## Clinical Presentation Analysis **Key Point:** This patient has multiple features of **atopic dermatitis (AD)** with acute exacerbation, not primary contact dermatitis: - Personal history of atopy (allergic rhinitis) - Family history of atopy (asthma) - Elevated serum IgE (280 IU/mL) - **Negative patch test** (rules out allergic contact dermatitis) - Distribution on hands/forearms (common site for AD in adults) - Acute vesicles and oozing (acute phase AD) ## Differential Diagnosis: Eczema Types | Feature | Atopic Dermatitis | Irritant Contact | Allergic Contact | Dyshidrotic | |---------|-------------------|------------------|------------------|-------------| | **Patch test** | Negative | Negative | **Positive** | Negative | | **Personal atopy** | **Yes** | No | No | Variable | | **Family history** | **Yes** | No | No | No | | **Serum IgE** | **Elevated** | Normal | Normal | Normal | | **Onset** | Chronic relapsing | Acute after exposure | 48–72 hrs after exposure | Seasonal/stress-related | | **Demarcation** | Ill-defined | Well-defined | Well-defined | Ill-defined | | **Response to TCS** | Good | Good | Good | Variable | ## Pathogenic Mechanism of AD ```mermaid flowchart TD A[Genetic Predisposition]:::outcome --> B[FLG Mutations + Atopy Genes]:::outcome B --> C[Impaired Skin Barrier Function]:::action C --> D[Increased Transepidermal Water Loss]:::action D --> E[Allergen & Irritant Penetration]:::action E --> F[Dendritic Cell Activation]:::action F --> G[Th2 Polarization]:::action G --> H[IL-4, IL-5, IL-13 Production]:::action H --> I[IgE Elevation]:::outcome I --> J[Mast Cell Degranulation]:::action J --> K[Pruritus & Inflammation]:::urgent K --> L[Scratching → Barrier Damage Cycle]:::urgent ``` **High-Yield:** AD is fundamentally a **Th2-mediated, IgE-associated inflammatory disorder** with: 1. **Genetic component:** Filaggrin (FLG) mutations → impaired barrier 2. **Immune dysregulation:** Th2 skewing → IL-4, IL-5, IL-13 overproduction 3. **Elevated IgE:** Supports Th2 phenotype (though not diagnostic alone) 4. **Barrier dysfunction:** Increased TEWL → secondary irritant penetration ## Why Other Options Are Incorrect **Irritant contact dermatitis:** While hand-washing is a risk factor, the presence of: - Elevated IgE - Personal + family atopy history - Negative patch test ...makes AD the primary diagnosis. Irritant dermatitis is a **diagnosis of exclusion** in atopic individuals and does not explain the systemic IgE elevation or familial pattern. **Allergic contact dermatitis:** **Negative patch test definitively excludes this diagnosis.** Allergic contact dermatitis requires Type IV hypersensitivity (sensitization to a specific hapten) and would show positive patch test reaction. **Dyshidrotic eczema:** This is a subset of AD presenting with vesicular morphology, often on palms/soles. However, it is NOT a distinct entity but rather **a morphologic variant of AD** in genetically predisposed individuals. The diagnosis here is still AD; dyshidrotic eczema is the clinical phenotype. **Clinical Pearl:** In an atopic patient with hand dermatitis, **occupational irritant exposure exacerbates underlying AD** rather than causing primary irritant dermatitis. Management requires both barrier repair and immune modulation, not just irritant avoidance. **Mnemonic for AD Diagnosis — "ATOPY":** - **A**topy history (personal or family) - **T**est negative (patch test negative) - **O**nset early (usually childhood, but can persist/relapse in adulthood) - **P**ruritis intense and chronic - **Y**ield to topical corticosteroids and calcineurin inhibitors 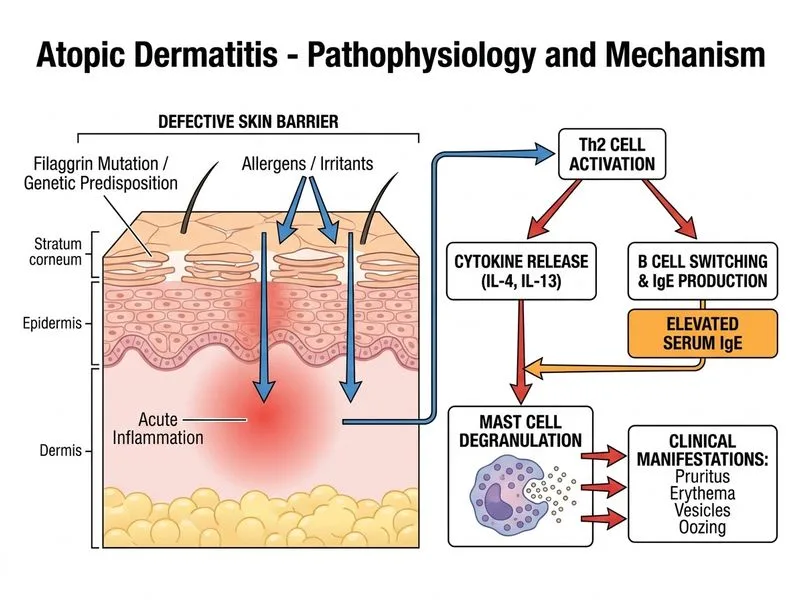
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.