## Primary Pathophysiology of Atopic Dermatitis **Key Point:** The fundamental defect in atopic dermatitis is a **compromised epidermal barrier** due to loss-of-function mutations in the filaggrin (FLG) gene, which encodes a critical structural protein in the stratum corneum. ### Filaggrin and Barrier Dysfunction Filaggrin is essential for: - Aggregation of keratin filaments in corneocytes - Formation of a competent stratum corneum - Maintenance of skin hydration and prevention of transepidermal water loss (TEWL) **High-Yield:** Filaggrin mutations are present in 20–30% of atopic dermatitis patients and are the strongest genetic risk factor identified to date. This explains the characteristic xerosis (dry skin) and increased susceptibility to secondary infections in AD. ### Secondary Immune Dysregulation The impaired barrier allows: 1. Increased antigen penetration 2. Enhanced Th2 cytokine response (IL-4, IL-5, IL-13) 3. Elevated serum IgE levels **Clinical Pearl:** Although IgE elevation is common in AD, it is a *secondary* consequence of barrier dysfunction and allergic sensitization, not the primary defect. This is why barrier repair (emollients, ceramides) is the foundation of AD management. ### Why Barrier Repair Comes First The "outside-in" model of AD pathogenesis emphasizes that restoring the physical barrier (through ceramide-rich moisturizers and gentle cleansing) is often sufficient to reduce inflammation and prevent flares, even before immunosuppressive therapy. 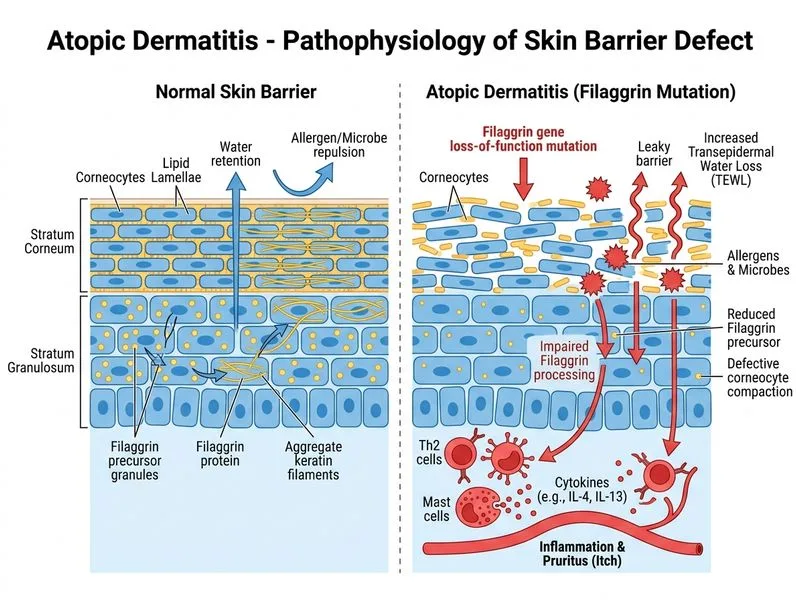
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.