sufficient for localized/moderate flares - Systemic steroids carry risk of rebound flare upon withdrawal - Systemic steroids do not address barrier dysfunction (emollients do) - Reserve systemic steroids for severe, widespread flares failing topical therapy **Tip:** If systemic steroids are used, keep the course short (7–14 days) and taper gradually to avoid rebound. ### Why NOT Calcineurin Inhibitors as First-Line? - Slower onset (2–3 weeks) compared to topical corticosteroids - Useful as **steroid-sparing agents** on face/neck (to avoid skin atrophy) - Better for maintenance, not acute flares - Often used in combination with topical steroids, not as monotherapy ### Why NOT Phototherapy or Immunosuppressants? - **Phototherapy (UVB):** Requires 2–3 weeks for effect; not suitable for acute flares. Reserved for chronic, maintenance phase. - **Immunosuppressants (azathioprine, cyclosporine):** Reserved for severe, refractory AD unresponsive to topical therapy and phototherapy. Not first-line. - **Systemic retinoids:** Not indicated for AD; used in other dermatoses (e.g., severe psoriasis). ### Mnemonic: **BEAT** (Acute AD Flare Management) - **B** — Barrier repair (emollients, ceramides) - **E** — Emollients (frequent, liberal application) - **A** — Anti-inflammatory (topical corticosteroids) - **T** — Treat infection (oral antibiotics if bacterial signs present) 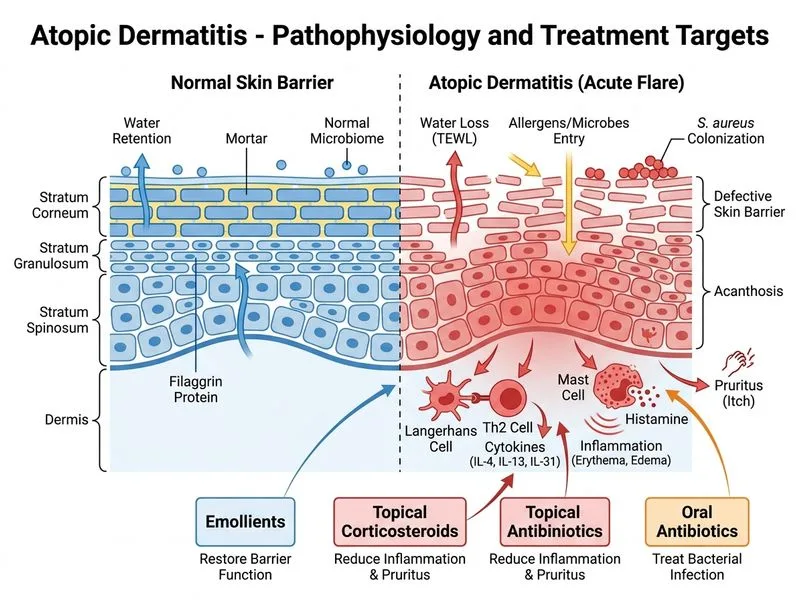
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.