## Diagnosis of Atopic Dermatitis ### Clinical Diagnosis is Gold Standard **Key Point:** Atopic dermatitis (AD) is primarily a clinical diagnosis. There is no single pathognomonic laboratory test or imaging study that confirms AD. The diagnosis rests on clinical history, examination findings, and the presence of major and minor criteria. ### Hanifin and Rajka Criteria The patient must meet **3 of 4 major criteria** for diagnosis: | Major Criteria | Minor Criteria | |---|---| | Pruritus (essential) | Elevated serum IgE | | Typical morphology and distribution (flexural surfaces in children) | Early age of onset | | Chronic or relapsing course | Dry skin (xerosis) | | Personal history of atopy (asthma, allergic rhinitis, food allergy) | Recurrent skin infections | **High-Yield:** This patient meets **all 4 major criteria**: pruritus, flexural distribution (typical for children), chronic course (2 years), and personal history of atopy (allergic rhinitis). ### Why Laboratory Tests Are Not Diagnostic **Clinical Pearl:** Elevated serum IgE and positive skin prick tests are **supportive but not diagnostic**. Many atopic individuals have elevated IgE without AD, and many AD patients have normal IgE levels. These tests help identify triggers but do not confirm the diagnosis. **Warning:** Patch testing is used to identify contact allergens in contact dermatitis, not atopic dermatitis. It is not indicated here. ### Summary The diagnosis of AD is **clinical** — based on history, examination, and criteria. Investigations (IgE, skin prick test) may be helpful in identifying triggers and associated atopy but are **not confirmatory** for the diagnosis itself. 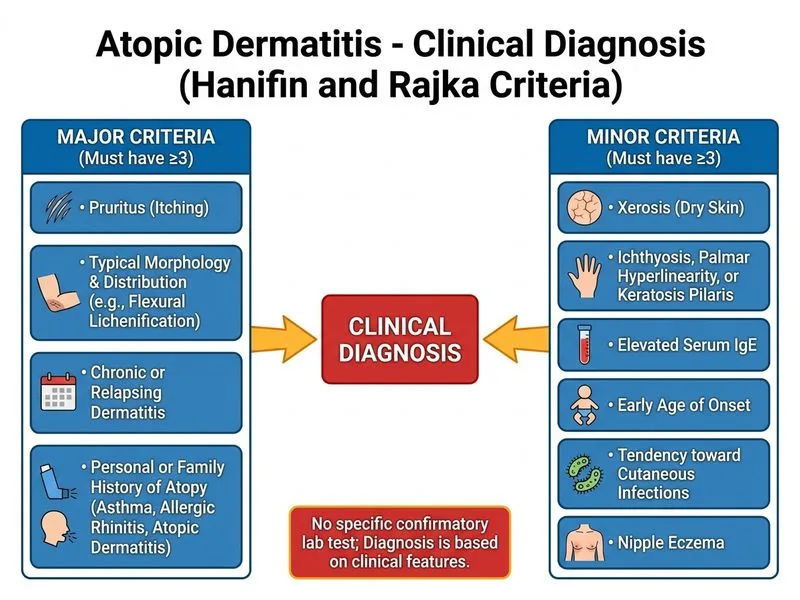
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.